📞Customer Service: +86 13248368268 📧servicecenter@suzhoufrank.com one year replacement and warranty!
Medical Simulation in Endoscopy and Gastrointestinal (GI) Training: Complete Guide
Complete guide to medical simulation for endoscopy training. Learn about medical simulator types , training applications and competency-based education integration.
MEDICAL TRAINING
Dr Qi Rui
1/16/202610 min read
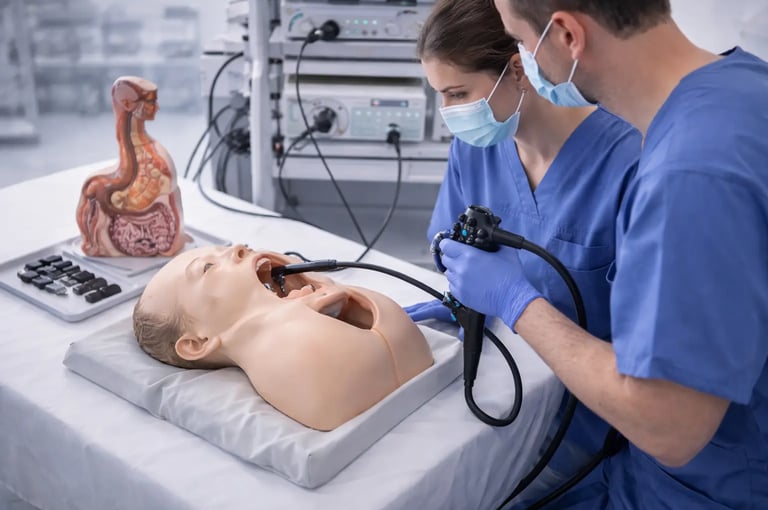
The landscape of medical education has fundamentally changed. Where physicians once learned procedural skills exclusively on patients , today's training programs increasingly rely on medical simulation to build competence before clinical exposure. Nowhere is this shift more evident than in endoscopy and gastrointestinal training , where the technical demands of procedures and the imperative of patient safety have driven widespread adoption of simulation-based education.
This comprehensive guide explores what medical simulation means in the context of endoscopy and GI training , the types of medical simulators available , who uses them , and how they integrate into modern competency-based education programs.
Understanding Medical Simulation in Healthcare
Medical simulation refers to the use of artificial environments , models , and technologies to replicate clinical scenarios for educational purposes. The goal is straightforward: allow learners to develop , practice , and refine clinical skills in settings where errors carry no patient risk.
The Society for Simulation in Healthcare , the world's largest organization dedicated to healthcare simulation , defines the field as encompassing technologies and methodologies that improve patient safety and provider performance while reducing costs and medical errors. Their work has established standards , certifications and accreditation processes that guide simulation programs globally.
In endoscopy specifically , medical simulation addresses a fundamental challenge. Endoscopic procedures require simultaneous mastery of complex psychomotor skills , anatomical knowledge , clinical decision-making and complication management. Traditional apprenticeship models , where trainees learn by doing procedures on patients under supervision , create tension between educational needs and patient welfare.
A medical simulator bridges this gap. Trainees can attempt procedures repeatedly , make mistakes , receive feedback and build muscle memory , all without any patient ever being at risk. The learning environment becomes safer for everyone involved.
For those new to this field , understanding endoscopy simulators provides essential foundation. What distinguishes simulation-based training from traditional approaches is the opportunity for deliberate practice , the ability to encounter rare scenarios on demand , and objective assessment of performance.
The Evolution of Simulation in GI Training
Endoscopy simulation has progressed dramatically since its origins. Early efforts involved simple mechanical models that allowed scope manipulation practice. These basic trainers served limited purposes but established the principle that procedural skills could be developed outside the clinical setting.
The introduction of computer-based virtual reality systems transformed possibilities. Suddenly , trainees could navigate virtual anatomy , encounter pathology , perform interventions and receive immediate performance feedback. These systems brought standardization to training that varied greatly between institutions.
Research has consistently demonstrated that simulation training transfers to improved clinical performance. Studies show that trainees who complete structured simulation curricula achieve competence faster , perform procedures more safely and cause less patient discomfort than those trained through observation alone. The evidence base supporting simulation has grown sufficiently robust that major professional organizations now explicitly incorporate simulation into training recommendations.
The American Society for Gastrointestinal Endoscopy (ASGE) has published guidance on principles of endoscopic training that specifically addresses incorporating simulators into endoscopy teaching. Their white papers recognize simulation as integral to modern training rather than optional supplementation.
Types of Medical Simulators for Endoscopy Training
Understanding the categories of medical simulators helps programs select appropriate tools for specific training objectives. Each type offers distinct advantages and limitations.
Mechanical or Physical Models
Physical models provide tangible , hands-on training experiences. These range from simple scope manipulation trainers to anatomically accurate organ models that allow practice of specific techniques.
Box trainers create enclosed spaces where trainees manipulate instruments while viewing their work on monitors , replicating the hand-eye coordination demands of actual endoscopy. These relatively inexpensive devices excel at building basic psychomotor skills.
Anatomical models replicate specific organs or anatomical regions. A gastrointestinal endoscopy simulator provides realistic tissue representation for practicing navigation , visualization and basic diagnostic techniques. These models allow trainees to understand three-dimensional anatomy in ways that diagrams and videos cannot convey.
Explanted tissue models use animal organs to provide highly realistic tissue properties. While offering excellent fidelity , these models require special handling , have limited reuse potential and raise some ethical considerations that programs must address.
Virtual Reality Simulators
Virtual reality (VR) medical simulators use computer graphics and haptic feedback devices to create immersive procedural experiences. Trainees manipulate controls that provide force feedback while viewing computer-generated anatomical environments on screens.
VR simulators offer several advantages. They can present unlimited case variety , including rare pathology and complications that trainees might not encounter for years in clinical practice. They provide objective metrics: procedure time , scope tip position , forces applied to virtual tissue , completeness of examination and numerous other parameters that allow precise performance tracking.
Validated VR platforms exist for upper endoscopy , colonoscopy , ERCP , EUS and other GI procedures. These systems have demonstrated construct validity , meaning they distinguish between novice and expert performers , and transfer validity , meaning skills acquired on simulators improve actual clinical performance.
The limitation of VR systems is cost. High-fidelity platforms require substantial investment in hardware , software licensing and ongoing maintenance. For many programs , these costs necessitate careful consideration of which procedures warrant VR training investment.
Hybrid Simulators
Hybrid simulators combine physical models with virtual or augmented reality components. A trainee might manipulate a real endoscope through a physical model while viewing computer-enhanced imagery that adds virtual pathology , bleeding or other clinical scenarios to the physical environment.
These systems attempt to capture benefits of both approaches: the realistic tactile experience of physical models with the case variety and metrics of virtual systems. Development in this space continues rapidly as technologies mature.
Task Trainers
Task trainers focus on specific procedural components rather than complete procedures. Instead of simulating an entire colonoscopy , a task trainer might isolate polypectomy technique , hemostasis maneuvers or specific therapeutic interventions.
This modular approach aligns well with competency-based education principles. Trainees can focus intensive practice on specific skills where they need development without spending time on components they've already mastered.
For therapeutic techniques , specialized simulators address specific training needs. Our gastrointestinal ESD surgical simulator allows practice of endoscopic submucosal dissection , a technically demanding procedure that requires extensive training before clinical application.
Simulation Across Related Specialties
While this guide focuses on gastrointestinal applications , medical simulation principles extend across endoscopic specialties. Understanding the broader landscape helps programs recognize transferable concepts and shared resources.
Bronchoscopy Simulation
Pulmonary endoscopy training faces similar challenges to GI training. Bronchoscopy requires scope navigation skills , anatomical recognition and therapeutic competencies that benefit from simulation-based development.
Our bronchoscopy simulator options range from basic navigation trainers to comprehensive intervention systems. The endoscopy bronchoscopy simulator provides realistic airway anatomy for diagnostic bronchoscopy training , while more advanced configurations support therapeutic skill development.
Urological Endoscopy
Urological procedures including cystoscopy , ureteroscopy and percutaneous approaches have their own simulation training needs. A urological endoscopy simulator addresses the unique anatomical and technical requirements of urinary tract endoscopy.
Laparoscopic Training
Though not strictly endoscopy , laparoscopic simulation shares many principles with endoscopic training. Both require development of hand-eye coordination for instrument manipulation while viewing monitors. Our laparoscopy simulator allows surgical trainees to develop foundational skills applicable across minimally invasive approaches.
Gynecological Endoscopy
Hysteroscopy training benefits from simulation before clinical procedures. A hysteroscopy simulator provides safe skill development for a procedure commonly performed by gynecologists and reproductive specialists.
Who Uses Medical Simulation in GI Training?
Medical simulation serves diverse learners across the educational continuum. Understanding these populations helps programs design appropriate curricula.
Medical Students
Increasingly , medical schools incorporate simulation into gastroenterology rotations. Students gain exposure to endoscopic concepts and basic scope handling before clinical clerkships. This early exposure helps students understand what gastroenterologists do and may influence specialty selection.
For medical students , simulation objectives typically emphasize understanding rather than competence. Students should appreciate endoscopy's role in patient care , understand basic anatomy and recognize that procedural mastery requires years of dedicated training.
Internal Medicine Residents
Internal medicine residents receive varying exposure to endoscopy depending on program structure and available rotations. Simulation can supplement limited clinical opportunities and standardize experiences across programs.
Resident training in GI increasingly incorporates simulation to maximize learning efficiency during gastroenterology rotations.
Gastroenterology Fellows
GI fellows represent the primary audience for intensive endoscopic simulation training. Fellowship programs must develop competent , independent endoscopists within structured timeframes. Simulation accelerates skill acquisition and provides assessment tools for competency verification.
Current ACGME requirements establish minimum procedure numbers for fellowship completion , but the field increasingly recognizes that numbers alone don't guarantee competence. Simulation-based assessment offers objective competency evaluation independent of case volume.
Fellowship training programs use simulation for multiple purposes: early skill development before patient contact , deliberate practice of challenging techniques , exposure to rare scenarios and objective progress assessment.
Advanced Endoscopy Fellows
Fourth-year fellows pursuing advanced therapeutic endoscopy face even steeper learning curves. ERCP , EUS , endoscopic resection and other complex procedures carry higher complication risks that make simulation training particularly valuable.
Fellowship programs in advanced endoscopy increasingly mandate simulation training as foundational preparation before supervised clinical procedures.
Practicing Endoscopists
Simulation isn't exclusively for trainees. Practicing endoscopists use simulation for skill maintenance , new technique acquisition and preparation for challenging cases. Continuing medical education increasingly incorporates hands-on simulation components.
When new devices or techniques emerge , simulation provides safe familiarization before clinical adoption. Practicing physicians can work through learning curves on simulators rather than patients.
Nurses and Endoscopy Technicians
Comprehensive endoscopy training extends beyond physicians. Nurses and technicians involved in endoscopy suite operations benefit from simulation that helps them understand procedures , anticipate physician needs and recognize complications.
Integrating Simulation into Competency-Based Training
Modern medical education has shifted toward competency-based frameworks. Rather than assuming that completing defined rotations or procedure numbers ensures competence , programs now directly assess whether trainees can perform expected tasks independently.
Medical simulation supports competency-based education powerfully. Simulators provide standardized assessment environments where all trainees face identical scenarios. Performance metrics enable objective comparison against established benchmarks. Assessment occurs without time pressure from waiting patients or clinical demands.
Milestones and Progression
Competency frameworks define developmental milestones that trainees should achieve at specific training stages. For endoscopy , these milestones might address technical skills (scope navigation , mucosal inspection , therapeutic maneuvers) , cognitive abilities (lesion recognition , clinical decision-making) and professional behaviors (informed consent , complication communication).
Competency training in endoscopy uses milestones to guide structured progression from novice to independent practitioner.
Simulation enables milestone assessment through standardized scenarios. All trainees attempting a milestone assessment face identical virtual or simulated cases , eliminating variability that makes clinical assessment inconsistent.
Curriculum Design
Effective simulation training requires intentional curriculum design , not just simulator availability. Random practice on available equipment produces inferior results compared to structured curricula that sequence content appropriately , provide focused feedback and require demonstrated competency before progression.
Designing simulation curricula for endoscopy programs involves identifying learning objectives , selecting appropriate simulation modalities , establishing practice schedules , creating assessment rubrics and training faculty in simulation-based teaching methods.
Skills Assessment
Assessment represents simulation's most powerful contribution to competency-based education. Traditional assessment relies heavily on subjective evaluations by supervising physicians who may observe only portions of procedures and bring varying standards.
Skills assessment through simulation offers standardization. Computerized systems can measure parameters consistently across all assessment attempts. Pre-defined criteria eliminate inter-rater variability. Trainees receive specific , actionable feedback rather than general impressions.
Evidence Supporting Simulation Training
The research supporting medical simulation in endoscopy training has grown substantially. Multiple randomized controlled trials demonstrate that simulation-trained fellows achieve competence faster and perform better on clinical metrics than traditionally trained peers.
The ASGE EndoVators Summit brought together thought leaders in simulation research to review evidence and establish priorities. Their white paper documents the strong foundation supporting simulation integration while identifying areas requiring further investigation.
Key findings from simulation research include: trainees who complete simulation curricula before clinical procedures cause less patient discomfort and achieve better outcomes; simulation training reduces learning curve length for new techniques; simulation-based assessment predicts clinical performance; and simulation training is cost-effective when considering reduced complication rates and improved efficiency.
The evidence base continues expanding as more programs incorporate simulation and publish outcomes. What began as innovative pilot projects has become standard of care in leading training programs.
Selecting Simulators for Your Program
Programs considering medical simulator acquisition face numerous options at varying price points. Several factors guide appropriate selection.
Training Objectives
What skills must the simulator develop? Basic scope manipulation requires different equipment than therapeutic technique training. Programs should map simulator capabilities to specific curricular objectives.
For comprehensive GI training programs , exploring GI simulator options helps identify systems matching program needs. Different simulators excel at different tasks , and most programs benefit from multiple simulator types serving complementary purposes.
Trainee Population
Who will use the simulator? A fellowship program with six trainees has different needs than a continuing education center serving hundreds of practitioners annually. Usage volume affects maintenance requirements , software licensing costs and space allocation.
Available Resources
Budget constraints affect all purchasing decisions. High-fidelity VR systems cost substantially more than mechanical trainers but offer capabilities simpler systems cannot match. Programs must balance ideal capabilities against fiscal realities.
Space requirements vary considerably. Some simulators require dedicated rooms with specialized ventilation and equipment. Others fit into existing spaces with minimal modification.
Technical support needs also vary. Complex computer-based systems require IT support for maintenance and troubleshooting. Simpler mechanical models need less technical expertise but may require consumable replacement.
Faculty Expertise
Simulators alone don't create effective training programs. Faculty must understand simulation pedagogy: how to structure practice sessions , provide effective feedback and assess performance meaningfully. Programs lacking simulation-trained faculty should plan for faculty development alongside equipment acquisition.
Clinical simulation in GI requires faculty who understand both clinical endoscopy and educational principles specific to simulation-based training.
The Future of Medical Simulation in GI Training
Medical simulation continues evolving rapidly. Several trends will shape its future in endoscopy education.
Artificial Intelligence Integration
AI systems are beginning to provide real-time feedback during simulated procedures. Rather than receiving performance summaries after sessions , trainees may receive guidance during procedures about technique , positioning and decision-making. These systems promise more efficient learning through immediate correction.
Extended Reality Technologies
Virtual and augmented reality technologies continue advancing. Future systems may provide more immersive experiences with improved visual fidelity , more realistic haptics and better integration with physical components.
Portable and Accessible Systems
Current high-fidelity simulators require dedicated facilities. Future systems may become more portable , allowing simulation training in clinical settings , conference locations or even trainees' homes. Accessibility improvements could democratize simulation training beyond well-resourced academic centers.
Assessment Integration
Simulation-based assessment may become standard for certification and credentialing decisions. Rather than relying on training program attestations , licensing bodies might require demonstrated performance on standardized simulation assessments.
Procedure-Specific Developments
As therapeutic endoscopy grows more complex , simulation for specific procedures will expand. Current simulators address common procedures well but may inadequately prepare trainees for emerging techniques. Continued development will address these gaps.
For colonoscopy training specifically , understanding colonoscopy simulator features helps programs select systems that prepare trainees for the specific challenges of colonic intubation and examination.
Our Simulation Training Solutions
At Suzhou Frank Medical , we provide comprehensive medical simulator options for endoscopy and interventional training programs. Our product line addresses training needs from basic skill development through advanced therapeutic technique acquisition.
Our gastrointestinal endoscopy simulator provides realistic upper and lower GI tract anatomy for navigation and diagnostic training. For programs teaching advanced resection techniques , our gastrointestinal ESD surgical simulator offers the tissue fidelity needed for submucosal dissection practice.
We also support training across related specialties. Our bronchoscopy simulators (Model A , Model B , Model C) address pulmonary training needs. Our ultrasound bronchoscopy simulator supports EBUS training for combined endoscopic and ultrasound procedures.
Additional specialty simulators include our urological endoscopy simulator for urologic procedures , hysteroscopy simulator for gynecologic applications , and laparoscopy simulator for surgical skill development.
Explore our complete range of endoscopic intervention training models to find simulators matching your program's specific training objectives. Our team can help identify solutions appropriate for your trainee population , curricular goals and available resources.
Conclusion
Medical simulation has transformed endoscopy and GI training from apprenticeship-based learning to structured , competency-verified education. The evidence supporting simulation is robust. The technologies are mature and continuously improving. The educational benefits for trainees and safety benefits for patients are well documented.
Programs not yet utilizing medical simulation should consider how to begin integration. Those with existing programs should evaluate whether current approaches maximize simulation's potential. All stakeholders in endoscopy education should recognize that simulation-based training represents not future aspiration but present standard of care.
© 2025. All rights reserved.
About Us
Introduction
Development
Cooperation
Service
Main Products
Medical Grade Monitor
No 15, Jinyang road KunshanSuzhou, Jiangsu, China
