📞Customer Service: +86 13248368268 📧servicecenter@suzhoufrank.com one year replacement and warranty!
Advanced Endoscopy: Meaning and Common Types
Advanced endoscopy goes beyond diagnosis into therapeutic territory. Covers ERCP , EUS , endoscopic resection and how physicians decide when it's needed.
ENDOSCOPY
Dr Qi Rui
1/9/20266 min read
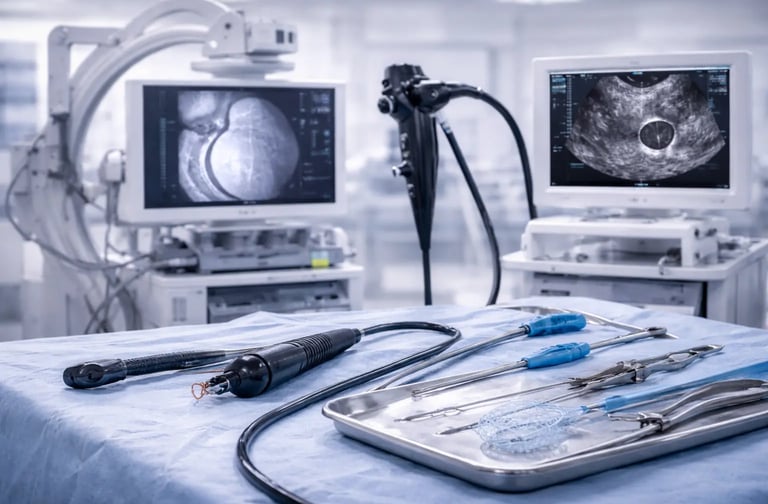
Standard endoscopy examines internal surfaces and takes biopsies. But what happens when a patient needs more than visualization and tissue sampling? When tumors require removal through the scope , when blocked bile ducts need opening , when early cancers can be excised without surgery?
This is where advanced endoscopy enters the picture. The term describes a set of complex endoscopic procedures that go beyond diagnostic examination into therapeutic territory. Understanding what advanced endoscopy means , which procedures it includes and how physicians decide when it's needed helps clarify this increasingly important area of gastroenterology.
What Makes Endoscopy "Advanced"?
The distinction between standard and advanced endoscopy isn't always formally defined , but the medical community generally recognizes certain characteristics that separate the two.
Standard endoscopy typically involves diagnostic examination , surveillance of known conditions and straightforward interventions like routine biopsies or simple polyp removal. These procedures form the bread and butter of gastroenterology practice. Most gastroenterologists perform them regularly after completing standard fellowship training. For foundational understanding of basic endoscopic procedures , reviewing what endoscopy involves provides essential context.
Advanced endoscopy involves procedures requiring additional specialized training beyond standard gastroenterology fellowship. These procedures typically carry higher complexity , greater technical demands and increased risk compared to routine endoscopy. They often serve therapeutic purposes that might otherwise require surgery. The American Society for Gastrointestinal Endoscopy recognizes advanced endoscopy as a distinct subspecialty requiring dedicated fellowship training of one to two additional years.
The "advanced" designation reflects several factors: technical difficulty requiring specialized skills , need for specialized equipment beyond standard endoscopes , higher procedural risk requiring expertise in complication management , and the ability to accomplish what previously required surgical intervention. Not every complex-sounding procedure qualifies as advanced endoscopy , and the boundaries shift as techniques that once seemed cutting-edge become routine.
Common Types of Advanced Endoscopy
Several procedure categories fall under the advanced endoscopy umbrella. Each serves distinct clinical purposes and requires specific expertise.
ERCP (Endoscopic Retrograde Cholangiopancreatography) represents one of the most established advanced endoscopy procedures. ERCP accesses the bile ducts and pancreatic duct through the duodenum , allowing diagnosis and treatment of biliary and pancreatic diseases. Physicians use ERCP to remove bile duct stones , place stents in blocked ducts , obtain tissue samples from suspicious strictures and manage complications of pancreatitis. The procedure requires specialized side-viewing endoscopes and fluoroscopic imaging to guide wire and catheter placement into the ductal systems.
ERCP exemplifies how advanced endoscopy replaces surgery. Patients with bile duct stones once required open surgical exploration. Now most undergo ERCP with sphincterotomy and stone extraction , avoiding surgical incisions entirely. The technical demands are substantial. Cannulating the appropriate duct , navigating complex anatomy and managing complications like bleeding or perforation require extensive training and ongoing volume to maintain competence.
Endoscopic Ultrasound (EUS) combines endoscopy with ultrasound imaging to visualize structures beyond the GI tract wall. Standard endoscopy sees only the mucosal surface. EUS sees through it , imaging layers of the gut wall , adjacent lymph nodes , pancreas , bile ducts and surrounding structures.
EUS serves both diagnostic and therapeutic purposes. Diagnostically , it stages cancers by assessing tumor depth and lymph node involvement. It characterizes submucosal lesions invisible to standard endoscopy. It evaluates pancreatic masses and cysts. Therapeutically , EUS guides fine-needle aspiration and biopsy of lesions unreachable by other means. Advanced EUS techniques now drain pancreatic pseudocysts , place biliary stents when ERCP fails and deliver targeted therapies directly into tumors.
Endoscopic Mucosal Resection (EMR) and Endoscopic Submucosal Dissection (ESD) remove early cancers and precancerous lesions without surgery. EMR lifts and snares lesions for removal , suitable for smaller abnormalities. ESD dissects larger lesions from the submucosal layer , enabling en bloc removal of sizeable early cancers.
These techniques revolutionized treatment of early GI cancers. Patients with early esophageal , gastric or colorectal cancers who would previously have required major surgery may now undergo endoscopic resection with organ preservation. The technical demands are significant , particularly for ESD , which requires meticulous dissection skills and substantial procedural time. Complication rates are higher than standard polypectomy , requiring expertise in managing bleeding and perforation.
Advanced biliary and pancreatic procedures extend beyond basic ERCP. Cholangioscopy passes a tiny scope through the ERCP scope into the bile duct itself , enabling direct visualization and targeted biopsies of strictures. Pancreatic interventions drain collections , disrupt stones and manage complex ductal anatomy. These procedures push technical boundaries and require the most experienced practitioners.
Bariatric and metabolic endoscopy represents an emerging advanced endoscopy frontier. Endoscopic sleeve gastroplasty , intragastric balloons and other techniques offer weight loss interventions without surgical incisions. While still evolving , these procedures are expanding advanced endoscopy beyond traditional diagnostic and cancer-focused applications.
When Doctors Recommend Advanced Endoscopy
Physicians consider advanced endoscopy when clinical situations exceed what standard endoscopy can accomplish. Several scenarios commonly prompt referral to advanced endoscopy specialists.
Biliary obstruction from stones or strictures often requires ERCP. When imaging shows dilated bile ducts , elevated liver enzymes suggest obstruction or jaundice develops , ERCP can diagnose the cause and often treat it in the same session. Patients with gallstone pancreatitis frequently undergo ERCP to clear retained bile duct stones.
Pancreatic disease evaluation often requires EUS. Pancreatic masses need characterization and tissue sampling. Cystic lesions require assessment to determine malignant potential. EUS provides imaging detail and biopsy access that CT and MRI cannot match.
Early GI cancers or large precancerous lesions may be candidates for endoscopic resection. When staging suggests superficial disease without lymph node involvement , EMR or ESD can potentially cure cancer while preserving the organ. This requires careful patient selection and expertise in determining which lesions are appropriate for endoscopic versus surgical management.
Submucosal tumors and lesions of uncertain significance often need EUS characterization. Standard endoscopy sees a bulge but cannot determine what lies beneath. EUS reveals the layer of origin , internal characteristics and features suggesting benign versus malignant nature.
Complex therapeutic needs that would otherwise require surgery increasingly fall to advanced endoscopy. Refractory strictures , enteral access for feeding , management of surgical complications and other challenging scenarios may have endoscopic solutions when performed by appropriately trained specialists.
The Training Pathway
Advanced endoscopy requires training beyond standard gastroenterology fellowship. After completing three years of GI fellowship , physicians pursuing advanced endoscopy undertake an additional one to two years of specialized training. This fourth-year fellowship focuses intensively on ERCP , EUS and other complex procedures.
Volume matters in advanced endoscopy. Competence requires performing hundreds of procedures under supervision before independent practice. Maintaining skills requires ongoing procedural volume. This concentration of experience explains why advanced procedures typically occur at larger medical centers with sufficient case volume to support specialized practitioners.
The training pathway ensures that physicians performing high-risk procedures have developed appropriate judgment about patient selection , technical skills for successful completion and expertise in managing complications when they occur.
Equipment and Infrastructure
Advanced endoscopy requires specialized equipment beyond standard endoscopes. ERCP uses side-viewing duodenoscopes designed for cannulating the papilla. EUS requires echoendoscopes integrating ultrasound transducers. Therapeutic procedures need specialized accessories for tissue resection , hemostasis and stent deployment.
Quality visualization remains fundamental. Advanced procedures benefit from high-resolution medical endoscope cameras that reveal subtle tissue details during complex interventions. Proper illumination from reliable LED light sources ensures optimal visibility in challenging anatomical locations. Specialized endoscope instruments enable the precise tissue manipulation that therapeutic procedures demand.
Facilities performing advanced endoscopy need fluoroscopy capabilities for ERCP , anesthesia support for lengthy procedures and infrastructure for managing complications including surgical backup when needed. This explains why advanced endoscopy concentrates in hospitals and large ambulatory centers rather than community endoscopy units.
Risks and Benefits
Advanced endoscopy carries higher risk than standard procedures. ERCP causes pancreatitis in a small but significant percentage of cases. Perforation rates exceed those of diagnostic endoscopy. Bleeding complications occur more frequently with therapeutic interventions. These risks require informed consent discussions that honestly convey what can go wrong.
The benefits often justify these risks. Avoiding major surgery means shorter recovery , less pain , lower overall complication rates and preservation of organs. For appropriate candidates , advanced endoscopy achieves outcomes comparable to surgery with substantially less invasiveness.
Patient selection determines the risk-benefit balance. Not every problem amenable to advanced endoscopy should be treated that way. Sometimes surgery remains the better choice. Experienced advanced endoscopists understand these nuances and recommend the approach most likely to benefit each individual patient.
The Expanding Frontier
Advanced endoscopy continues evolving. Techniques considered experimental years ago have become standard practice. New approaches currently in development will likely become tomorrow's established procedures.
Third-space endoscopy , including peroral endoscopic myotomy (POEM) for achalasia , exemplifies this evolution. Endoscopists now tunnel through tissue planes to reach treatment targets that would previously require surgical access. Endoscopic full-thickness resection removes lesions involving all gut wall layers. Combination procedures integrate multiple advanced techniques.
Training programs adapt to incorporate emerging procedures. Equipment manufacturers develop instruments enabling new capabilities. The definition of what constitutes "advanced" endoscopy will continue shifting as today's innovations become routine.
Conclusion
Advanced endoscopy represents the therapeutic frontier of endoscopic practice. Procedures like ERCP , EUS , EMR and ESD accomplish what once required surgery , offering patients less invasive alternatives for serious conditions. Understanding what advanced endoscopy means helps patients and referring physicians recognize when these specialized capabilities might benefit clinical care.
The complexity and risk of these procedures demand specialized training and appropriate infrastructure. When performed by experienced practitioners in well-equipped facilities , advanced endoscopy extends what's possible through the scope , turning diagnostic tools into therapeutic instruments.
© 2025. All rights reserved.
About Us
Introduction
Development
Cooperation
Service
Main Products
Medical Grade Monitor
No 15, Jinyang road KunshanSuzhou, Jiangsu, China
