📞Customer Service: +86 13248368268 📧servicecenter@suzhoufrank.com one year replacement and warranty!
Clinical Simulation in GI and Endoscopy
Clinical simulation bridges theory and real patient care in GI and endoscopy. Learn how case-based practice, team drills, and crisis training prepare practitioners for safe, effective procedures
MEDICAL TRAINING
Dr Qi Rui
1/22/20267 min read
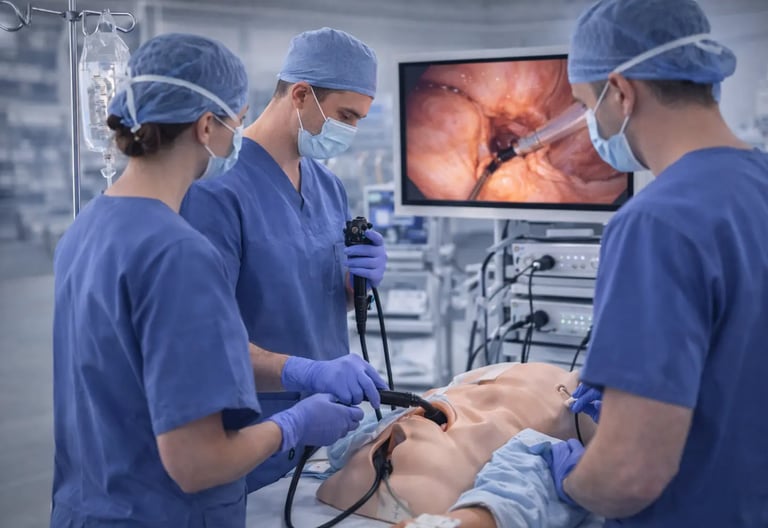
Modern medical training demands more than textbook knowledge. Practitioners need to develop clinical judgment , technical precision , and the ability to respond calmly when things go wrong. Clinical simulation provides the bridge between theoretical learning and real patient care. In gastroenterology and endoscopy , simulation has become essential for preparing trainees to handle everything from routine diagnostic procedures to life-threatening emergencies.
This guide explores how clinical simulation applies to GI and endoscopy training , covering case-based practice , team drills , crisis management , and the practical application of medical simulation across endoscopic specialties.
What Is Clinical Simulation?
Clinical simulation recreates healthcare situations for educational purposes. According to the Society for Simulation in Healthcare , simulation serves four main purposes in medicine: education , assessment , research , and health system integration to facilitate patient safety. The common thread is representing real clinical situations in controlled environments where learning can happen without risk to actual patients.
In practical terms , clinical simulation ranges from simple task trainers that replicate basic procedures to complex scenarios involving multiple team members , realistic patient responses , and time pressure. The level of complexity depends on the learning objectives. A trainee practicing basic scope handling needs different simulation resources than a team rehearsing their response to massive GI bleeding.
The key distinction between clinical simulation and isolated skills practice is context. Clinical simulation places technical skills within realistic patient care scenarios. Trainees must integrate procedural technique with clinical decision making , communication , and situational awareness. This integration prepares them for the multifaceted demands of actual practice.
Clinical Simulation in GI Endoscopy
Gastroenterology relies heavily on procedural skills. Upper endoscopy , colonoscopy , and more advanced interventions like ERCP and endoscopic ultrasound all require technical proficiency combined with interpretive ability. Clinical simulation addresses both dimensions.
Procedural simulation allows trainees to develop the manual dexterity and spatial awareness needed for scope manipulation. A GI Endoscopy Simulator provides anatomically accurate pathways where trainees can practice navigation , orientation , and basic maneuvers. They learn how the scope responds to control inputs , how to recognize landmarks , and how to maintain orientation within three-dimensional anatomy.
Beyond basic navigation , clinical simulation in GI incorporates diagnostic challenges. Trainees practice systematic examination techniques , learn to recognize pathology , and develop the pattern recognition that supports clinical decision making. Simulated cases can present a range of findings from normal anatomy to subtle lesions that require careful inspection to detect.
Therapeutic simulation takes training further by introducing interventional procedures. Biopsy , polypectomy , hemostasis , and more complex techniques like endoscopic submucosal dissection all benefit from simulation practice. The GI ESD Surgical Simulator allows trainees to develop the precise dissection skills required for advanced resection techniques before attempting them on patients.
Case-Based Practice
Effective clinical simulation organizes learning around realistic cases rather than isolated skills. A case-based approach presents trainees with patient scenarios that unfold over time , requiring them to gather information , make decisions , and perform appropriate interventions.
Consider a simulated upper endoscopy case. The scenario begins with a clinical history: a 65-year-old patient with iron deficiency anemia and weight loss. The trainee must perform the procedure with these clinical details in mind , maintaining appropriate suspicion for malignancy while conducting a thorough examination. If the simulation reveals a suspicious lesion , the trainee must decide on biopsy technique , specimen handling , and immediate next steps.
Case-based practice teaches clinical reasoning alongside procedural skill. Trainees learn to integrate findings from history , examination , and endoscopic visualization into coherent diagnostic assessments. They practice communicating their findings and explaining their reasoning. This integration mirrors how clinical medicine actually works , where procedures exist within broader patient care contexts.
Scenario design can incorporate increasing complexity as trainees advance. Early cases might present straightforward situations with clear endpoints. Advanced cases might include unexpected findings , complications that require management decisions , or time pressure that tests performance under stress.
Team Drills and Interprofessional Training
Endoscopy rarely involves a single practitioner working alone. Successful procedures require coordinated teamwork between endoscopists , nurses , technicians , and anesthesia providers. Clinical simulation provides opportunities to develop and maintain team function.
Team drills bring together all members of the endoscopy team to practice coordinated responses. A simulation might involve the entire team working through a case where a patient develops respiratory depression during sedation. Each team member has specific responsibilities. The endoscopist must recognize the problem and direct the response. Nurses must prepare medications and equipment. Everyone must communicate clearly and work together under pressure.
Research supports the value of team training. According to AHRQ's Patient Safety Network , teamwork training that incorporates simulation has been widely integrated into healthcare settings including endoscopy units. Multidisciplinary simulation-based teamwork training can yield improvement in participants' knowledge and skills while also improving actual patient outcomes.
In situ simulation takes team training into the actual clinical environment. Rather than practicing in a dedicated simulation center , teams rehearse in their own endoscopy suite using their own equipment. This approach identifies latent safety issues , tests workflows , and helps teams function better in the spaces where they actually work.
Team drills also support communication skill development. Trainees practice handoff communication , closed-loop communication during emergencies , and speaking up when they observe potential problems. These non-technical skills complement procedural training and contribute to safer care.
Crisis Management Training
Complications happen in endoscopy. Bleeding , perforation , aspiration , cardiac events , and other emergencies occur despite careful technique and patient selection. Clinical simulation prepares teams to manage these situations effectively.
Crisis simulation recreates emergency scenarios in controlled settings. A team might work through a case of massive upper GI bleeding where the patient is hemodynamically unstable. The endoscopist must achieve hemostasis while the team manages resuscitation. Everyone practices their roles under realistic time pressure.
These simulations accomplish several objectives. First , they ensure team members know their responsibilities during emergencies. Second , they identify gaps in equipment , protocols , or training. Third , they build confidence that translates to better performance when real emergencies occur. Fourth , they provide opportunities for deliberate practice of rare but critical interventions.
Evidence suggests simulation-based crisis training improves real-world outcomes. Studies have shown that targeted simulation training can reduce adverse events and improve adherence to best practices. When teams have rehearsed their emergency responses , they execute more smoothly when actual crises occur.
Crisis scenarios can address a range of potential complications. Respiratory emergencies , cardiac arrest , anaphylaxis , perforation management , and severe bleeding all represent important training topics. The specific scenarios selected should reflect the actual risks present in each clinical setting.
Clinical Simulation Across Endoscopy Specialties
While GI endoscopy provides many examples , clinical simulation principles apply across all endoscopic specialties. Each field has unique procedural requirements and clinical scenarios that simulation can address.
Pulmonary medicine relies on bronchoscopy for both diagnosis and therapy. Clinical simulation in bronchoscopy includes airway navigation , lesion identification , and sampling techniques. Bronchoscopy simulators such as the Bronchoscopy Simulator Type A , Type B , and Type C provide anatomically accurate airway models for navigation practice. For trainees learning endobronchial ultrasound , the Ultrasound Bronchoscopy Simulator combines imaging interpretation with procedural technique.
Urological endoscopy presents distinct challenges due to smaller caliber anatomy and delicate structures. Clinical simulation for cystoscopy and ureteroscopy teaches navigation through the urinary tract , stone management , and tissue sampling. The Urological Endoscopy Simulator supports these training needs. For prostate procedures , the Prostate Ultrasound Simulator allows practice combining imaging guidance with procedural technique.
Gynecological endoscopy has its own requirements. Hysteroscopy training addresses intrauterine navigation , pathology recognition , and therapeutic interventions. The Hysteroscopy Simulator provides realistic practice for these procedures.
Laparoscopic surgery shares many skills with endoscopy. The Laparoscopy Simulator supports training in camera navigation , instrument handling , and basic surgical techniques. These foundational skills transfer to more advanced minimally invasive procedures.
Spine surgery has embraced endoscopic approaches for certain conditions. The Intervertebral Foramen Endoscope Simulator supports training in these specialized techniques.
Designing Effective Clinical Simulation Programs
Clinical simulation requires thoughtful design to achieve educational objectives. Research reviewed in a PMC article on simulation-based training identifies several features associated with effective simulation programs.
Clear learning objectives guide scenario development. Rather than vague goals like "practice endoscopy" , effective programs specify exactly what skills , knowledge , and behaviors trainees should develop. Objectives might include technical metrics , decision making criteria , communication standards , or team function elements.
Realistic scenarios engage learners and promote skill transfer. Clinical fidelity means creating situations that feel like actual patient care , with appropriate complexity , time pressure , and uncertainty. Physical fidelity refers to how closely equipment and environment match real practice settings. Both types of realism contribute to effective learning.
Structured debriefing follows simulation activities. During debriefing , facilitators guide learners through reflection on what happened , why it happened , and how performance might improve. Research consistently shows that debriefing significantly enhances learning from simulation experiences. Without proper debriefing , much of simulation's educational value is lost.
Assessment methods document trainee progress. Clinical simulation supports both formative assessment for learning improvement and summative assessment for competency determination. Validated tools help ensure consistent and meaningful evaluation.
Integration with clinical training connects simulation to patient care. Simulation works best when it complements rather than replaces clinical experience. Trainees benefit from cycling between simulated practice and supervised patient care , applying lessons from each setting to the other.
Clinical Simulation Products from Suzhou Frank Medical
At Suzhou Frank Medical , we manufacture clinical simulation equipment designed to support comprehensive training programs across endoscopic specialties. Our product line includes anatomically accurate simulators for gastrointestinal , pulmonary , urological , gynecological , and surgical training applications.
We understand that effective clinical simulation requires realistic models that allow trainees to develop both technical skills and clinical judgment. Our simulators are built to withstand intensive training use while providing the fidelity needed for meaningful educational experiences.
Programs establishing or expanding clinical simulation capabilities can explore our complete endoscopic intervention training model catalog. For questions about specific products or to discuss how our simulators might support your training objectives , please contact us directly.
The Future of Clinical Simulation in Endoscopy
Clinical simulation continues to evolve. Technology advances enable increasingly realistic scenarios. Assessment methods become more sophisticated. Integration with competency-based training frameworks grows tighter.
For GI and endoscopy training , simulation has moved from optional supplement to expected component. Programs that invest in quality simulation experiences prepare trainees more effectively , reduce risk during the learning curve , and ultimately deliver better patient care.
The evidence is clear: clinical simulation improves performance , reduces errors , and enhances patient safety. For endoscopy training programs committed to excellence , simulation is not a luxury. It's a necessity that shapes how the next generation of practitioners develops the skills they need to provide safe , effective care.
© 2025. All rights reserved.
About Us
Introduction
Development
Cooperation
Service
Main Products
Medical Grade Monitor
No 15, Jinyang road KunshanSuzhou, Jiangsu, China
