📞Customer Service: +86 13248368268 📧servicecenter@suzhoufrank.com one year replacement and warranty!
Fellowship Training in Advanced Endoscopy: Simulation Strategies
Fellowship training in advanced endoscopy integrates simulation for ERCP, ESD, and complex resection techniques. Learn how programs build procedural competency.
MEDICAL TRAINING
Dr Qi Rui
3/4/20265 min read
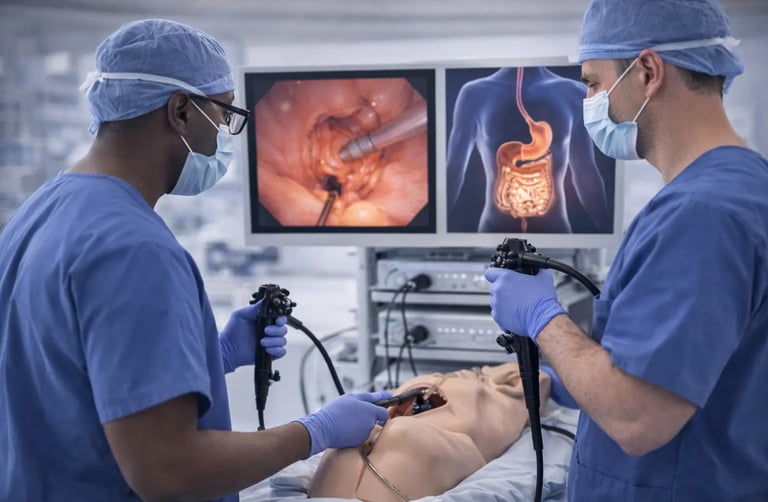
Advanced endoscopy fellowships represent the pinnacle of procedural gastroenterology education. These programs prepare physicians for technically demanding interventions including endoscopic retrograde cholangiopancreatography (ERCP), endoscopic submucosal dissection (ESD), endoscopic mucosal resection (EMR), and third-space procedures like peroral endoscopic myotomy (POEM). The complexity of these procedures, combined with their inherent risks, makes fellowship training particularly challenging. Increasingly, simulation has emerged as an essential component of advanced endoscopy curricula, offering fellows opportunities to develop foundational skills before performing complex interventions on patients.
The transition from general gastroenterology fellowship to advanced endoscopy fellowship marks a significant shift in procedural expectations. While general fellows may complete their training with competency in diagnostic endoscopy and colonoscopy, advanced procedures require entirely different skill sets. ERCP demands proficiency with side-viewing duodenoscopes and wire-guided cannulation techniques. ESD requires mastery of submucosal dissection planes and electrosurgical knife handling. These techniques cannot be learned quickly, and the learning curve carries real consequences for patient safety.
The Simulation Imperative in Advanced Training
Traditional apprenticeship models, while still central to procedural education, present limitations when applied to advanced endoscopy. The complexity of procedures like ERCP means that even experienced endoscopists require substantial exposure before achieving competency. Research published in the Journal of Interventional Gastroenterology indicates that trainees may need between 180 and 400 ERCP procedures to achieve an 80% success rate with selective cannulation. This volume requirement creates significant challenges for fellowship programs, particularly those with limited case exposure.
Simulation addresses this gap by providing repetitive practice opportunities without patient risk. Fellows can work through the mechanics of scope handling, accessory manipulation, and tissue interaction before entering the procedure suite. The goal is not to replace clinical training but to compress the early learning curve, allowing fellows to approach their first supervised cases with greater confidence and technical familiarity.
For fellowship programs building simulation curricula, the GI Endoscopy Simulator provides a foundation for developing basic scope handling and navigation skills that translate directly to more complex procedures.
Simulation Approaches for ERCP Training
ERCP represents one of the most challenging procedures in gastroenterology, combining endoscopic skill with fluoroscopic guidance and delicate wire manipulation. The procedure carries meaningful complication rates even among experienced operators, including post-ERCP pancreatitis, bleeding, and perforation. These risks make simulation particularly valuable during the fellowship training period.
Several simulation modalities have been applied to ERCP training. Computer-based simulators offer the advantage of standardized anatomy and reproducible scenarios, allowing fellows to practice cannulation techniques and wire manipulation in a controlled environment. However, these systems often use specialized probes rather than actual endoscopic accessories, limiting their fidelity to clinical practice.
Ex vivo porcine models provide more realistic tissue interaction, allowing fellows to work with actual duodenoscopes and accessories. The Erlangen Endo-Trainer and similar platforms use preserved animal tissue to simulate papillary anatomy, bile duct structure, and tissue response to instrumentation. Modifications such as the Neo-Papilla technique, which incorporates chicken heart tissue to create a more anatomically accurate papilla, have improved the realism of sphincterotomy practice.
Mechanical simulators offer a middle ground, providing the durability needed for repeated practice sessions while accommodating real endoscopic equipment. These systems can incorporate simulated fluoroscopy, allowing fellows to practice the integration of radiographic guidance with endoscopic technique. The ability to perform multiple cannulation attempts, sphincterotomies, and stent placements in a single session accelerates skill acquisition.
Simulation for ESD and Tissue Resection Techniques
Endoscopic submucosal dissection presents unique training challenges. Unlike ERCP, where the procedural steps follow a relatively predictable sequence, ESD requires continuous judgment about dissection planes, bleeding management, and perforation avoidance. The procedure is technically demanding and time-consuming, with learning curves that extend well beyond initial fellowship training.
Animal models have become standard for ESD training, particularly for programs in regions where early gastric cancer—the primary indication for ESD in Asia—is less common. As described in research from Clinical Endoscopy, both ex vivo and in vivo porcine models provide valuable training opportunities. Ex vivo models allow fellows to focus on basic knife handling and dissection technique without the added complexity of bleeding and peristalsis. In vivo models add physiological realism but require animal facility access and veterinary support.
The progression typically moves from ex vivo practice to in vivo training before supervised human cases. This graduated approach allows fellows to develop muscle memory for submucosal injection, circumferential incision, and controlled dissection before facing the additional variables present in clinical procedures. The GI ESD Surgical Simulator supports this progression by providing a platform for practicing the fundamental techniques of submucosal dissection.
Expanding Fellowship Training Beyond Gastroenterology
Advanced endoscopy fellowships increasingly incorporate exposure to procedures beyond the gastrointestinal tract. Interventional pulmonology techniques, including endobronchial ultrasound (EBUS) and navigational bronchoscopy, share technical elements with gastrointestinal endoscopy. Some fellowship programs offer cross-training opportunities that broaden procedural competency.
Simulation platforms designed for bronchoscopy allow fellows to practice airway navigation, biopsy technique, and ultrasound-guided sampling. The Ultrasound Bronchoscopy Simulator provides training in EBUS-guided procedures, while conventional bronchoscopy trainers like the Bronchoscopy Simulator Type A and Type B offer foundational airway endoscopy experience.
Similarly, simulation for urological and gynecological endoscopy expands the procedural toolkit available to interventionally oriented physicians. The Hysteroscopy Simulator and Urological Endoscopy Simulator provide training opportunities that complement gastrointestinal expertise, particularly for fellows interested in broader interventional careers.
Integrating Simulation into Fellowship Curricula
Effective simulation programs require more than equipment acquisition. Fellowship directors must consider how simulation sessions fit within overall training schedules, who will provide supervision and feedback, and how simulated performance connects to clinical competency assessment.
Structured simulation curricula typically begin with orientation sessions that familiarize fellows with equipment and basic techniques. Progressive complexity follows, with simulation scenarios advancing alongside clinical case exposure. Regular practice sessions, ideally weekly or bi-weekly during the early fellowship period, reinforce skills and build procedural automaticity.
Debriefing represents a critical but often underemphasized component of simulation training. Simply performing procedures on a simulator provides limited benefit without structured feedback. Expert observation, video review, and performance metrics help fellows identify areas for improvement and track their progress over time.
Simulation Equipment from Suzhou Frank Medical
At Suzhou Frank Medical, we manufacture simulation equipment designed to support advanced endoscopy fellowship programs. Our simulators provide the anatomical accuracy and durability that intensive fellowship training demands. When programs need equipment that can handle repeated use by multiple fellows while delivering consistent tactile feedback and realistic tissue interaction, build quality matters.
Explore our complete endoscopic intervention training model catalog to see the full range of training options available. For questions about specific applications or to discuss how our simulators might fit your fellowship program's curriculum, contact us directly.
Key Considerations for Fellowship Programs
When developing simulation-integrated curricula, fellowship programs should evaluate several factors. First, simulation should complement rather than replace clinical training—the goal is accelerating early skill acquisition, not substituting for supervised patient care. Second, equipment selection should prioritize compatibility with actual endoscopic instruments, as the tactile learning that comes from handling real accessories transfers more directly to clinical practice. Third, faculty engagement matters significantly; simulation sessions led by experienced interventional endoscopists provide modeling and feedback that self-directed practice cannot replicate. Fourth, assessment integration helps validate simulation effectiveness—tracking how simulated performance correlates with clinical outcomes guides curriculum refinement. Finally, programs should budget for ongoing consumables and maintenance, as simulation platforms require regular upkeep to maintain training quality.
The incorporation of simulation into advanced endoscopy fellowship training represents an investment in both trainee development and patient safety. As procedural expectations continue to evolve, simulation will likely assume an increasingly central role in preparing the next generation of interventional endoscopists.
© 2025. All rights reserved.
About Us
Introduction
Development
Cooperation
Service
Main Products
Medical Grade Monitor
No 15, Jinyang road KunshanSuzhou, Jiangsu, China
