📞Customer Service: +86 13248368268 📧servicecenter@suzhoufrank.com one year replacement and warranty!
GI Simulators: Options for Gastrointestinal Endoscopy Training
GI simulator options for endoscopy training include mechanical, virtual reality, and tissue models. Compare features supporting upper and lower GI skill development.
MEDICAL TRAINING
Dr Qi Rui
3/6/20265 min read
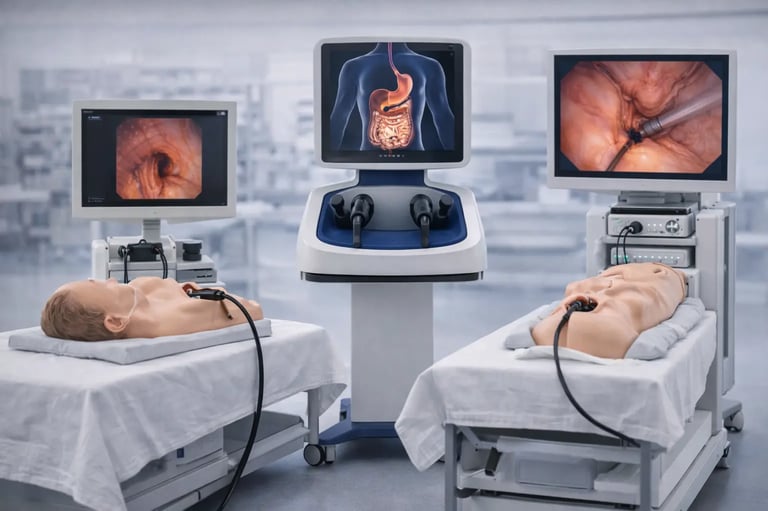
Gastrointestinal endoscopy requires technical precision, visual-spatial awareness, and procedural judgment that develops only through extensive hands-on experience. Traditional apprenticeship-based training models, while effective, present limitations around patient safety, procedure duration, and standardization of competency assessment. The emergence of the GI simulator as a training modality addresses these challenges by providing risk-free environments where trainees can develop foundational skills before performing procedures on patients.
This article examines the categories of GI simulators available for endoscopy training, their distinguishing features, and practical considerations for training program implementation.
Understanding the Role of Simulation in Endoscopy Training
The rationale for incorporating GI simulators into training programs extends beyond patient safety considerations. Research published in the journal Cancers notes that simulation platforms can standardize various educational metrics and provide objective assessment of technical skills, addressing a significant limitation of conventional training approaches where competency evaluation often lacks consistency (Finocchiaro et al., 2021).
Simulation-based training allows trainees to practice specific techniques repeatedly without extending clinical procedure times or affecting patient comfort. The simulator-based approach has gained particular relevance following pandemic-related disruptions to endoscopy training, which significantly reduced procedure volumes at teaching institutions and accelerated interest in alternative training methodologies.
For programs seeking foundational information on simulation principles, our complete guide to medical simulation in endoscopy and GI training provides comprehensive coverage of educational frameworks and implementation considerations.
Categories of GI Simulator Platforms
Training simulators for gastrointestinal endoscopy fall into three primary categories, each with distinct advantages for different training objectives.
Mechanical Simulators
Mechanical GI simulators use physical phantoms constructed from materials like silicone to replicate anatomical structures. The cavity within these phantoms allows endoscope insertion and practice of navigation maneuvers. According to a review in Clinical Endoscopy, mechanical simulators offer advantages including lower cost compared to computerized alternatives, effectiveness for initial-phase training, and superior haptic realism compared to virtual reality systems (Kim et al., 2023).
The tactile feedback from mechanical simulators allows trainees to develop an intuitive understanding of tissue resistance and instrument response. Physical models replicate the three-dimensional structure of the gastrointestinal tract, supporting practice of scope insertion techniques, retroflexion maneuvers, and basic navigation skills.
Models like the Gastrointestinal Endoscopy Simulator exemplify this category, providing anatomically accurate representations of the upper GI tract from esophagus through duodenum. These systems support training in both diagnostic observation and basic therapeutic techniques using standard clinical endoscopes.
For programs emphasizing advanced therapeutic procedures, dedicated platforms address specific technique requirements. The Gastrointestinal ESD Surgical Simulator focuses on submucosal dissection techniques, allowing practice of marking, injection, incision, and dissection sequences in a controlled environment before attempting these technically demanding procedures on patients.
Virtual Reality Simulators
Virtual reality GI simulators combine hardware interfaces with software that generates computer-rendered images of the gastrointestinal tract. These systems track endoscope movements and translate them into visual feedback on a monitor, creating an interactive training environment.
A Cochrane systematic review examining VR simulation training found that trainees who received VR training demonstrated higher rates of independent procedure completion compared to those receiving no intervention, with moderate-quality evidence supporting the use of simulation as a supplement to conventional training (Khan et al., 2018).
Virtual reality platforms typically offer multiple procedure modules within a single system, including upper and lower GI endoscopy scenarios. Some advanced systems incorporate patient vital monitoring, sedation management simulations, and immediate performance metrics that support competency assessment. The ability to present identical scenarios to multiple trainees also facilitates standardized evaluation across training cohorts.
Ex Vivo and In Vivo Animal Models
Animal tissue models provide the highest degree of tactile realism and allow practice with actual electrosurgical equipment. Ex vivo models use explanted organs mounted in supporting frameworks, while in vivo training involves procedures on anesthetized animals.
These approaches are typically reserved for advanced therapeutic technique training, including hemostasis, polypectomy, and endoscopic submucosal dissection, where the properties of living or recently vital tissue most closely approximate human procedural conditions. Cost, logistical complexity, and ethical considerations limit their application to specialized training contexts.
Selecting Simulators for Different Training Objectives
The choice among GI simulator types depends on the specific skills being developed and the stage of trainee progression.
For novice endoscopists beginning their training, mechanical simulators provide an appropriate starting point for developing basic scope manipulation skills. The direct physical feedback helps establish fundamental motor patterns for instrument control, torque application, and tip deflection before trainees face the cognitive load of performing on actual patients.
Virtual reality platforms become increasingly valuable as trainees progress beyond basic manipulation toward integrated procedural performance. The ability to simulate complete procedures with varying pathology presentations supports development of diagnostic recognition and clinical decision-making alongside technical skills.
Programs developing therapeutic endoscopy curricula may benefit from dedicated training systems addressing specific procedures. For institutions training fellows in ESD techniques, simulators designed specifically for submucosal dissection practice allow repeated skill development before clinical application of these techniques.
Cross-Specialty Training Considerations
While gastrointestinal endoscopy represents the primary application, simulation training principles extend across endoscopic specialties. Programs training providers in multiple endoscopic disciplines may find value in platforms addressing bronchoscopy, urological endoscopy, and gynecological procedures.
Bronchoscopy simulation supports training in airway navigation and endobronchial ultrasound techniques. Systems like the Ultrasound Bronchoscopy Simulator address the combined imaging and biopsy skills required for lymph node sampling procedures. Basic bronchoscopy trainers including Bronchoscopy Simulator Type A and Bronchoscopy Simulator Type B support development of airway navigation and visualization techniques.
Urological endoscopy training benefits from simulators replicating cystoscopy and ureteroscopy procedures. The Urological Endoscopy Simulator provides structured training in lower urinary tract navigation and intervention techniques.
Similarly, gynecological training programs can incorporate the Hysteroscopy Simulator for uterine cavity visualization and procedure training.
Implementation Considerations
Integrating GI simulators into training programs requires attention to curriculum design, scheduling logistics, and assessment protocols. Effective simulation training typically follows structured curricula that progress from basic skills through increasingly complex procedural scenarios.
Assessment of simulator-based performance should employ validated evaluation tools where available. Direct observation of procedural skills using standardized rating scales allows documentation of trainee progression and identification of areas requiring additional practice.
Maintenance and durability considerations affect long-term program costs. Mechanical simulators experience wear from repeated use, and the anatomical accuracy of physical models depends on material quality and construction techniques. Programs with high training volumes should evaluate replacement component availability and anticipated service requirements when selecting equipment.
Suzhou Frank Medical: Training Equipment Solutions
At Suzhou Frank Medical, we specialize in endoscopic imaging systems and provide simulation training equipment designed to support medical education programs. Our equipment is manufactured for durability under intensive daily use, with attention to anatomical accuracy that supports effective skill development.
Our range of training simulators spans gastrointestinal, bronchoscopy, urological, and gynecological applications, allowing institutions to address multiple training requirements from a single supplier. For a complete overview of available training models, visit our endoscopic intervention training model catalog.
Programs interested in discussing specific training requirements or requesting product information can contact us directly for consultation and quotation.
Moving Forward with Simulation-Based Training
The evidence supporting GI simulator integration into endoscopy training continues to accumulate, though research also emphasizes that simulation supplements rather than replaces supervised clinical experience. Effective training programs combine simulator-based skill development with structured clinical mentorship, using simulation to accelerate early learning curves and reduce patient exposure during novice skill acquisition phases.
As simulation technology continues advancing, training programs should remain attentive to emerging evidence regarding optimal curriculum design, training duration, and integration with clinical practice. The goal remains consistent: developing competent endoscopists who can perform procedures safely and effectively while minimizing learning-curve impacts on patient outcomes.
© 2025. All rights reserved.
About Us
Introduction
Development
Cooperation
Service
Main Products
Medical Grade Monitor
No 15, Jinyang road KunshanSuzhou, Jiangsu, China
