📞Customer Service: +86 13248368268 📧servicecenter@suzhoufrank.com one year replacement and warranty!
Medical Imaging Analysis: From Image to Clinical Insight
Medical imaging analysis explained: from image acquisition to clinical action. Learn how images are reviewed , documented and integrated with clinical judgment.
MEDICAL IMAGING
Dr Qi Rui
1/2/20266 min read
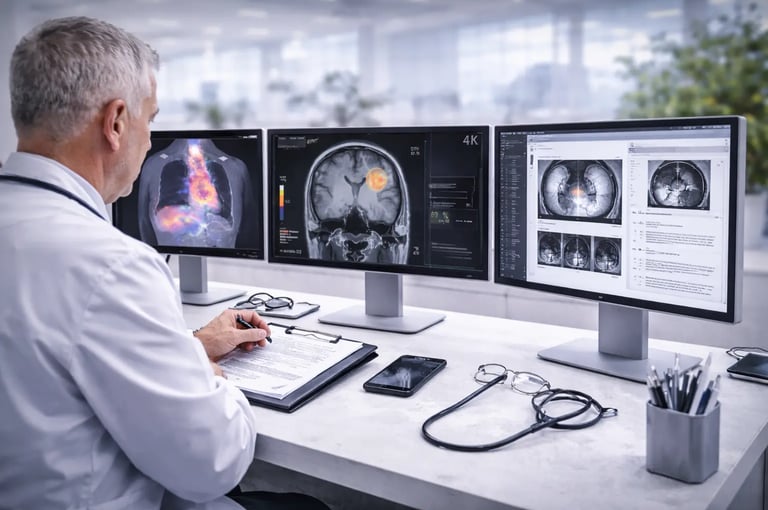
Medical images capture what's happening inside the body. But raw images alone don't guide treatment decisions. The process of examining , interpreting and extracting meaningful information from those images , medical imaging analysis , is what transforms visual data into clinical insight that shapes patient care.
This analysis happens every time a radiologist reviews a CT scan , every time a cardiologist interprets an echocardiogram , every time a pathologist examines a digital slide. Understanding how medical imaging analysis works helps clinicians appreciate both its power and its limitations. And as analysis tools become more sophisticated , knowing how they support (rather than replace) clinical judgment becomes increasingly important.
What Is Medical Imaging Analysis?
Medical imaging analysis encompasses all the processes involved in examining medical images to extract clinically useful information. This includes visual inspection by trained professionals , quantitative measurements , pattern recognition , comparison with prior studies and integration of imaging findings with other clinical data.
The National Institute of Biomedical Imaging and Bioengineering describes medical imaging as technologies that allow clinicians to see inside the body for diagnosis , treatment guidance and monitoring. Medical imaging analysis is the essential next step: making sense of what those technologies reveal.
Analysis varies by imaging modality and clinical application. A chest X-ray might receive rapid visual review for obvious abnormalities. A complex MRI study might require detailed measurements , multiplanar review and correlation with multiple prior examinations. The depth and approach of analysis matches the clinical question being answered.
What remains constant across all medical imaging analysis is the goal: convert visual information into actionable clinical insight.
The Pathway From Image to Insight
Medical imaging analysis follows a general workflow , though specifics vary by modality , institution and clinical context.
Image Acquisition and Quality Assessment
Analysis begins with quality evaluation. Are the images technically adequate? Is positioning appropriate? Are there artifacts that might obscure findings or mimic pathology? Poor quality images may require repeat acquisition before meaningful analysis can proceed.
Quality assessment requires understanding both the imaging technology and the clinical application. What constitutes acceptable quality for screening differs from what's needed for surgical planning. Medical imaging analysis expertise includes knowing when images are good enough and when they're not.
Systematic Review
Trained professionals review images systematically to avoid missing findings. Radiologists develop search patterns appropriate to each study type. A chest CT review might progress from lung windows to mediastinal windows to bone windows , examining each anatomic region methodically.
Systematic approaches reduce the chance that attention to one finding causes others to be overlooked. Medical imaging analysis training emphasizes these systematic methods because human attention naturally gravitates toward obvious abnormalities while potentially missing subtle but important findings elsewhere.
Finding Identification
The core of medical imaging analysis involves identifying abnormal findings. This requires pattern recognition developed through extensive training and experience. Abnormalities must be distinguished from normal variants , artifacts and incidental findings of no clinical significance.
Finding identification draws on knowledge of anatomy , pathology , disease manifestations and technical factors. A shadow on a lung image might represent tumor , infection , inflammation , atelectasis or artifact. Medical imaging analysis determines which explanation best fits the visual pattern and clinical context.
Characterization and Measurement
Identified findings require characterization. What are the specific features? Size , shape , density , enhancement pattern , location and relationship to adjacent structures all contribute to characterization.
Quantitative measurements provide objective data. Tumor dimensions , ventricular volumes , vessel diameters and countless other measurements support diagnosis , staging and monitoring. Medical imaging analysis increasingly incorporates standardized measurement protocols that ensure consistency across interpreters and institutions.
Comparison With Prior Studies
Most medical imaging analysis includes comparison with previous imaging when available. Has a nodule grown? Has inflammation resolved? Is treatment producing response?
Comparison provides temporal context that single examinations cannot. Changes over time often matter more than absolute findings at one moment. Effective comparison requires access to prior images and understanding of what changes are clinically significant.
Integration With Clinical Information
Images don't exist in isolation. Medical imaging analysis integrates visual findings with clinical history , laboratory results , physical examination findings and other diagnostic information. The same imaging finding may have different significance depending on clinical context.
A radiologist interpreting a chest CT approaches the study differently when clinical information indicates suspected pulmonary embolism versus lung cancer screening versus trauma evaluation. Clinical context shapes what the analysis seeks to find and how findings are interpreted.
Reporting and Communication
Analysis conclusions must be communicated effectively. Structured reports convey findings , impressions and recommendations in standardized formats that referring clinicians can quickly understand and act upon.
The European Society of Radiology has developed structured reporting guidelines that improve communication between imaging specialists and clinical teams. Clear reporting ensures the insight generated through medical imaging analysis actually reaches and influences patient care decisions.
Types of Medical Imaging Analysis
Different clinical applications require different analytical approaches.
Diagnostic Analysis
The most common form of medical imaging analysis aims to identify or exclude specific diagnoses. Is there evidence of appendicitis? Does this mammogram show malignancy? What's causing this patient's symptoms?
Diagnostic analysis answers clinical questions. The analysis approach and depth match the question being asked. Some questions require exhaustive review. Others can be answered with targeted focused evaluation.
Quantitative Analysis
Many clinical applications require precise measurements. Cardiac imaging measures ejection fraction and chamber volumes. Oncology imaging measures tumor dimensions for staging and response assessment. Vascular imaging quantifies stenosis severity.
Quantitative medical imaging analysis demands consistency. Measurement techniques must be standardized so values are comparable across time and between institutions. Automated measurement tools can improve consistency but require validation against clinical standards.
Functional Analysis
Some imaging modalities reveal function rather than just structure. Functional MRI shows brain activity patterns. Nuclear medicine studies demonstrate metabolic activity. Doppler ultrasound displays blood flow.
Functional medical imaging analysis interprets these dynamic processes. Understanding normal function is prerequisite to identifying dysfunction. This analysis type requires knowledge extending beyond anatomy into physiology.
Surveillance Analysis
Patients with known conditions often undergo serial imaging to monitor stability or detect progression. Cancer surveillance , aneurysm monitoring and transplant follow-up all involve repeated medical imaging analysis comparing current studies to prior baselines.
Surveillance analysis focuses specifically on change detection. Subtle interval changes that might be insignificant on initial presentation become highly relevant when following known disease.
Technology Supporting Medical Imaging Analysis
Modern medical imaging analysis increasingly incorporates technological tools that enhance human capabilities.
Display Technology
What analysts see depends on how images are displayed. High-resolution monitors , calibrated for medical use , reveal details that consumer displays might obscure. Understanding how advanced medical imaging technology affects visualization helps facilities make infrastructure decisions that support accurate analysis.
Display quality directly impacts diagnostic accuracy. A radiologist reviewing studies on a properly calibrated medical-grade monitor sees images as the imaging system intended them to appear. Inadequate displays can hide subtle findings or create misleading appearances.
Picture Archiving and Communication Systems
PACS infrastructure stores , distributes and displays medical images. These systems enable the comparison with prior studies that medical imaging analysis requires. They provide the workflow tools that support systematic review and efficient reporting.
PACS capabilities continue expanding. Integration with electronic health records , AI analysis tools and advanced visualization applications extends what medical imaging analysis can accomplish.
Advanced Visualization
3D reconstruction , multiplanar reformatting , volume rendering and other visualization techniques reveal information that standard 2D review might miss. Complex anatomy becomes comprehensible when viewed from multiple angles or rendered three-dimensionally.
The American Institute of Ultrasound in Medicine provides guidelines on image display and documentation that address visualization requirements for accurate analysis. Their standards recognize that how images are presented affects how accurately they're analyzed.
Computer-Aided Detection and Analysis
Algorithms can identify potential findings , perform measurements and flag studies that may require urgent attention. These tools support medical imaging analysis without replacing human interpretation.
Computer-aided systems excel at tasks requiring consistency: measuring the same structure the same way every time , scanning entire images for specific patterns , comparing current findings to prior studies quantitatively. They struggle with tasks requiring clinical judgment , contextual understanding and integration of information from multiple sources.
The most effective implementations position AI as a tool that augments human analysis rather than a replacement for clinical expertise.
Limitations and the Role of Clinical Judgment
Medical imaging analysis has inherent limitations that clinical judgment must navigate.
Uncertainty Is Unavoidable
Not every finding permits definitive interpretation. Indeterminate nodules , nonspecific enhancement patterns and ambiguous appearances are common. Medical imaging analysis often generates differential diagnoses rather than single answers.
Recognizing uncertainty and communicating it appropriately is part of expert analysis. Overconfident interpretation that ignores uncertainty can mislead clinical decision-making more than honest acknowledgment of diagnostic limitations.
Images Show Anatomy , Not Diagnosis
Imaging reveals visual patterns. Interpreting what those patterns mean diagnostically requires inference based on probability , clinical context and pattern recognition. The same imaging appearance can result from different pathological processes.
Medical imaging analysis provides evidence that supports or refutes diagnostic possibilities. It rarely provides pathological proof. Tissue diagnosis , clinical response to treatment and other confirmatory information often remain necessary.
Technology Doesn't Replace Expertise
Advanced analysis tools enhance what skilled professionals can accomplish. They don't substitute for the training , experience and clinical integration that medical imaging analysis requires.
Facilities investing in analysis technology should simultaneously invest in professional development. Tools are only as valuable as the expertise applying them.
The Future of Medical Imaging Analysis
Medical imaging analysis continues evolving. AI capabilities are expanding. Integration between imaging and other clinical data is deepening. Quantitative analysis is becoming more standardized and automated.
These advances promise more consistent , efficient and comprehensive analysis. But the fundamental process remains: transforming visual information into clinical insight through systematic expert review.
Facilities can prepare for advancing capabilities by investing in quality infrastructure , including display technology like 3D visualization systems that reveal depth information traditional displays cannot convey. Building strong foundational capabilities positions organizations to adopt emerging analysis tools effectively.
Conclusion
Medical imaging analysis is the bridge between image acquisition and clinical action. Through systematic review , pattern recognition , quantitative measurement and clinical integration , analysis transforms visual data into insight that guides patient care.
Understanding this process , including both its capabilities and limitations , helps clinicians use imaging effectively. As analysis tools become more sophisticated , maintaining focus on clinical judgment as the essential final step ensures technology serves rather than supplants expert care.
© 2025. All rights reserved.
About Us
Introduction
Development
Cooperation
Service
Main Products
Medical Grade Monitor
No 15, Jinyang road KunshanSuzhou, Jiangsu, China
