📞Customer Service: +86 13248368268 📧servicecenter@suzhoufrank.com one year replacement and warranty!
Procedure Training with Simulators: Stepwise Skill Building
Explains how procedure training is broken into steps and repeated on simulators, from basic scope insertion to complex therapeutic maneuvers, with examples from GI endoscopy.
MEDICAL TRAINING
Dr Qi Rui
1/21/20266 min read
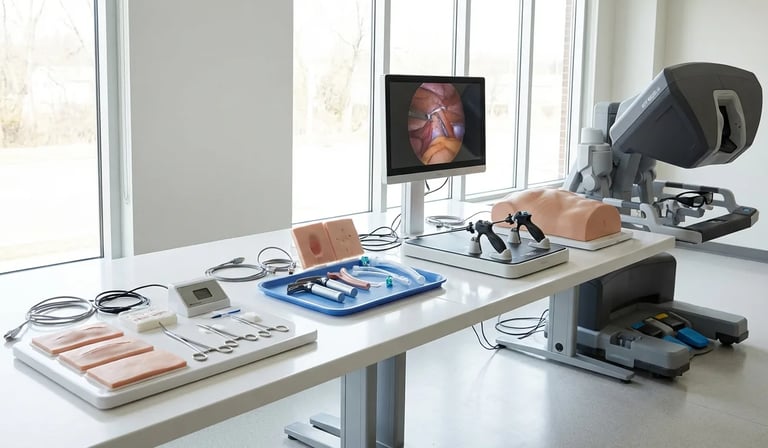
Medical procedures require a specific sequence of movements , decisions , and adjustments that must become second nature before they're performed on real patients. This doesn't happen overnight. It doesn't happen by watching videos or reading textbooks. And it certainly doesn't happen by jumping straight into complex clinical situations. Effective procedure training breaks down sophisticated techniques into component parts , builds skills progressively , and uses simulators to provide the repetitive practice that transforms awkward beginners into confident practitioners.
This guide explains how medical simulation programs structure procedure training for maximum learning impact.
Why Stepwise Training Matters
Complex procedures involve dozens of micro-skills working together. Consider a standard upper endoscopy. The trainee must hold the scope correctly , operate the control wheels smoothly , coordinate hand movements with visual feedback , navigate through anatomical landmarks , insufflate appropriately , recognize normal versus abnormal findings , capture images at the right moments , and manage any complications that arise. Trying to learn all of this simultaneously overwhelms cognitive capacity.
The traditional apprenticeship model threw trainees into this complexity from day one. They watched experienced practitioners , then attempted the procedure themselves while a supervisor stood ready to intervene. This approach worked , eventually. But it placed unnecessary stress on trainees , extended learning curves , and created variable outcomes depending on case mix and supervision quality.
Stepwise training recognizes that procedures can be decomposed into discrete skills. Each component can be isolated , practiced repeatedly , and mastered before moving to the next level of complexity. According to research on deliberate practice in medical simulation , this focused approach with clear objectives and immediate feedback produces better outcomes than unstructured repetition.
The Building Blocks of Procedure Training
Effective procedure training progresses through identifiable stages. The exact sequence varies by procedure type , but the general framework applies broadly.
The foundation layer covers basic device handling. For endoscopic procedures , this means learning to hold the endoscope , understanding which controls do what , and developing coordination between hand movements and scope tip deflection. Trainees practice these fundamentals without worrying about anatomy or pathology recognition. The goal is making basic manipulation feel natural.
A GI Endoscopy Simulator provides an ideal environment for this early practice. Trainees can repeat basic maneuvers hundreds of times without time pressure or patient concerns. They develop the muscle memory that will later support more complex tasks.
The navigation layer builds on device handling by introducing anatomical pathways. Trainees learn to guide their scope through relevant structures. For upper endoscopy that means passing the cricopharyngeus , navigating the esophagus , entering the stomach , and reaching the duodenum. For colonoscopy it involves progressing from rectum to cecum while managing loops and angulations.
Navigation training emphasizes landmark recognition and spatial orientation. Trainees learn what structures look like , how to identify their position , and how to correct course when they encounter difficulties. Simulators can present standardized anatomy that allows systematic skill development before trainees face the natural variation present in actual patients.
The diagnostic layer adds clinical decision making. Trainees learn to recognize normal versus abnormal findings. They practice systematic examination techniques that ensure complete visualization. They develop pattern recognition for common pathology. This layer integrates the technical skills from earlier stages with the cognitive skills required for clinical practice.
The therapeutic layer introduces interventional techniques. Depending on the procedure type , this might include biopsy , polypectomy , bleeding control , tissue resection , or device placement. Each therapeutic skill requires its own stepwise development. A trainee learning polypectomy , for example , progresses from understanding principles to practicing snare placement to performing actual tissue removal under supervision.
Advanced therapeutic training often requires specialized simulators. For endoscopic submucosal dissection , the GI ESD Surgical Simulator allows trainees to practice the precise dissection techniques required without risk of perforation or bleeding complications in actual patients.
Deliberate Practice in Procedure Training
Not all practice produces improvement. Mindless repetition can actually reinforce bad habits. Effective procedure training requires what researchers call deliberate practice , which involves several key elements.
Clear objectives define what the trainee should accomplish in each session. Rather than vague goals like "get better at colonoscopy" , objectives specify measurable targets like "achieve cecal intubation within 15 minutes in 90% of simulated cases" or "perform snare polypectomy with clean margins on five consecutive polyps."
Focused repetition concentrates practice on specific skills. If a trainee struggles with loop reduction during colonoscopy , they spend dedicated time practicing that particular technique rather than running through complete procedures where the problem skill gets limited attention.
Immediate feedback tells trainees how they're performing. Many simulators provide automated metrics , but instructor feedback remains essential for interpreting performance and suggesting improvements. According to the NCBI Bookshelf resource on mastery learning , the combination of deliberate practice with structured feedback produces superior outcomes compared to traditional teaching approaches.
Progressive challenge prevents plateaus. Once trainees master basic scenarios , they encounter increasingly difficult cases. Simulators can present challenging anatomy , introduce complications , or add time pressure to push trainees toward higher performance levels.
Procedure Training Across Medical Specialties
While gastroenterology provides many examples , stepwise procedure training applies across medical specialties.
In pulmonology , bronchoscopy training follows similar principles. Trainees start with basic scope handling , progress to airway navigation , and eventually perform therapeutic interventions. Bronchoscopy simulators such as the Bronchoscopy Simulator Type A , Type B , and Type C allow trainees to practice navigating the tracheobronchial tree before examining actual patients. The Ultrasound Bronchoscopy Simulator adds the complexity of endobronchial ultrasound interpretation for trainees advancing to that technique.
Urological endoscopy presents unique challenges due to smaller caliber instrumentation and delicate structures. The Urological Endoscopy Simulator supports cystoscopy and ureteroscopy skill development. For ultrasound-guided procedures , the Prostate Ultrasound Simulator allows practice integrating imaging with procedural technique.
Gynecological procedures benefit from dedicated training tools. Hysteroscopy requires navigating the uterine cavity and performing various diagnostic and therapeutic maneuvers. The Hysteroscopy Simulator provides realistic practice opportunities for trainees developing these skills.
Surgical specialties increasingly use simulation for laparoscopic skill development. The Laparoscopy Simulator allows trainees to practice instrument handling , camera navigation , and basic surgical maneuvers before performing procedures on patients.
Spine surgery has also embraced simulation training. Endoscopic spine procedures require precise technique in confined anatomical spaces. The Intervertebral Foramen Endoscope Simulator supports training in these specialized techniques.
Integrating Simulation with Clinical Training
Simulators don't replace clinical experience. They prepare trainees to maximize learning from patient encounters. The most effective training programs integrate simulation and clinical practice strategically.
Pre-clinical simulation establishes foundational skills before patient contact. Trainees arrive for their first clinical procedures already comfortable with basic device handling and familiar with expected anatomy. This reduces anxiety and allows them to focus on aspects of the procedure that can only be learned with real patients.
Concurrent simulation addresses specific deficiencies identified during clinical work. A trainee struggling with a particular technique can return to the simulator for focused practice. This targeted approach is more efficient than simply hoping improvement happens through additional clinical volume.
Maintenance simulation keeps skills sharp for rarely performed procedures. Some techniques occur infrequently in clinical practice. Without periodic refresher training , skills can decay. Simulation provides the repetitive exposure needed to maintain competence even when clinical opportunities are limited.
Assessment and Progression
Structured procedure training requires systematic assessment to determine when trainees are ready to progress. Simple procedure counts don't reliably indicate competence. Two trainees with identical case numbers may have very different skill levels.
Modern training programs use validated assessment tools that measure specific performance elements. For endoscopy , tools like the Direct Observation of Procedural Skills capture both technical proficiency and decision making quality. Simulators can provide objective metrics like completion time , wall contact events , and anatomical completeness of examination.
Mastery-based progression means trainees advance when they demonstrate competence , not when they accumulate a predetermined number of cases. This approach ensures all graduates meet minimum standards while allowing faster learners to progress efficiently.
Simulator Training from Suzhou Frank Medical
At Suzhou Frank Medical , we manufacture a comprehensive range of procedure training simulators designed to support stepwise skill development across medical specialties. Our products include models for gastrointestinal endoscopy , bronchoscopy , urological procedures , gynecological interventions , laparoscopic surgery , and spine procedures. Each simulator is built to provide realistic practice opportunities that accelerate learning curves and prepare trainees for clinical success.
We understand that different training programs have different needs. Whether you're establishing a new simulation center or adding capabilities to an existing program , we can help identify the right products for your educational goals. Browse our complete endoscopic intervention training model catalog to explore available options , or contact us to discuss your specific requirements.
Building Competence Through Structure
Procedure training has evolved beyond the apprenticeship model. Simulators enable the deliberate practice that research shows produces superior outcomes. Stepwise skill building allows trainees to master components before integrating them into complete procedures. And structured assessment ensures progression reflects actual competence rather than arbitrary benchmarks.
For training programs committed to producing skilled practitioners , simulation-based stepwise training is no longer optional. It's the standard that prepares trainees to deliver safe , effective care from their first independent procedure forward.
© 2025. All rights reserved.
About Us
Introduction
Development
Cooperation
Service
Main Products
Medical Grade Monitor
No 15, Jinyang road KunshanSuzhou, Jiangsu, China
