📞Customer Service: +86 13248368268 📧servicecenter@suzhoufrank.com one year replacement and warranty!
Resident Training in GI Endoscopy: Role of Simulation
Resident training in endoscopy no longer means learning on patients first. See how simulation prepares residents for safer, faster skill development.
MEDICAL IMAGING
Dr Qi Rui
1/27/20265 min read
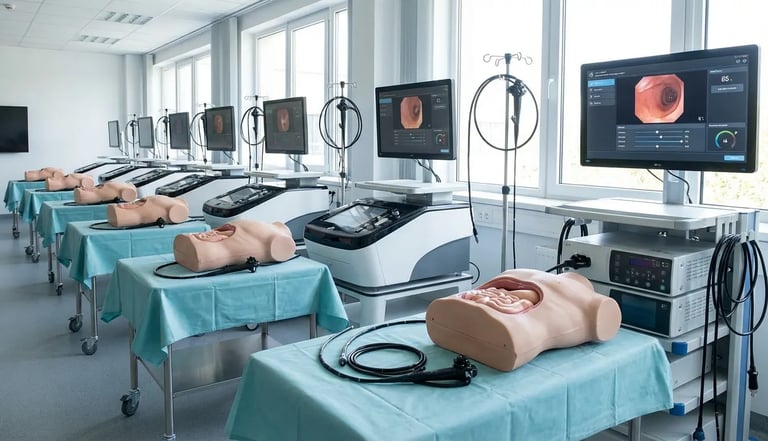
Learning to perform endoscopy on real patients is inherently difficult. Residents must develop hand-eye coordination, spatial awareness, and procedural judgment while managing patient comfort and safety. The traditional apprenticeship model — watch one, do one, teach one — puts patients at risk during the learning curve and provides inconsistent training experiences. Simulation changes this equation by giving residents a safe environment to build foundational skills before they ever hold a scope near a patient.
This guide examines how resident training in GI endoscopy works, where simulation fits into the curriculum, and how programs use simulators to prepare residents for supervised clinical cases.
The Challenge of Teaching Endoscopy to Residents
Endoscopy requires a combination of cognitive knowledge, technical skill, and clinical judgment that takes time to develop. Residents must learn to navigate three-dimensional anatomy while watching a two-dimensional screen, interpret what they see in real time, and perform therapeutic interventions when needed. These skills do not develop overnight.
The traditional training model poses several problems. When residents learn primarily on patients, those patients experience longer procedure times, more discomfort, and potentially higher complication rates. Faculty must balance teaching with patient care, often sacrificing educational moments to maintain efficiency. And residents receive inconsistent exposure depending on case mix and scheduling.
According to a systematic review published in Clinical Gastroenterology and Hepatology, simulation-based training creates an ideal environment where trainees can practice specific skills, perform cases at their own pace, and make mistakes with no risk to patients. Educators benefit because they can focus solely on teaching without the competing demands of patient care.
Where Simulation Fits in the Curriculum
Effective resident training integrates simulation at specific points where it provides the most value. Most programs use simulation early in training to establish foundational skills before clinical exposure begins.
Pre-clinical simulation focuses on basic scope handling. Residents learn how control inputs translate to tip movement, how to maintain orientation, and how to navigate anatomical turns. The GI Endoscopy Simulator provides anatomically accurate pathways where residents can practice these fundamentals repeatedly until the movements become automatic.
Once residents begin supervised patient procedures, simulation shifts to a complementary role. Residents can use simulators to practice specific maneuvers they found difficult during clinical cases. They can work through challenging anatomy without time pressure. They can prepare for upcoming procedures by rehearsing similar cases on simulators first.
Advanced simulation addresses therapeutic techniques. Polypectomy, hemostasis, and complex interventions require precise movements that are risky to learn on patients. The GI ESD Surgical Simulator allows residents to develop dissection skills for advanced resection techniques in a controlled environment.
Structured Curricula Versus Open Practice
Simply giving residents access to simulators does not guarantee learning. Research consistently shows that simulation without structure, feedback, and defined objectives produces minimal benefit. A 2004 study found that residents practicing on colonoscopy simulators without any feedback showed no improvement in their skills.
Effective simulation curricula incorporate several key elements. Clear learning objectives define what residents should accomplish in each session. Progressive difficulty ensures residents are appropriately challenged as their skills develop. Structured feedback from faculty helps residents identify and correct errors. Assessment tools document progress toward competency.
The ASGE has developed the Skills, Training, Assessment, and Reinforcement program that combines hands-on simulation training with formative feedback and structured assessments. Programs adopting similar structured approaches see better transfer of simulation skills to clinical performance.
From Simulator to Patient
The transition from simulation to supervised patient cases requires careful management. Residents who have developed basic skills on simulators still face new challenges when working with real patients. Anatomy varies. Patients move and respond to discomfort. Time pressure exists. The clinical environment adds complexity that simulation cannot fully replicate.
Effective programs use simulation to reduce the initial learning curve, not replace clinical training. A resident who has already learned basic scope manipulation on a simulator can focus on patient-specific factors during their first supervised cases. They spend less time struggling with basic technique and more time developing clinical judgment.
Some programs implement "just-in-time" simulation, where residents practice on simulators immediately before clinical sessions. This warm-up approach helps residents refresh their skills and mentally prepare for the procedures ahead. Studies in other procedural domains show that pre-procedure simulation practice improves subsequent clinical performance.
Feedback and Debriefing
Feedback drives improvement in simulation-based training. Residents need specific, actionable information about their performance to know what to change. Generic praise or criticism provides little educational value.
Effective feedback in endoscopy simulation addresses both what residents did and why it matters. Rather than simply noting that a resident took too long to navigate a flexure, faculty explain what technique would work better and demonstrate alternatives. Video review allows residents to see their own performance and compare it to expert technique.
Debriefing after simulation sessions creates space for reflection. Residents discuss what went well, what proved difficult, and what they plan to work on next. This reflective practice helps residents develop the self-assessment skills they will need throughout their careers.
Simulation Across Endoscopic Subspecialties
While GI endoscopy provides the primary focus for gastroenterology residents, simulation principles extend across all endoscopic training. Pulmonary medicine residents learning bronchoscopy benefit from the same structured approach. Simulators like the Bronchoscopy Simulator Type A and Type B allow airway navigation practice before clinical cases. The Ultrasound Bronchoscopy Simulator addresses the combined skills needed for EBUS procedures.
Surgical residents often receive endoscopy training as part of their curriculum. The Laparoscopy Simulator builds foundational camera navigation and instrument handling skills that transfer to flexible endoscopy. Urology residents learning cystoscopy can use the Urological Endoscopy Simulator to develop skills specific to their specialty.
For comprehensive information on building simulation into endoscopy training, see our complete guide to medical simulation in endoscopy and GI training.
Simulation Equipment from Suzhou Frank Medical
At Suzhou Frank Medical, we manufacture simulation equipment designed to support resident training programs across endoscopic specialties. Our simulators provide the anatomical accuracy and durability that intensive training demands. When programs need equipment that can handle daily use by multiple residents while delivering consistent educational experiences, build quality matters.
Explore our complete endoscopic intervention training model catalog to see the full range of training options available. For questions about specific applications or to discuss how our simulators might fit your program's needs, contact us directly.
Frequently Asked Questions
When should residents start simulation training? Most programs introduce simulation at the very beginning of endoscopy training, before any patient contact. This allows residents to develop basic scope handling skills in a risk-free environment. Early simulation exposure means residents arrive at their first supervised patient cases with foundational competencies already established.
How much simulation time do residents need? Research suggests that distributed practice over time produces better results than concentrated sessions. Rather than a single intensive simulation boot camp, programs see better outcomes when residents have regular access to simulators throughout their training. Even brief practice sessions before clinical rotations help maintain and reinforce skills.
Can simulation replace clinical training? No. Simulation complements clinical training but cannot replace it. Patients present variability, complexity, and real-world pressures that simulation cannot fully replicate. The goal is to use simulation to accelerate the early learning curve so residents can focus on higher-level skills during clinical cases.
What makes simulation training effective? Structure, feedback, and clear objectives matter more than simulator fidelity. Residents need defined learning goals, progressive challenges, expert feedback, and opportunities for deliberate practice. Simply providing simulator access without these elements produces minimal educational benefit.
© 2025. All rights reserved.
About Us
Introduction
Development
Cooperation
Service
Main Products
Medical Grade Monitor
No 15, Jinyang road KunshanSuzhou, Jiangsu, China
