📞Customer Service: +86 13248368268 📧servicecenter@suzhoufrank.com one year replacement and warranty!
Designing a Simulation Curriculum for Endoscopy Training
Simulation curriculum design for endoscopy training requires progressive skill building, validated assessments, and structured feedback. Learn key implementation strategies.
MEDICAL TRAINING
Dr Qi Rui
3/5/20265 min read
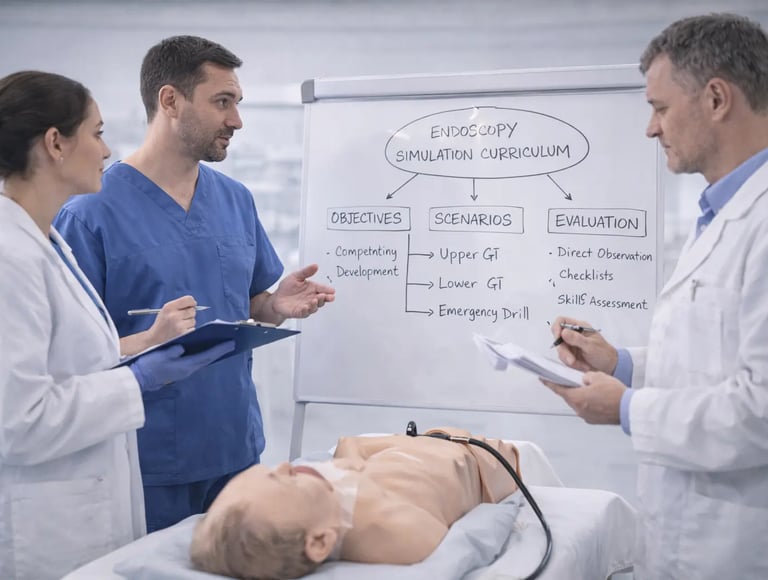
Building a simulation curriculum for endoscopy training requires more than purchasing equipment and scheduling practice sessions. Programs that treat simulation as an add-on rather than an integrated educational experience often see limited returns on their investment. The difference between effective and ineffective simulation training comes down to curriculum design—how learning objectives connect to specific simulator exercises, when trainees progress to more complex tasks, and how feedback shapes skill development over time.
The traditional approach to endoscopy education followed an apprenticeship model where trainees observed procedures, then performed them under supervision until they accumulated enough cases to demonstrate competence. This model has well-documented limitations. Trainees learn at different rates, supervisors have varying teaching styles, and patient complexity introduces unpredictable variables into the learning process. A 2022 review in the World Journal of Gastrointestinal Endoscopy noted that the apprenticeship model produces variable skill outcomes and has come under scrutiny for patient safety implications.
Simulation curriculum design addresses these limitations by providing standardized training experiences with measurable outcomes. For a comprehensive overview of how simulation fits into broader endoscopy education, see our complete guide to medical simulation in endoscopy and GI training.
Foundational Elements of Curriculum Design
Effective simulation curricula share several structural elements regardless of the specific procedures they target. The first is clearly defined learning objectives organized in a progressive sequence. Novice trainees need different skill targets than those preparing for advanced therapeutic techniques, and the curriculum must reflect this progression.
A 2020 study published in BMC Medical Education described a proficiency-based curriculum for upper GI endoscopy that divided training into cognitive, technical, and non-technical components. Trainees worked through scope navigation, anatomical landmark identification, mucosal inspection, retroflexion, pathology recognition, and targeted biopsy in sequence. Each component had specific proficiency benchmarks that trainees needed to achieve before advancing.
The second foundational element involves matching simulator fidelity to learning stage. Early training benefits from lower-fidelity models that isolate specific skills like scope manipulation and torque steering. As trainees develop foundational abilities, they progress to higher-fidelity simulators that integrate multiple skill domains and present realistic procedural challenges. For programs building upper and lower GI training capabilities, the Gastrointestinal Endoscopy Simulator provides the anatomical accuracy needed for both basic and intermediate skill development.
Upper GI Endoscopy Curriculum Components
Esophagogastroduodenoscopy training typically begins with orientation to endoscope mechanics—understanding control wheel function, insertion tube handling, and video system operation. These sessions can use tabletop trainers or simple bench models before trainees work with anatomical simulators.
The next phase focuses on navigation skills: advancing the scope through the esophagus, identifying the gastroesophageal junction, entering the stomach, and maneuvering through the pylorus into the duodenum. Retroflexion in the stomach presents particular challenges that benefit from repetitive practice. Trainees often struggle with the coordinated wheel manipulation required to achieve adequate retroflexed views, and simulation allows them to repeat this maneuver until it becomes intuitive.
Mucosal inspection skills develop alongside navigation abilities. Trainees learn systematic examination patterns that ensure complete visualization while avoiding blind spots. Documentation skills—capturing appropriate still images of landmarks and pathology—become part of the curriculum once trainees demonstrate basic navigation competency.
Therapeutic Technique Integration
As trainees master diagnostic techniques, the simulation curriculum expands to include therapeutic interventions. Biopsy sampling, hemostasis techniques, and mucosal resection each require dedicated training modules. The Gastrointestinal ESD Surgical Simulator supports programs teaching endoscopic submucosal dissection, one of the more demanding therapeutic techniques in GI endoscopy.
Therapeutic simulation presents unique curriculum design challenges. These procedures carry higher complication risks than diagnostic endoscopy, making the transition from simulation to patient care particularly important. Programs often implement graduated supervision protocols where trainees demonstrate consistent simulator performance before attempting procedures on patients, then receive intensive oversight during their initial clinical cases.
Research published in Frontline Gastroenterology emphasized that simulation without feedback from instructors may be ineffective. The authors noted that structured debriefing sessions—where trainees and instructors review performance, identify gaps, and establish improvement targets—significantly enhance skill transfer to clinical settings. This finding has important implications for curriculum design: programs must allocate instructor time for feedback, not just simulator access time for trainees.
Cross-Specialty Curriculum Considerations
While GI endoscopy represents the largest training volume, simulation curriculum principles apply across endoscopic specialties. Bronchoscopy training programs face similar challenges in developing navigation skills, lesion recognition, and sampling techniques. The Ultrasound Bronchoscopy Simulator addresses the growing importance of endobronchial ultrasound in pulmonary medicine, while traditional navigation skills can be developed using bronchoscopy trainers like the Bronchoscopy Simulator Type A and Type B models.
Urological endoscopy presents its own curriculum requirements. Cystoscopy, ureteroscopy, and transurethral resection procedures demand specific skill sets that differ from GI applications. Programs incorporating urological training can utilize the Urological Endoscopy Simulator to build technique before patient contact.
Gynecological endoscopy rounds out the cross-specialty picture. Hysteroscopy training shares characteristics with other endoscopic procedures—navigation through anatomical structures, visualization techniques, and sampling or therapeutic interventions—while requiring familiarity with female reproductive anatomy. The Hysteroscopy Simulator provides realistic training for diagnostic and operative hysteroscopy procedures.
Deliberate Practice and Mastery Learning
Two educational concepts shape modern simulation curriculum design: deliberate practice and mastery learning. Deliberate practice involves focused repetition of specific skills with immediate feedback and correction. Unlike simple repetition, deliberate practice requires trainees to work at the edge of their current abilities, identify errors, and make targeted improvements.
Mastery learning extends this concept by establishing minimum performance standards that all trainees must achieve before advancing. Rather than allowing trainees to progress based on time spent or procedures completed, mastery learning requires demonstrated competence. This approach reduces variability in trainee outcomes—everyone who completes the curriculum meets the same performance benchmarks.
Implementing mastery learning requires validated assessment tools that measure performance reliably. Several assessment instruments have been developed for GI endoscopy, including the Gastrointestinal Endoscopy Competency Assessment Tool and the Mayo Colonoscopy Skills Assessment Tool. These instruments provide objective measures that support mastery learning curriculum design.
Assessment and Progression Protocols
The simulation curriculum must define how trainee progress will be measured and what triggers advancement to subsequent training phases. Formative assessments during training help trainees identify areas needing improvement, while summative assessments at phase completion determine readiness to advance.
Assessment frequency matters. Programs that evaluate trainees only at curriculum endpoints miss opportunities for early intervention when trainees struggle with specific skills. Frequent low-stakes assessments create feedback loops that accelerate learning and identify problems before they compound.
Documentation of trainee progress serves multiple purposes: it guides individual training plans, demonstrates program effectiveness for accreditation, and provides evidence of competency for credentialing purposes. Digital tracking systems can aggregate performance data across trainees and over time, revealing curriculum elements that consistently challenge trainees or produce strong outcomes.
Suzhou Frank Medical: Supporting Simulation Curriculum Development
At Suzhou Frank Medical, we manufacture simulation equipment designed to support comprehensive endoscopy training curricula. Our simulators provide the anatomical accuracy and build quality that structured training programs require. Equipment designed for curriculum use faces intensive daily demands—multiple trainees practicing repeatedly across extended training periods—and durability matters as much as realism.
Programs developing or expanding simulation curricula can view our complete range of endoscopic intervention training models to identify equipment matching their specific training objectives. For questions about equipment specifications or curriculum support, please contact us directly.
Implementation Considerations
Starting a simulation curriculum requires institutional commitment beyond equipment procurement. Faculty development ensures instructors can deliver effective feedback and facilitate debriefing sessions. Protected time for simulation sessions—both trainee practice and supervised instruction—must be built into training schedules. Physical space considerations include storage for simulators, room availability for training sessions, and integration with existing education facilities.
Successful programs typically start with focused curricula targeting specific procedures or skill sets, then expand as faculty expertise and institutional capacity develop. This measured approach allows programs to refine curriculum elements based on early experience before scaling to more comprehensive training offerings.
© 2025. All rights reserved.
About Us
Introduction
Development
Cooperation
Service
Main Products
Medical Grade Monitor
No 15, Jinyang road KunshanSuzhou, Jiangsu, China
