📞Customer Service: +86 13248368268 📧servicecenter@suzhoufrank.com one year replacement and warranty!
Skills Assessment in Simulation-Based Training
Skills assessment transforms medical simulation from practice into accountability. Discover evaluation methods that ensure trainees are ready for real patient care.
MEDICAL TRAINING
Dr Qi Rui
1/23/20265 min read
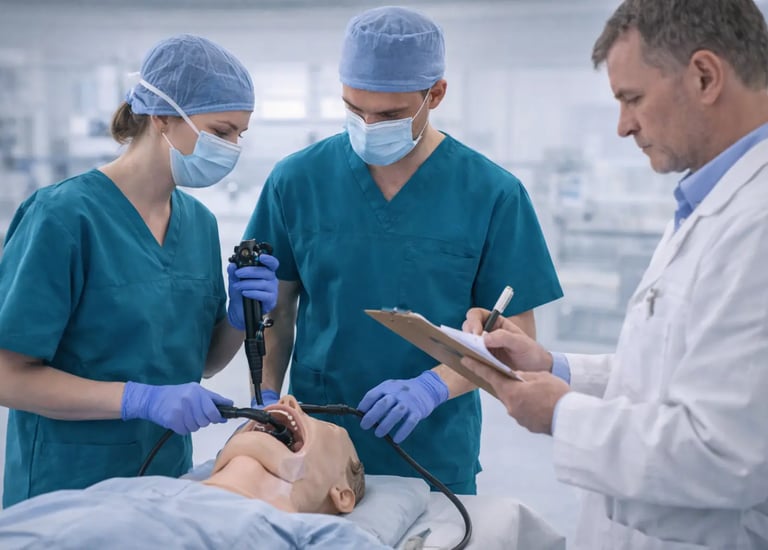
Medical education has shifted from subjective evaluations to structured, measurable approaches. Skills assessment in simulation-based training provides the objective framework needed to determine whether trainees can actually perform clinical tasks safely and effectively. Without reliable assessment methods, simulation remains practice without purpose. With them, training programs can document competency, identify gaps, and ensure patient safety before trainees ever touch a real patient.
This guide explores how skills assessment works within simulation environments, covering evaluation frameworks, scoring methodologies, and the tools that make objective measurement possible across technical and non-technical domains.
Why Skills Assessment Matters in Simulation
Traditional clinical evaluation relied heavily on expert opinion. An attending physician would watch a trainee perform a procedure and make a judgment call. The problem with this approach is variability. Research from the National Board of Medical Examinations found that correlation between independent evaluations by two examiners was often less than 0.25. One examiner's pass could easily be another's fail.
Simulation-based training solves part of this problem by creating controlled, repeatable scenarios. But simulation without structured assessment is just expensive practice. Skills assessment transforms simulation from activity into accountability. It answers the essential question: can this trainee perform this skill to the required standard?
According to AHRQ's Patient Safety Network, simulation has been successfully applied for both formative experiences to develop clinical skills and summative assessments to verify competency. The combination of realistic practice environments with objective measurement creates a powerful system for ensuring healthcare professionals meet defined standards before caring for patients.
Technical Skills Assessment
Technical skills form the foundation of procedural medicine. In endoscopy, this means scope manipulation, tissue recognition, and therapeutic interventions. In surgery, it encompasses instrument handling, tissue dissection, and hemostasis. Each specialty has core technical competencies that trainees must master.
Assessment of technical skills in simulation typically uses task-specific checklists. These checklists break complex procedures into discrete, observable steps. For a colonoscopy, the checklist might include scope insertion technique, navigation through flexures, mucosal inspection patterns, and retroflexion maneuvers. Each step receives a score based on whether it was performed correctly, partially, or not at all.
Global rating scales complement checklists by capturing overall performance quality. Rather than marking individual steps, global scales assess dimensions like efficiency of movement, instrument handling, and flow of procedure. A trainee might complete all checklist items but do so with excessive scope looping and patient discomfort. Global ratings capture these qualitative differences.
The GI Endoscopy Simulator supports technical skills assessment by providing consistent anatomical challenges across trainees. When everyone navigates the same anatomy, performance differences reflect actual skill levels rather than case variation. For advanced therapeutic techniques, the GI ESD Surgical Simulator allows assessment of precise dissection skills that would be difficult to evaluate safely on real patients during training.
The Objective Structured Clinical Examination
The Objective Structured Clinical Examination represents the gold standard for simulation-based skills assessment. First described by Harden in 1975, the OSCE has become a required component of medical training programs worldwide. According to a comprehensive review published in PMC, the OSCE assesses competency based on objective testing through direct observation, covering areas critical to healthcare performance that traditional examinations cannot evaluate.
An OSCE consists of multiple stations where trainees rotate through standardized scenarios. Each station tests specific competencies using predetermined criteria and typically lasts five to fifteen minutes. Trained assessors use standardized marking schemes to evaluate performance, ensuring all trainees face the same challenges and are judged against identical standards.
The structure makes OSCE particularly valuable for comprehensive competency assessment. A single examination can test technical procedures, communication skills, clinical reasoning, and professional behavior. Stations can incorporate standardized patients, task trainers, and high-fidelity mannequins, allowing assessment of the full range of skills trainees need.
Non-Technical Skills Assessment
Clinical competence extends beyond procedural technique. Communication, teamwork, situational awareness, and decision making all influence patient outcomes. These non-technical skills prove equally important but more difficult to measure than technical performance.
Behavioral rating systems have emerged to assess non-technical skills. The Anaesthetists' Non-Technical Skills framework evaluates task management, team working, situation awareness, and decision making. Similar frameworks exist for surgery, emergency medicine, and other specialties.
Team-based simulations provide opportunities to assess interprofessional competencies. When an endoscopy team manages a simulated complication, assessors evaluate not just technical response but the entire team's communication, role clarity, and coordination.
Scoring Systems and Rubrics
Effective skills assessment requires well-designed scoring instruments. Binary checklists mark items as done or not done. This approach works well for procedures with clear required steps but fails to capture performance quality. A trainee who performs all steps clumsily scores the same as one who performs them expertly.
Likert scales address this limitation by allowing graded responses. A five-point scale might range from "not done or done incorrectly" through "done correctly with expert technique." This captures the difference between minimal competency and true proficiency. However, Likert scales require clear anchors defining each level to maintain inter-rater reliability.
Anchored rating scales provide the most robust measurement. Each score level includes specific behavioral descriptions. Rather than asking assessors to judge "communication quality" on a generic scale, anchored instruments describe exactly what communication looks like at each level. This specificity improves agreement between different assessors evaluating the same performance.
Assessment Across Specialties
Skills assessment principles apply across all procedural specialties, though specific tools must match specialty requirements. Bronchoscopy training uses simulators like the Bronchoscopy Simulator Type A, Type B, and Type C to assess airway navigation and sampling techniques. For endobronchial ultrasound procedures, the Ultrasound Bronchoscopy Simulator enables assessment of combined imaging and procedural skills.
Urological procedures present unique assessment challenges due to delicate anatomy and limited working space. The Urological Endoscopy Simulator supports evaluation of cystoscopy and ureteroscopy skills. Prostate procedures requiring ultrasound guidance can be assessed using the Prostate Ultrasound Simulator.
Gynecological endoscopy has its own competency requirements. The Hysteroscopy Simulator allows assessment of intrauterine navigation and therapeutic techniques. Laparoscopic skills foundational to many surgical specialties can be evaluated using the Laparoscopy Simulator.
Formative Versus Summative Assessment
Skills assessment serves two distinct purposes. Formative assessment supports learning by providing detailed feedback during training. After a simulated procedure, trainees learn what they did well and what needs improvement. The goal is development, not judgment.
Summative assessment carries stakes. It determines whether trainees can progress, perform procedures independently, or obtain certification. These assessments require higher standards for reliability because decisions affect careers and patient safety. Most programs use summative simulation assessments as one component of broader competency evaluation alongside clinical performance and written examinations.
Implementing Skills Assessment Programs
Successful skills assessment requires more than good instruments. Programs must train assessors to use scoring tools consistently. Calibration sessions where multiple assessors score the same performances help identify and correct inconsistencies.
Standard setting establishes the boundary between competent and not-yet-competent performance. Documentation systems allow programs to monitor trainee progress over time, revealing learning trajectories and identifying those who need additional support. For comprehensive guidance on building simulation training programs, see our complete guide to medical simulation in endoscopy and GI training.
Skills Assessment Equipment from Suzhou Frank Medical
At Suzhou Frank Medical, we manufacture simulation equipment designed to support rigorous skills assessment across endoscopic and interventional specialties. Our simulators provide the anatomical accuracy and consistent performance characteristics that valid assessment requires. When assessment results need to reflect actual trainee capabilities rather than equipment variation, quality simulation matters.
Programs building or expanding their skills assessment capabilities can explore our complete endoscopic intervention training model catalog. For questions about specific assessment applications or to discuss how our simulators might support your program's evaluation needs, please contact us directly.
The Future of Skills Assessment
Skills assessment in simulation continues to evolve. Automated performance metrics captured directly from simulators reduce reliance on human observers. Motion analysis, force measurement, and procedure timing provide objective data that complement expert evaluation.
Competency-based medical education frameworks increasingly mandate documented skills assessment before trainees advance. As these frameworks mature, skills assessment in simulation will become not just beneficial but required. The fundamental principle remains unchanged: assessment transforms simulation from activity into accountability, ensuring trainees are truly ready to care for patients.
© 2025. All rights reserved.
About Us
Introduction
Development
Cooperation
Service
Main Products
Medical Grade Monitor
No 15, Jinyang road KunshanSuzhou, Jiangsu, China
