📞Customer Service: +86 13248368268 📧servicecenter@suzhoufrank.com one year replacement and warranty!
What Is an Endoscopy Simulator? Types, Uses, and Benefits
Endoscopy simulator guide covering types , training uses and benefits. Understand how simulators help trainees build skills safely before patient procedures.
MEDICAL TRAINING
Dr Qi Rui
1/19/20268 min read
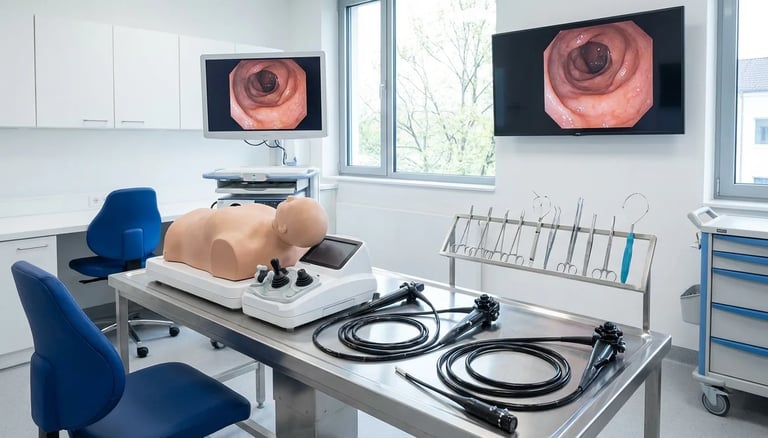
Learning to perform endoscopy presents a fundamental challenge. The procedures require complex psychomotor skills , anatomical knowledge and split-second decision-making , yet traditional training happens on real patients where mistakes carry consequences. An endoscopy simulator offers a solution: a training platform where learners develop competence before ever touching a patient.
This guide explains what endoscopy simulators are , describes the main types available , explores how training programs use them and outlines the benefits they provide for learners , educators and ultimately patients.
Defining the Endoscopy Simulator
An endoscopy simulator is any device or system designed to replicate the experience of performing endoscopic procedures for educational purposes. These training tools range from simple mechanical models to sophisticated computer-based systems that create immersive virtual experiences.
The core purpose remains consistent across all types: allow trainees to practice endoscopic skills in environments where errors carry no patient risk. This fundamental principle drives the growing adoption of simulation throughout medical education.
For a comprehensive overview of how simulation fits into broader gastroenterology education , our guide on medical simulation in endoscopy and GI training provides detailed context on curriculum integration , competency frameworks and evidence supporting simulation-based education.
Why Endoscopy Simulators Matter
Traditional endoscopy training followed an apprenticeship model. Trainees learned by performing procedures on patients under supervision , gradually taking more responsibility as skills developed. This approach worked but created tension between educational needs and patient welfare.
Every procedure performed by a learning trainee takes longer , may cause more discomfort and carries slightly higher complication risk than procedures performed by experienced endoscopists. Patients essentially subsidize trainee education with their bodies. While supervision mitigates risks , the ethical tension remains.
Research published in PMC confirms that simulation-based training improves learning outcomes and performance in clinical settings while offering unique advantages to both trainees and educators. Simulation creates environments where trainees can practice specific skills , perform cases at their own pace and make mistakes without patient consequences.
An endoscopy simulator shifts the earliest , most error-prone learning phases away from patients entirely. Trainees build foundational skills , develop muscle memory and learn to recognize anatomy before their first clinical procedure. When they do begin patient-based training , they arrive with baseline competencies that make learning more efficient and safer.
Types of Endoscopy Simulators
Understanding the categories of endoscopy simulators helps programs select appropriate tools for specific training objectives. Each type offers distinct advantages suited to different learning goals.
Mechanical Simulators
Mechanical simulators use physical models to replicate anatomical structures. These range from simple tube-based trainers to anatomically accurate organ reproductions that mimic tissue properties , structural landmarks and pathological findings.
The simplest mechanical endoscopy simulator might consist of a flexible tube through which trainees practice scope navigation. More sophisticated versions recreate complete upper or lower GI tract anatomy with realistic tissue texture , appropriate resistance and visual landmarks matching human anatomy.
Our gastrointestinal endoscopy simulator provides this kind of anatomically accurate training environment. Trainees practice navigation , visualization techniques and basic scope handling on models that respond like real tissue.
Mechanical simulators excel at developing fundamental psychomotor skills. The tactile experience of manipulating a real endoscope through physical structures builds hand-eye coordination and scope control that transfer directly to clinical practice.
Advantages of mechanical simulators include relatively lower cost compared to virtual reality systems , no requirement for specialized software or technical support , and highly realistic tactile feedback. Limitations include inability to present case variety without physical model changes and lack of automated performance metrics.
Virtual Reality Simulators
Virtual reality (VR) endoscopy simulators use computer graphics and haptic feedback devices to create immersive procedural experiences. Trainees manipulate controllers that provide force feedback while viewing computer-generated anatomical environments on screens.
VR systems offer capabilities impossible with mechanical trainers. They can present unlimited case variety , from routine normal examinations to rare pathology and emergency complications. Performance metrics are captured automatically: procedure time , scope positioning , forces applied , completeness of examination and dozens of other parameters.
According to research in PMC , over 21 randomized controlled trials have investigated virtual reality simulation as a teaching tool in endoscopy. Studies consistently show that trainees using VR simulation-based learning improve in technical skills , non-technical abilities and patient comfort measures during the early learning process.
VR simulators particularly excel at cognitive training. Trainees learn to recognize pathology , make diagnostic decisions and respond to complications in scenarios that can be repeated until mastery is achieved. The same rare emergency can be practiced dozens of times , building response patterns that might take years to develop through clinical exposure alone.
The primary limitation of VR systems is cost. High-fidelity platforms require substantial investment in hardware , software licensing and ongoing maintenance. Additionally , while haptic technology continues improving , VR tactile feedback still doesn't perfectly replicate real tissue properties.
Hybrid Simulators
Hybrid systems combine elements of mechanical and virtual reality approaches. A trainee might manipulate a real endoscope through a physical model while viewing computer-enhanced imagery that adds virtual pathology , bleeding or other clinical scenarios.
These systems attempt to capture the realistic tactile experience of mechanical models while gaining the case variety and metrics capabilities of VR platforms. Development in this space continues as technologies mature and integration improves.
Ex Vivo and Animal Models
Some training programs use explanted animal organs or specially prepared tissue specimens as simulation platforms. These provide highly realistic tissue properties that synthetic materials cannot fully replicate.
Ex vivo models excel for therapeutic technique training where tissue response matters critically. Techniques like polypectomy , hemostasis and mucosal resection benefit from practice on real tissue before clinical application.
Limitations include the need for special handling and storage , limited reuse potential , ethical considerations and variable quality between specimens. Many programs use ex vivo models selectively for advanced techniques rather than foundational training.
Task Trainers
Task trainers focus on specific procedural components rather than complete procedures. Instead of simulating an entire colonoscopy , a task trainer isolates polypectomy technique , clip placement , injection methods or specific therapeutic maneuvers.
This modular approach aligns well with competency-based education. Trainees can concentrate intensive practice on specific skills requiring development without spending time on components already mastered.
For advanced therapeutic techniques , our gastrointestinal ESD surgical simulator provides focused training for endoscopic submucosal dissection. This technically demanding procedure requires extensive practice before clinical application , and dedicated task trainers address that need specifically.
How Training Programs Use Endoscopy Simulators
Effective simulation integration requires thoughtful curriculum design , not merely simulator availability. Programs use endoscopy simulators across multiple educational contexts.
Pre-Clinical Foundation Building
Before trainees perform their first patient procedures , simulation establishes foundational skills. New fellows or residents spend structured time on simulators learning scope manipulation , anatomical orientation and basic techniques.
This approach ensures all trainees begin clinical rotations with consistent baseline competencies regardless of prior exposure. Programs report that simulation-prepared trainees require less intensive supervision during initial clinical procedures and progress more quickly toward independence.
Deliberate Practice
Deliberate practice involves focused , repetitive work on specific skills with immediate feedback. Unlike general experience accumulation , deliberate practice targets identified weaknesses and pushes trainees beyond current comfort levels.
Endoscopy simulators enable deliberate practice that would be impractical or unethical on patients. A trainee struggling with retroflexion can perform that maneuver fifty times in a simulator session. Someone needing work on loop reduction can practice repeatedly until the technique becomes automatic.
Rare Scenario Exposure
Some clinical scenarios occur too infrequently for trainees to encounter reliably during training. Massive bleeding , perforation recognition , foreign body removal and other emergencies require immediate competent response but may happen only occasionally.
Simulators allow programs to ensure all trainees encounter and practice managing rare scenarios. The complications that might occur once in a fellowship year can be practiced weekly on simulators until responses become reflexive.
Objective Assessment
Competency-based education requires objective assessment of whether trainees can perform expected tasks. Traditional assessment relied heavily on subjective evaluations by supervising physicians who might observe only portions of procedures.
A Cochrane systematic review examining VR simulation training found that simulation likely provides trainees with benefits in independent procedure completion compared to no training. These findings support using simulation not only for training but for standardized competency assessment.
VR endoscopy simulators capture performance data automatically. All trainees facing assessment encounter identical scenarios. Pre-defined criteria eliminate inter-rater variability. Results provide specific , actionable feedback rather than general impressions.
Continuing Education
Simulation serves practicing endoscopists as well as trainees. When new techniques emerge or new devices become available , experienced physicians use simulators to develop proficiency before clinical adoption.
Continuing medical education increasingly incorporates hands-on simulation. Physicians attending conferences or training courses practice techniques on simulators before returning to their practices. This approach accelerates adoption of advances while maintaining patient safety.
Benefits of Endoscopy Simulator Training
The advantages of simulation extend to trainees , educators , institutions and patients.
For Trainees
Learners benefit from low-stakes practice environments where mistakes become learning opportunities rather than patient harms. They can repeat challenging scenarios until mastery develops. They receive objective feedback identifying specific areas for improvement. And they build confidence before facing the pressures of real patient care.
Simulation also accommodates different learning paces. Some trainees need more practice than others to achieve competence. Simulators provide unlimited repetition without the scheduling constraints , patient availability issues or supervision requirements of clinical training.
For Educators
Faculty benefit from structured teaching environments where they can focus entirely on the learner. Clinical teaching often involves balancing educational goals against procedure completion , time pressures and patient comfort. Simulation removes those competing demands.
Educators can also standardize curricula across trainees. Every learner encounters the same foundational scenarios , receives consistent instruction and meets identical competency benchmarks. This standardization improves program quality and outcomes assessment.
For Institutions
Training programs benefit from improved efficiency. Simulation-prepared trainees require less intensive supervision and progress faster through clinical training. Procedure times during supervised cases decrease. Complication rates during the learning curve diminish.
Programs also gain assessment tools that support accreditation requirements and competency documentation. Objective simulation performance data supplements traditional evaluations and provides evidence of training effectiveness.
For Patients
Ultimately , patients benefit most. Endoscopists trained with simulation cause less discomfort , achieve better outcomes and handle complications more effectively than those trained through traditional apprenticeship alone. The learning curve that once occurred entirely on patients now happens substantially on simulators.
Endoscopy Simulators Across Specialties
While gastrointestinal applications dominate discussion , endoscopy simulator principles extend across specialties using endoscopic techniques.
Bronchoscopy training faces similar challenges to GI training. Our bronchoscopy simulator options include the standard bronchoscopy simulator for basic airway navigation , intermediate configurations for diagnostic procedures and advanced systems supporting therapeutic techniques. For combined endoscopic and ultrasound training , our ultrasound bronchoscopy simulator addresses EBUS-specific skills.
Urological endoscopy including cystoscopy and ureteroscopy benefits from dedicated training platforms. Our urological endoscopy simulator addresses the anatomical and technical requirements specific to urinary tract procedures.
Gynecological applications also utilize simulation. Our hysteroscopy simulator provides training for diagnostic and operative hysteroscopy procedures.
Related minimally invasive techniques share many training principles with endoscopy. Our laparoscopy simulator develops hand-eye coordination and instrument manipulation skills applicable across surgical specialties.
Selecting the Right Endoscopy Simulator
Programs evaluating simulator options should consider several factors.
Training objectives should drive selection. What specific skills must the simulator develop? Basic scope manipulation requires different equipment than advanced therapeutic technique training. Programs should map simulator capabilities to curricular needs.
Trainee population matters. A fellowship program with few trainees has different needs than a large residency program or continuing education center. Usage volume affects maintenance requirements and total cost of ownership.
Available resources constrain choices. Budget limitations require prioritization. Space requirements vary between simulator types. Technical support needs differ between simple mechanical models and complex computer systems.
Faculty expertise affects outcomes. Simulators alone don't create effective training. Faculty must understand how to structure practice , provide feedback and assess performance. Programs should plan faculty development alongside equipment acquisition.
Our Endoscopy Simulation Solutions
At Suzhou Frank Medical , we provide comprehensive endoscopy simulator options for training programs across specialties and skill levels. Our product range addresses needs from foundational skill development through advanced therapeutic technique acquisition.
We understand that different programs have different requirements. A new fellowship building simulation capacity from scratch faces different decisions than an established program adding specific capabilities. Our team works with programs to identify solutions matching their trainee populations , curricular objectives and available resources.
Explore our complete range of endoscopic intervention training models to find simulators matching your program's specific needs. Whether you're establishing initial simulation capability or expanding existing resources , we offer options at various price points and complexity levels.
Have questions about which simulators best fit your training objectives? Contact us to discuss your program's needs and explore solutions.
Conclusion
An endoscopy simulator transforms how trainees develop procedural competence. By shifting foundational learning away from patients , simulation improves safety , accelerates skill acquisition and enables objective competency assessment. The evidence supporting simulation continues growing as more programs integrate these tools into structured curricula.
The question for training programs is no longer whether to use endoscopy simulators but how to use them most effectively. Thoughtful selection , intentional curriculum integration and faculty development maximize simulation's educational potential. The result benefits everyone: trainees who learn more efficiently , educators who teach more effectively and patients who receive care from better-prepared endoscopists.
© 2025. All rights reserved.
About Us
Introduction
Development
Cooperation
Service
Main Products
Medical Grade Monitor
No 15, Jinyang road KunshanSuzhou, Jiangsu, China
