📞Customer Service: +86 13248368268 📧servicecenter@suzhoufrank.com one year replacement and warranty!
Biopsy Training on Simulators: Building Confidence and Accuracy
Biopsy training on simulators builds the forceps control, jaw technique, and positioning accuracy needed to minimize sampling errors before trainees perform biopsies on real patients.
MEDICAL TRAINING
Dr Qi Rui
3/26/20267 min read
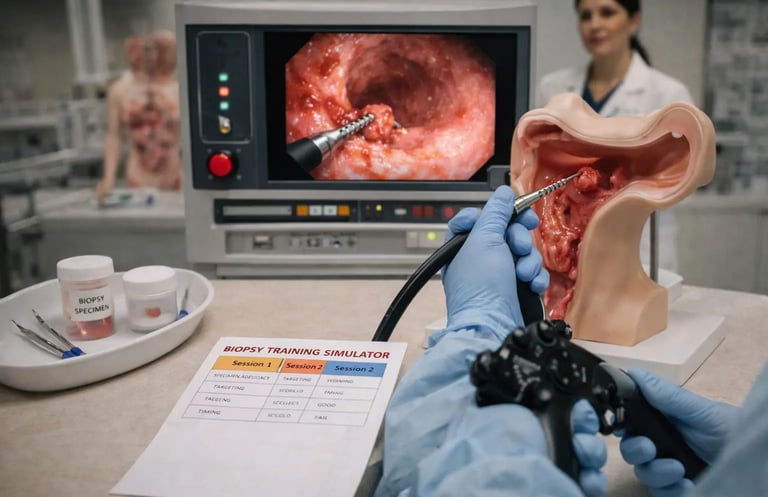
Endoscopic biopsy is a skill that sits at the intersection of technical precision and clinical judgment. The procedure may look simple on paper, open forceps, touch tissue, close forceps, but in practice, obtaining consistently adequate, well-positioned samples requires a level of coordinated instrument control that takes real, structured practice to develop. For trainees entering gastroenterology or GI surgery, biopsy accuracy is not a skill that can be taken for granted. It must be built deliberately, ideally in a simulation environment before the stakes involve real patients.
This article focuses specifically on biopsy training in simulation settings: the goals of training, the technical challenges simulation addresses, the types of simulators and models used, and the evidence that supports this approach.
The Challenge of Teaching Biopsy
Biopsy seems deceptively simple when watched, the supervising endoscopist positions the scope, passes the forceps, samples the tissue, and moves on. What trainees do not see until they try it themselves is how much invisible coordination underlies each step. Scope tip position must be maintained while simultaneously operating the accessory channel. Forceps jaws must be fully open before mucosal contact. Jaw closure timing must coincide with stable scope position. Specimen retrieval must be smooth to prevent fragmentation.
When trainees attempt biopsy for the first time on real patients, these demands compete for limited cognitive bandwidth. The result is often an inconsistent biopsy: tangential samples, superficial tissue bites, poorly located specimens, or inappropriate force that causes mucosal trauma. These errors are difficult to correct in real time during a clinical procedure because supervisor intervention disrupts workflow and may increase patient discomfort.
Simulation solves this problem by creating a dedicated practice environment where trainees can focus on each component of the biopsy sequence without clinical time pressure or patient welfare concerns.
Core Competencies Developed in Biopsy Simulation Training
1. Scope Tip Positioning for Biopsy
The most important determinant of biopsy quality is endoscope position. Simulation training specifically targets the skill of repositioning the scope tip to achieve an en face view of a target lesion before sampling. This requires:
Recognizing when the current scope position is suboptimal for biopsy
Using tip deflection and torque to adjust the viewing angle
Understanding how scope position in the stomach, esophagus, or colon affects forceps trajectory
Physical training models allow trainees to practice this positioning repeatedly for different anatomical locations: the posterior gastric body, the gastric fundus on retroflexion, flat lesions in the sigmoid colon, and subtle mucosal changes at the ileocecal valve. Each location presents different geometric challenges that require different positioning adjustments.
2. Forceps Deployment and Jaw Control
Passing biopsy forceps through a curved endoscope and deploying them accurately onto a target requires practice. The forceps must:
Travel through the accessory channel without snagging
Deploy fully at the scope tip with jaws in the correct orientation
Open completely before mucosal contact
Close with appropriate timing and force to capture an adequate tissue core
Simulation training allows trainees to practice this sequence until it becomes automatic. When jaw deployment and control are practiced to the point of procedural automaticity, trainees can allocate cognitive resources to target selection and sample quality assessment rather than instrument mechanics.
3. Force Control and Tissue Contact
Applying appropriate force during biopsy is a calibrated skill. Too little force results in a superficial sample or no sample at all; too much force causes mucosal trauma, hemorrhage, and occasionally perforation. The correct force is just enough to ensure full jaw engagement with the mucosal surface before closure.
Physical simulation models provide the tactile resistance feedback necessary to calibrate this force. Trainees can feel the difference between inadequate contact, appropriate contact, and excessive pressure through the instrument handle, a form of learning that is difficult to achieve on VR simulators with limited haptic fidelity and impossible to teach verbally.
4. Sample Target Accuracy
In clinical endoscopy, many biopsy indications require sampling from a specific location, the edge of an ulcer, the center of a polypoid lesion, or a defined segment of Barrett's mucosa at precise intervals. Hitting these targets accurately while maintaining scope stability is a spatial skill that benefits directly from targeted practice.
Simulation training can create specific target scenarios: small dots or marked areas on a training model surface that trainees must hit accurately with biopsy forceps. This gamification of targeting practice has been shown to improve precision in clinical biopsy performance.
Types of Simulators Used in Biopsy Training
Physical Tissue Analog Models
Physical models using silicone, gel, or latex surfaces that mimic mucosal tissue properties are the most commonly used platform for biopsy technique training. These models:
Accept real biopsy forceps through standard accessory channels
Provide tactile resistance similar to mucosal tissue
Allow visual confirmation of sample location and size
Support repeated use across many training sessions
The GI Endoscopy Simulator from SuzhouFrank is a physical training platform that supports biopsy technique practice in a realistic anatomical context. Its tissue-mimicking surface properties and compatible accessory channel allow trainees to practice the complete biopsy sequence, scope positioning, forceps deployment, jaw control, and specimen retrieval, using real instruments.
Advanced ESD and Procedure Models
For advanced biopsy training, including large-forceps sampling, submucosal lesion targeting, or biopsy under challenging access conditions, more specialized simulation platforms are available. The GI ESD Surgical Simulator provides a training environment for advanced endoscopic tissue manipulation, including precise sampling and tissue handling techniques relevant to both biopsy and resection procedures.
Virtual Reality Simulators with Biopsy Modules
Some VR endoscopy simulators include biopsy modules that allow trainees to practice sample location selection and lesion targeting in a computer-generated environment. While the haptic feedback for forceps-tissue interaction remains limited compared to physical models, VR biopsy modules have value for:
Practicing sampling protocol compliance (e.g., Sydney Protocol, Barrett's surveillance intervals)
Training target recognition and sample location decision-making
Generating performance metrics (number of samples, deviation from protocol)
The combination of physical model practice for technical execution and VR training for protocol compliance creates a comprehensive biopsy training package.
Structured Biopsy Training Programs
A well-designed biopsy training program is not simply a block of unstructured simulator time. It is a structured curriculum with defined learning objectives, milestones, and feedback mechanisms.
Sample Training Progression
Session 1: Instrument Orientation Trainee learns to pass, deploy, and retrieve biopsy forceps through the accessory channel on a bench model. Focus is on jaw mechanics, not tissue interaction.
Session 2: Flat Surface Targeting Trainee practices achieving en face scope position and accurately placing open forceps on marked targets on a flat tissue analog surface. Multiple repetitions per target location.
Session 3: Curved Surface Targeting Trainee practices biopsy on curved surfaces replicating gastric folds, colonic haustrae, and angulated segments. Scope repositioning for optimal position is emphasized.
Session 4: Protocol-Based Sampling Trainee practices multi-site sampling protocols (e.g., five-site gastric mapping, four-quadrant esophageal sampling) on an anatomical model, ensuring correct locations and sample labeling.
Session 5: Challenging Access Scenarios Trainee practices biopsy of targets in anatomically difficult positions: posterior gastric wall on retroflexion, flat lesions in acute-angle segments, friable tissue requiring modified technique.
Feedback and Assessment
After each session, feedback should address:
Accuracy of target selection
Sample adequacy (assessed visually from retrieved tissue size)
Scope positioning technique
Protocol compliance
Time efficiency
For a comprehensive framework covering how assessment is integrated into endoscopy simulation training, see Skills Assessment in Simulation, which reviews the major assessment tools and their application to procedural skills including biopsy.
Transfer of Biopsy Skills from Simulation to Clinical Practice
The key question in any simulation training program is whether skills practiced on a simulator actually transfer to clinical performance. For biopsy, the evidence is encouraging.
Studies published on PubMed demonstrate that simulation-based training for endoscopic procedural skills, including accessory channel techniques, produces measurable improvements in early clinical performance. Trainees who complete structured simulator biopsy training before their first supervised patient cases achieve higher rates of sample adequacy and lower rates of technical errors compared to controls.
The mechanism of transfer is primarily through procedural automaticity, trainees who have practiced the biopsy sequence to the point of automatic execution can direct their full clinical attention to target selection, patient safety, and protocol compliance rather than instrument mechanics. This is the fundamental value of simulation in procedural medicine.
For a broader perspective on how simulation-based training frameworks support the development of clinical endoscopy competencies, see Clinical Simulation in Endoscopy, which discusses the theoretical and practical foundations of endoscopy simulation education.
Minimizing Sampling Errors Through Simulation Practice
Sampling errors, taking biopsies from the wrong location, with inadequate depth, or in insufficient number, are a significant quality problem in clinical endoscopy. While some errors reflect clinical judgment issues, many reflect technical limitations in biopsy execution that simulation training can directly address.
Common Sampling Errors Addressable Through Simulation
Tangential samples occur when the scope is poorly positioned and the forceps approach the tissue at an angle rather than head-on. Superficial samples result from incomplete jaw opening or insufficient mucosal contact. Sampling from the wrong location is a protocol compliance issue that simulation can directly reinforce through structured exercises. Fragmented samples often result from rough forceps withdrawal, a technique error that smooth retrieval practice on simulators corrects quickly. And missing the intended target entirely, particularly on curved mucosal surfaces, is addressed through dedicated curved-surface targeting drills on bench models.
Systematically practicing each of these error scenarios in a simulation environment, and receiving immediate feedback on performance, creates trainees who enter clinical practice with a biopsy technique that is both technically sound and procedurally reliable.
The World Health Organization and Procedural Competency
The global context for biopsy training quality extends beyond individual trainees. The World Health Organization has emphasized that diagnostic accuracy in procedural medicine depends critically on operator competence. Inadequate biopsy technique contributes to missed diagnoses, delayed cancer detection, and unnecessary repeat procedures, all of which impose patient harm and healthcare resource burden.
Structured simulation-based biopsy training is a practical mechanism for improving diagnostic quality at a population level, particularly as endoscopy services expand in lower-resource settings. For the WHO's framework on procedural quality and patient safety, see WHO: Patient Safety.
SuzhouFrank: Simulation Equipment for Biopsy and Procedural Training
SuzhouFrank provides high-quality physical simulation models designed to support the full spectrum of endoscopic procedure training, including biopsy technique development. Our products are engineered for anatomical accuracy, tissue realism, and durability across intensive training use.
Browse our complete catalogue of endoscopic training models at https://www.suzhoufrank.com/all-products#endoscopic-intervention-training-model. For tailored program support, product demonstrations, or institutional purchasing inquiries, visit https://www.suzhoufrank.com/contact-us.
Conclusion
Biopsy training in simulation is not a luxury, it is a quality investment. The technical demands of accurate, protocol-compliant endoscopic biopsy are real, and the consequences of inadequate training are measured in missed diagnoses and patient harm. Structured simulation programs that specifically address scope positioning, forceps control, force calibration, and target accuracy give trainees the procedural foundation they need to perform consistently high-quality biopsies from their earliest supervised cases. With the right simulation tools and curriculum design, biopsy competence can be built efficiently, measured objectively, and transferred reliably to clinical practice.
References:
© 2025. All rights reserved.
About Us
Introduction
Development
Cooperation
Service
Main Products
Medical Grade Monitor
No 15, Jinyang road KunshanSuzhou, Jiangsu, China
