📞Customer Service: +86 13248368268 📧servicecenter@suzhoufrank.com one year replacement and warranty!
Colonoscopy Models: When Physical Models Still Matter
When does a physical colonoscopy model outperform a virtual simulator? This guide explains the strengths of bench-top models and how they complement software-based training in GI programs.
MEDICAL TRAINING
Dr Qi Rui
3/24/20267 min read
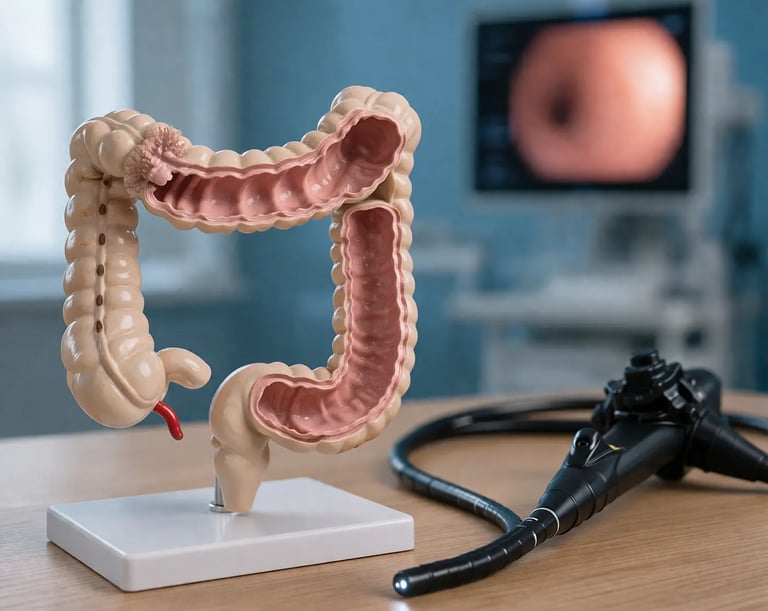
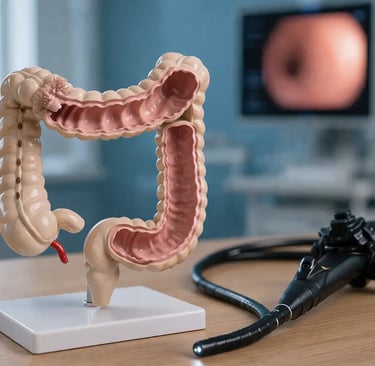
In an era of sophisticated virtual reality simulators and computer-generated anatomy, it might seem like physical colonoscopy models would be obsolete. They are not. Physical training models remain an essential component of any serious colonoscopy training program, offering distinct advantages that digital platforms cannot replicate. Understanding what physical models do well, and where they fit in a broader simulation curriculum, helps program directors design training that is both effective and cost-efficient.
This article explains what colonoscopy physical models are, how they work, the specific skills they develop best, and how they complement virtual simulators in a comprehensive training environment.
What Is a Colonoscopy Physical Model?
A colonoscopy physical model is an anatomically shaped, tactile replica of the human colon. These models are typically constructed from silicone, latex, or similar materials that approximate the texture and resistance of real intestinal tissue. They are designed to be used with actual colonoscopes and accessories, giving trainees genuine hands-on experience with the instruments they will use in clinical practice.
Physical models range from simple segment models (representing a portion of the colon for practicing a specific skill) to full-length colonic models that replicate the entire path from rectum to cecum, including anatomical landmarks like the splenic flexure, hepatic flexure, and ileocecal valve. Some models are mounted in transparent housings so that trainers can observe scope position during practice, while others are enclosed in more realistic external casings.
Unlike virtual reality simulators, physical models do not require computers, software, or calibration. They can be set up in any room, used at any time, and maintained with minimal technical support. This simplicity makes them accessible to a wide range of institutions and training environments, including resource-limited settings where VR infrastructure may not be feasible.
The Unique Value of Physical Tactile Feedback
The central argument for physical colonoscopy models is tactile, or haptic, feedback. When a trainee pushes, torques, or withdraws a colonoscope through a physical model, the instrument responds in ways that a physical body would: resistance increases at angulations, looping generates characteristic counter-pressure, and the tip deflection translates into actual movement that can be felt in the hands.
This tactile experience is qualitatively different from what even the best VR simulators currently provide. Haptic technology in VR platforms has improved significantly, but it remains an approximation of real tissue interaction rather than a direct physical analog. For skills where force application and instrument feel are critical, such as navigating a tight sigmoid angulation or reducing a transverse loop, physical models provide training that more closely resembles the actual procedure.
Force Calibration and Pressure Awareness
One of the most common errors made by novice colonoscopists is applying excessive force to advance the scope. In patients, this causes pain, loop formation, and in rare cases, perforation. Physical models give trainees immediate feedback when they are pushing too hard: the model resists, the scope transmits counter-force to the hands, and the trainer can observe scope looping or model deformation.
This real-time physical feedback is difficult to replicate digitally. Training a trainee's hands to sense inappropriate force requires physical resistance, something that physical models provide naturally and reliably across thousands of training repetitions.
Skills Best Developed on Physical Models
Not all colonoscopy skills are equally well-served by physical versus virtual simulation. Physical models excel at developing specific competencies.
Instrument Handling and Coordination
Colonoscopy requires coordinated use of both hands: the right hand controls scope advancement, withdrawal, and torque, while the left hand manages the control dials for tip deflection and accessory channel operations. This bimanual coordination must be learned with a real instrument in hand. Physical models are the ideal environment for this foundational skill.
Loop Recognition and Management
Loops are a central challenge of colonoscopy, particularly in the sigmoid colon and transverse colon. Physical models that replicate sigmoid redundancy allow trainees to feel how a loop forms during overzealous advancement and to practice the alpha loop reduction maneuver, a technique that requires both scope withdrawal and counter-clockwise torque applied simultaneously. The physical feel of loop reduction is difficult to adequately simulate in VR.
Insertion and Navigation Technique
The basic mechanics of advancing the colonoscope through the colon, using air/water sparingly, cleaning folds to maintain visualization, and using position changes to straighten the colon, are skills that benefit from repeated physical practice. Physical models allow this practice to occur without time constraints, supervisor availability requirements, or patient welfare considerations.
Accessory Channel Skills
Physical models support practice of accessory instrument use: biopsy forceps deployment, snare positioning for polypectomy, and clip application for hemostasis. These skills require the trainee to manipulate real instruments through a real channel, developing the hand-eye coordination needed for clinical procedures. This is an area where physical models hold a clear advantage over VR systems, which typically offer limited simulation of accessory channel instrument interaction.
Physical Models vs. Virtual Reality Simulators: A Complementary Relationship
Physical models and VR simulators are not competitors, they address different learning needs within the same training program. The most effective colonoscopy training programs use both, assigning each to the tasks it does best.
Physical models excel at instrument familiarization and loop management because both skills depend on real tactile feedback that software cannot fully replicate. Accessory channel skills, including biopsy, polypectomy snare work, and clip placement, also transfer better from hands-on model practice than from virtual platforms. On the other side, VR simulators are stronger for systematic mucosal inspection, pathology recognition, and performance metric tracking, all areas where visual detail and objective scoring matter more than physical feel. Physical models also carry a much lower cost per session, since they require no software licenses or maintenance contracts, making them an accessible foundation for programs at any budget level.
For a comprehensive understanding of how VR simulators compare to physical models across GI endoscopy training, see GI Simulators for Training, which reviews the major simulator categories and their practical applications.
Physical Models in Demonstration and Teaching
Physical models serve an important role not just for trainee practice but also for teaching and demonstration. When an instructor needs to show a trainee why a loop forms in the sigmoid, or how counter-clockwise torque straightens the transverse colon, a transparent-housing physical model provides a visual and tactile teaching tool that a VR screen cannot match.
This demonstration function is particularly valuable in group settings, workshops, training days, or orientation sessions, where multiple trainees can observe the same maneuver before attempting it themselves. The visible scope position within the model makes abstract anatomical concepts concrete and immediately understandable.
Use in Procedural Workshops
Colonoscopy skills workshops often use physical models as the primary hands-on platform precisely because they are portable, require no technical setup, and can be used simultaneously by multiple trainees. A workshop with ten physical models and ten colonoscopes allows a cohort of trainees to practice simultaneously, maximizing hands-on time per trainee in a single session.
Colonoscopy Models in Resource-Limited Settings
In many parts of the world, sophisticated VR simulator platforms are simply not feasible due to cost, technical infrastructure requirements, or maintenance challenges. In these settings, high-quality physical models offer a practical alternative for building procedural competence before clinical practice.
The World Health Organization has consistently emphasized that expanding access to safe surgical and endoscopic procedures is a global health priority. Training infrastructure that is affordable, portable, and maintainable without specialized technical support plays an important role in achieving this goal. For the WHO's framework on safe procedural practice, see WHO: Patient Safety.
Physical colonoscopy models can be deployed in settings where VR simulators cannot, extending the benefits of structured simulation training to trainees in lower-resource healthcare systems.
Evaluating Physical Colonoscopy Models: What to Look For
Not all physical colonoscopy models are equal. When selecting a model for a training program, several factors should be considered.
Anatomical Accuracy
The model should replicate the natural curves, flexures, and diameters of the human colon accurately. Models that over-simplify the anatomy do not prepare trainees for the variability they will encounter in real patients.
Material and Tactile Realism
The model surface should provide realistic resistance without being so stiff that it distorts technique or so soft that it gives unrealistic force feedback. High-quality silicone or latex materials that closely mimic tissue properties are preferable.
Durability
Physical models are subjected to repeated scope insertions and forceful maneuvers. Materials and construction quality must support thousands of training sessions without deterioration that compromises the training experience.
Compatibility with Standard Instruments
Models must accommodate the standard colonoscope diameters and lengths used in clinical practice. Compatibility with accessories (biopsy forceps, snares, clips) is essential for programs that include therapeutic skill training.
Transparency Option
Models with transparent or semi-transparent outer casings allow trainers to observe scope position and loop formation, greatly enhancing the teaching and feedback value of the model.
For a review of the specific features that distinguish high-quality colonoscopy simulation products, see Colonoscopy Simulators Features, which covers key design criteria in detail.
Research on Physical Models in Colonoscopy Training
The evidence for physical model-based colonoscopy training aligns with the broader evidence base for simulation in endoscopy education. Studies published on PubMed have demonstrated that hands-on simulation training, whether physical or virtual, improves early clinical performance compared to unaugmented apprenticeship training.
Specifically, physical model training has been shown to be effective for developing insertion technique, loop management skills, and instrument familiarity in novice colonoscopists. These foundational skills translate directly to improved performance during initial supervised patient cases.
SuzhouFrank: High-Quality Colonoscopy Physical Models
SuzhouFrank manufactures a comprehensive range of medical simulation equipment for endoscopy training, including high-quality physical colonoscopy models designed for realistic, durable practice. Our models are built to clinical anatomical standards, using materials that provide authentic tactile feedback for insertion, navigation, and accessory skill training.
Our training equipment is used by medical schools, hospital endoscopy programs, and gastroenterology training centers globally. To browse our full product range, visit https://www.suzhoufrank.com/all-products#endoscopic-intervention-training-model. For pricing, customization inquiries, or to request a demonstration, contact us at https://www.suzhoufrank.com/contact-us.
Conclusion
Physical colonoscopy models remain a vital component of modern endoscopy training. Their tactile realism, accessibility, low cost per session, and suitability for group teaching make them irreplaceable in specific training contexts, particularly for instrument familiarization, loop management, and accessory channel skill development. When used in combination with VR simulators and supervised clinical practice, physical models contribute to a training curriculum that is comprehensive, efficient, and evidence-based. The question is not whether to include physical models in colonoscopy training programs, but how to deploy them most effectively alongside the other tools available.
References:
© 2025. All rights reserved.
About Us
Introduction
Development
Cooperation
Service
Main Products
Medical Grade Monitor
No 15, Jinyang road KunshanSuzhou, Jiangsu, China
