📞Customer Service: +86 13248368268 📧servicecenter@suzhoufrank.com one year replacement and warranty!
What Diseases Can Endoscopy Detect?
Discover what diseases can be detected by an endoscopy (EGD, Colonoscopy). Visualization + biopsy confirms everything from GERD to cancer with definitive accuracy.
ENDOSCOPY
Dr Qi Rui
12/16/20258 min read
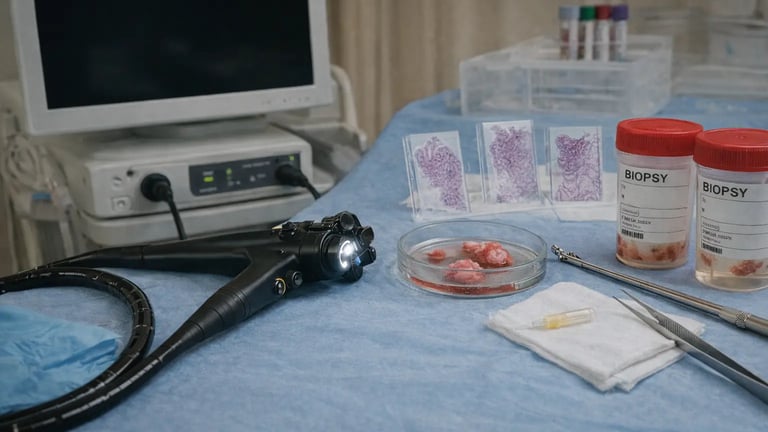
Endoscopy serves as one of the most reliable diagnostic tools in gastroenterology. It lets physicians see inside your digestive tract directly - something imaging tests like CT scans and X-rays simply can't match. But what exactly can this procedure find?
The short answer: quite a lot. Endoscopy can detect conditions ranging from acid reflux damage to cancer. It identifies inflammation, ulcers, polyps, strictures and structural abnormalities. And when combined with biopsy, it provides definitive diagnoses that would otherwise require surgery to obtain.
If you're unfamiliar with the basics, our guide on what is endoscopy covers how the procedure works and why physicians recommend it. This article focuses specifically on the diseases and conditions endoscopy can identify.
How Endoscopy Detects Disease
Before diving into specific conditions, it helps to understand how endoscopy actually finds problems.
The endoscope contains a high-definition camera that transmits real-time images to a monitor. As the physician guides the scope through your digestive tract, they're looking at the mucosal lining in remarkable detail. Modern equipment can detect abnormalities as small as a few millimeters.
But visualization is only part of the story.
Endoscopy also allows tissue sampling. If the physician spots something suspicious - or even something that looks normal but warrants closer examination - they can take a biopsy on the spot. This tissue goes to a pathology lab where it's examined under a microscope for cellular abnormalities.
This combination of direct visualization plus histopathological analysis is what makes endoscopy so powerful. You get both the "what does it look like" and the "what is it actually" answers in one procedure.
The National Institute of Diabetes and Digestive and Kidney Diseases notes that endoscopy can identify diseases and health conditions including gastroesophageal reflux disease, celiac disease, Barrett's esophagus and cancer - among many others.
Conditions of the Esophagus
The esophagus is the first structure examined during upper endoscopy. Several conditions affecting this organ are readily detected.
Gastroesophageal Reflux Disease (GERD)
GERD occurs when stomach acid repeatedly flows back into the esophagus. Over time, this acid exposure damages the esophageal lining. Endoscopy reveals the telltale signs - redness, erosions, ulcerations and inflammation of the lower esophagus.
Not everyone with GERD has visible damage. Some patients have symptoms without obvious mucosal changes. But when damage is present, endoscopy identifies it clearly. This helps physicians determine disease severity and guide treatment decisions.
Barrett's Esophagus
This condition develops as a complication of chronic GERD. The normal squamous cells lining the lower esophagus get replaced by columnar cells - a change called intestinal metaplasia. Barrett's esophagus significantly increases the risk of esophageal adenocarcinoma.
Endoscopy is the only way to diagnose Barrett's. The abnormal tissue often has a distinct salmon-pink appearance that differs from normal esophageal lining. But visual inspection alone isn't enough. Biopsies are essential to confirm the diagnosis and check for dysplasia (precancerous changes).
According to the Cleveland Clinic, patients with Barrett's esophagus require regular surveillance endoscopies to monitor for progression to cancer.
Esophageal Strictures
Strictures are narrowed sections of the esophagus that make swallowing difficult. They often result from chronic acid reflux, but can also develop after radiation therapy, caustic injury or certain medications.
Endoscopy both diagnoses and treats strictures. The physician can visualize the narrowing directly and often dilate it during the same procedure using a balloon or graduated dilators.
Eosinophilic Esophagitis (EoE)
EoE is an allergic inflammatory condition affecting the esophagus. It causes difficulty swallowing, food impaction and heartburn. The condition has become increasingly recognized over the past two decades.
During endoscopy, EoE often presents with characteristic findings - rings, furrows, white plaques and narrowing. But these visual features aren't always present. Biopsy is required to confirm the diagnosis by identifying elevated eosinophil counts in the esophageal tissue.
Esophageal Cancer
Endoscopy detects esophageal malignancies including adenocarcinoma and squamous cell carcinoma. Suspicious findings include masses, ulcerated lesions, irregular mucosa and strictures that don't have a benign explanation.
When cancer is suspected, multiple biopsies are taken for histological confirmation and staging purposes.
Conditions of the Stomach
Moving beyond the esophagus, endoscopy examines the entire stomach lining.
Peptic Ulcers
Gastric ulcers are breaks in the stomach lining. They cause pain, nausea, bloating and sometimes bleeding. The two main causes are Helicobacter pylori infection and overuse of nonsteroidal anti-inflammatory drugs (NSAIDs).
Endoscopy visualizes ulcers directly. The physician can assess size, depth, location and whether active bleeding is present. Biopsies are typically taken to test for H. pylori and rule out malignancy - gastric ulcers can occasionally represent cancer.
Gastritis
Gastritis refers to inflammation of the stomach lining. It has many causes - H. pylori infection, alcohol, bile reflux, autoimmune conditions and certain medications. Symptoms include upper abdominal pain, nausea and vomiting.
Endoscopy reveals the inflammatory changes - redness, swelling, erosions. Biopsies help identify the specific cause and rule out more serious pathology.
Gastric Polyps
Polyps are growths projecting from the stomach lining. Most are benign, but some types carry malignant potential. Endoscopy identifies polyps, and the physician can remove small ones during the procedure for pathological examination.
Gastric Cancer
Stomach cancer often presents late because early stages cause few symptoms. Endoscopy can detect gastric malignancies when they're still treatable. Suspicious findings include ulcerated masses, irregular mucosa and thickened stomach walls.
Multiple biopsies are essential. The American Cancer Society notes that this combination of visualization and tissue sampling makes endoscopy one of the most reliable methods for diagnosing GI cancers.
Hiatal Hernia
A hiatal hernia occurs when part of the stomach pushes up through the diaphragm into the chest cavity. It's often associated with GERD. During endoscopy, the physician can visualize the hernia and assess its size and type.
Conditions of the Duodenum and Small Intestine
The duodenum - the first part of the small intestine - is examined during standard upper endoscopy. Deeper sections of the small bowel require specialized techniques like capsule endoscopy or balloon enteroscopy.
Duodenal Ulcers
Like gastric ulcers, duodenal ulcers are breaks in the mucosal lining. They're actually more common than stomach ulcers. H. pylori infection is the leading cause.
Endoscopy identifies duodenal ulcers and assesses their severity. Active bleeding can be treated during the same procedure.
Celiac Disease
Celiac disease is an autoimmune condition triggered by gluten consumption. It damages the small intestinal lining, causing malabsorption of nutrients. Symptoms include diarrhea, bloating, fatigue and weight loss.
Endoscopy plays a crucial role in diagnosis. The physician looks for characteristic findings like villous atrophy (flattening of the intestinal villi) and scalloping of the duodenal folds. Biopsies confirm the diagnosis by showing the specific pattern of damage and inflammation.
Crohn's Disease
Crohn's is an inflammatory bowel disease that can affect any part of the digestive tract. When it involves the upper GI tract or terminal ileum, endoscopy helps identify areas of inflammation, ulceration and stricturing. Biopsies show the characteristic granulomatous inflammation.
Small Bowel Tumors
Tumors in the small intestine are relatively rare but can be detected through various endoscopic techniques. Capsule endoscopy is particularly useful for surveying the entire small bowel length.
Conditions Detected by Colonoscopy
Colonoscopy - the endoscopic examination of the large intestine - detects its own set of conditions.
Colorectal Polyps
Polyps are the primary target of screening colonoscopy. These growths project from the colon lining and some types (adenomas) can progress to cancer over time. Colonoscopy finds polyps and removes them during the same procedure - this is why the test is so effective at preventing colorectal cancer.
Colorectal Cancer
When cancer has already developed, colonoscopy identifies it. Suspicious masses are biopsied for histological confirmation. The location and extent of disease guide treatment planning.
Inflammatory Bowel Disease
Both Crohn's disease and ulcerative colitis affect the colon. Colonoscopy reveals the pattern and extent of inflammation. In ulcerative colitis, inflammation typically starts at the rectum and extends proximally in a continuous fashion. Crohn's disease often shows patchy, skip lesions.
Biopsies help differentiate between these conditions and assess disease activity.
Diverticulosis and Diverticulitis
Diverticula are small pouches that form in the colon wall. They're extremely common with age. Colonoscopy can identify diverticula, though they're often incidental findings. Active diverticulitis (infection/inflammation of diverticula) is usually diagnosed clinically and with CT scanning rather than colonoscopy.
Angiodysplasia
These are abnormal blood vessels in the colon that can cause chronic bleeding and iron deficiency anemia. Colonoscopy identifies these lesions and can treat them with cauterization.
Beyond the GI Tract: Specialized Endoscopy
Different types of endoscopy examine other body systems.
ERCP for Biliary and Pancreatic Disease
Endoscopic retrograde cholangiopancreatography (ERCP) examines the bile ducts, gallbladder and pancreatic duct. It detects gallstones lodged in the bile duct, strictures, tumors and other abnormalities. ERCP is both diagnostic and therapeutic - stones can be removed during the procedure.
Bronchoscopy for Lung Conditions
Bronchoscopy examines the airways and can detect lung cancer, infections, inflammation and structural abnormalities.
Cystoscopy for Bladder Disease
Cystoscopy examines the bladder and urethra, detecting bladder cancer, stones, infections and structural problems.
The Role of Biopsy in Diagnosis
Visual inspection alone has limitations. Many conditions look similar on camera. And some diseases cause microscopic changes that aren't visible to the naked eye.
That's where biopsy becomes essential.
When the physician takes tissue samples, a pathologist examines them under a microscope. This reveals cellular details that confirm or rule out specific diagnoses. Is that ulcer benign or malignant? Is that inflammation from infection or autoimmune disease? Does that normal-looking tissue actually show early cancer?
Biopsy answers these questions.
For a deeper understanding of how findings are interpreted, our article on what an endoscopy will show explains the different results you might receive.
Why Endoscopy Is Used Alongside Other Tests
Endoscopy is powerful, but it's not always the first test ordered. Physicians often use it alongside other diagnostic methods.
Blood tests can suggest certain conditions - anemia might indicate GI bleeding, elevated liver enzymes might suggest biliary disease, and specific antibodies can point toward celiac disease. But blood tests can't visualize what's happening inside.
Imaging studies like CT scans and MRIs show structural abnormalities and can detect masses. But they can't examine the mucosal surface in detail or obtain tissue samples.
Stool tests can detect blood, infection and inflammation markers. They're useful screening tools but can't provide definitive diagnoses.
Endoscopy fills the gaps. It provides direct visualization plus tissue sampling. When other tests suggest a problem, endoscopy often confirms it. When other tests are inconclusive, endoscopy frequently provides the answer.
What Determines Your Results?
Two patients undergoing identical endoscopy procedures might receive very different results. Several factors influence what gets detected.
Disease presence and stage. Obviously, endoscopy can only find conditions that actually exist. Early-stage diseases may be subtle. Some conditions only cause microscopic changes that require biopsy to identify.
Preparation quality. For colonoscopy especially, bowel preparation dramatically affects visualization. Poor prep means the physician can't see the mucosal surface properly. Lesions get missed.
Physician experience. Higher procedure volumes correlate with better detection rates. Experienced endoscopists recognize subtle abnormalities that less experienced operators might miss.
Equipment quality. High-definition imaging improves detection of small and flat lesions. Modern endoscopes with advanced optics outperform older equipment.
Whether biopsies are taken. Some conditions require histological confirmation. If biopsies aren't obtained from the right locations, diagnoses get missed.
When Normal Results Don't Mean Nothing's Wrong
Here's something important to understand. A normal endoscopy doesn't always mean you're disease-free.
Some conditions don't cause visible changes. Functional disorders like irritable bowel syndrome won't show abnormalities on endoscopy. Early celiac disease might look normal to the naked eye but show changes on biopsy. Microscopic colitis - as the name suggests - requires biopsy to detect.
Additionally, endoscopy only examines certain areas. Standard upper endoscopy doesn't visualize most of the small intestine. Colonoscopy doesn't examine the upper GI tract. If disease exists in areas not examined, it won't be detected.
This is why symptoms sometimes persist despite normal endoscopy results. Further testing or different types of endoscopy might be needed.
The Importance of Quality Equipment in Diagnosis
Detection rates depend partly on imaging technology. The better the visualization, the more abnormalities get identified.
Modern endoscopes produce high-definition images that reveal subtle mucosal changes. Advanced techniques like narrow-band imaging enhance visualization of vascular patterns and surface architecture. These improvements translate directly to better diagnostic accuracy.
Healthcare facilities invest significantly in endoscopy equipment because quality matters for patient outcomes. Superior cameras, adequate lighting and advanced image processing all contribute to catching diseases early - when they're most treatable.
For clinics looking for imaging systems used in diagnostic endoscopy, Suzhou Frank offers a range of medical endoscope camera systems designed for reliable performance and excellent visualization.
© 2025. All rights reserved.
About Us
Introduction
Development
Cooperation
Service
Main Products
Medical Grade Monitor
No 15, Jinyang road KunshanSuzhou, Jiangsu, China
