📞Customer Service: +86 13248368268 📧servicecenter@suzhoufrank.com one year replacement and warranty!
Endoscopy Biopsy Technique: Fundamentals for Trainees
Endoscopy biopsy technique is a foundational skill every GI trainee must develop. Learn the indications, technical steps, and how simulation practice builds accuracy before real patient cases.
MEDICAL TRAINING
Dr Qi Rui
3/25/20266 min read
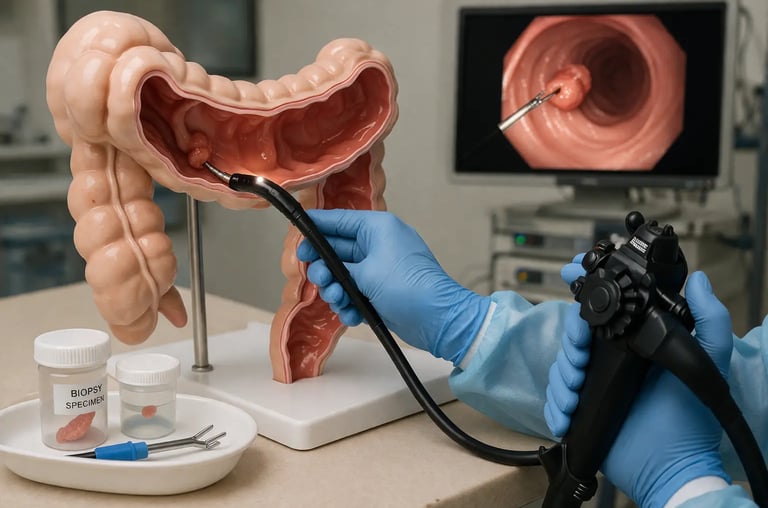
Endoscopic biopsy is one of the most frequently performed accessory procedures in gastrointestinal endoscopy. Whether during a routine upper GI examination, a surveillance colonoscopy, or an investigation of suspicious mucosal lesions, the ability to obtain adequate tissue samples accurately and safely is a fundamental clinical competency. For trainees entering gastroenterology or surgical endoscopy, developing sound biopsy technique early in training establishes a foundation that supports all subsequent therapeutic skill development.
This article introduces the core concepts of endoscopic biopsy technique, explains the anatomical and procedural considerations that influence sampling decisions, and discusses how simulation and physical training models contribute to biopsy skill development before trainees encounter real patients.
Why Endoscopic Biopsy Matters
Histological tissue analysis obtained via endoscopic biopsy is central to the diagnosis and management of a broad range of gastrointestinal conditions. The accuracy of that diagnosis depends not only on the pathologist's interpretation but on the quality and appropriateness of the tissue sample obtained at endoscopy. A technically poor biopsy, too superficial, poorly positioned, or taken from the wrong location, can yield inconclusive results, delay diagnosis, and necessitate repeat procedures.
Common indications for endoscopic biopsy include:
Gastric ulcer, to exclude malignancy and confirm Helicobacter pylori infection
Barrett's esophagus, to detect dysplasia requiring intervention
Colorectal polyps, to characterize histological type and guide management
Suspected Crohn's disease or ulcerative colitis, to establish diagnosis and assess disease extent
Celiac disease, to assess villous architecture in the duodenum
Suspicious mucosal lesions, any appearance suggesting dysplasia, neoplasia, or infection
Each indication carries specific sampling requirements in terms of number of samples, sample location, and depth of tissue acquisition.
Instruments and Equipment
Biopsy Forceps Types
Biopsy forceps are the primary instrument for endoscopic tissue sampling. They are passed through the accessory (working) channel of the endoscope and deployed under direct visualization. Multiple designs exist, each with specific applications:
Standard cup forceps: The most commonly used design, suitable for most mucosal biopsy indications. Available with or without a central spike (to stabilize forceps position before jaw closure).
Jumbo forceps: Larger cup diameter for increased sample size; used when adequate tissue volume is critical, such as in submucosal lesion sampling.
Needle-tipped forceps: Include a central needle to facilitate tissue penetration in fibrotic or firm lesions.
Alligator jaw forceps: Serrated jaws to grip and hold friable tissue; used for hemorrhagic or fragile mucosa.
Familiarity with each forceps type, its deployment mechanics, jaw opening diameter, and appropriate clinical applications, is an essential component of trainee education.
Accessory Channel Management
Before passing biopsy forceps, the endoscopist must ensure the accessory channel port is open and the scope tip is positioned appropriately. Inexperienced trainees often underestimate how much scope tip position and shaft torque affect forceps deployment. When the endoscope is in a curved position, forceps may not deploy fully or may deploy at an unexpected angle. Understanding these mechanics is critical for consistent, accurate biopsy technique.
Core Principles of Biopsy Technique
Optimal Scope Position
The single most important determinant of biopsy accuracy is endoscope position at the moment of sampling. The scope tip should be positioned to achieve:
En face view of the target lesion, Ideally, the mucosa to be sampled is viewed perpendicularly ("face on") rather than tangentially. Tangential biopsy produces superficial, crush-artifact-prone samples that are often inadequate for diagnosis.
Stable position, Respiratory movement, peristalsis, and patient movement can all cause the scope to shift during biopsy. Minimizing scope movement at the moment of forceps closure improves sample quality.
Adequate working distance, The forceps must be visible on screen at the moment of deployment. Working at too short or too long a distance reduces accuracy and risks sampling the wrong area.
Systematic Sampling Protocols
For many biopsy indications, protocols specify the number of samples, their distribution, and any positional requirements. For example:
Gastric biopsy for H. pylori (Sydney Protocol): Samples from the antrum (greater and lesser curvature), the incisura, and the body (greater and lesser curvature), five samples total in separate containers
Barrett's esophagus surveillance: Four-quadrant biopsies every 1–2 cm throughout the Barrett's segment, plus targeted biopsies of any visible lesion
Celiac disease: Minimum four biopsies from the distal duodenum, including the duodenal bulb
Trainees must not only learn how to take a biopsy technically but also understand which protocol applies to a given clinical scenario. This integrates biopsy technique with broader endoscopic decision-making.
Forceps Deployment Mechanics
The biopsy sequence involves several coordinated steps:
Advance the forceps through the accessory channel until the closed jaws are visible at the scope tip
Open the jaws using the thumb ring on the forceps handle
Advance the open forceps onto the mucosal surface with gentle, controlled pressure
Close the jaws firmly by releasing or pushing the thumb ring, while maintaining stable scope position
Withdraw the closed forceps through the channel, retrieving the tissue sample
Remove the tissue from the forceps jaws and place it in the appropriate fixative container
Each step in this sequence has technical requirements that take practice to execute consistently. Closing the jaws too early (before adequate mucosal contact) produces tiny, superficial samples. Failing to maintain scope position during closure produces tangential samples. Rough withdrawal can fragment the specimen.
Common Technical Errors and How to Avoid Them
Tangential Sampling
The most common biopsy error, tangential sampling occurs when the forceps approach the mucosa at an angle rather than perpendicularly. The result is a thin, often inadequate sample containing predominantly surface cells and little lamina propria. Training in optimal scope positioning before biopsy attempts, achievable in a simulation environment, directly reduces this error.
Inadequate Forceps Opening
If the forceps are not fully opened before mucosal contact, the bite size is reduced. Trainees should confirm full jaw opening visually on screen before advancing onto the tissue.
Sample Fragmentation During Retrieval
Hasty withdrawal of forceps through a curved endoscope can shear or fragment the biopsy. Smooth, steady withdrawal, without jerking, preserves sample integrity. This technique requires deliberate practice to develop.
Wrong Container / Cross-Contamination
Biopsy samples from different locations should be placed in separate labeled containers. Organizational errors at this step can result in serious diagnostic errors. Training programs should include explicit instruction on sample handling as part of biopsy training.
The Role of Simulation in Biopsy Training
Learning to perform accurate endoscopic biopsies on real patients during early training is challenging for several reasons: procedure time is limited, supervisors must share their attention across multiple procedure aspects simultaneously, and patient discomfort must be minimized. Simulation addresses these constraints by providing a dedicated environment for biopsy skill development.
Physical Models for Biopsy Training
Physical endoscopy models with simulated mucosal surfaces allow trainees to practice the full biopsy sequence repeatedly: advancing forceps, achieving optimal scope position, opening jaws, making mucosal contact, closing jaws, and withdrawing the specimen. Repeated practice on a physical model builds the hand coordination and procedural memory that translates to better first-case performance.
The GI ESD Surgical Simulator from SuzhouFrank provides a realistic platform for practicing endoscopic tissue sampling techniques including biopsy. Its tissue-mimicking surface properties allow trainees to develop the force control and instrument coordination essential for accurate sampling.
Targeted Biopsy Practice
Simulation allows training programs to create specific scenarios targeting known biopsy challenges, small flat lesions, lesions at acute angulations, lesions in difficult-to-reach locations like the gastric fundus or proximal esophagus. Trainees can practice these challenging scenarios repeatedly without patient exposure, building confidence and accuracy before encountering these situations clinically.
For a broader perspective on how simulation supports procedure training in endoscopy, see Procedure Training with Simulators, which covers the general principles of simulator-based procedural skill development applicable to biopsy and other accessory techniques.
Biopsy in the Context of Broader Endoscopic Training
Biopsy is not an isolated skill, it is embedded in a larger procedural workflow that includes mucosal survey, lesion characterization, therapeutic decision-making, and documentation. Trainees who develop sound biopsy technique early are better positioned to build on this foundation as they progress to more complex therapeutic procedures such as polypectomy, endoscopic mucosal resection, and hemostasis.
The integration of biopsy training into a structured endoscopy curriculum is an important design consideration. For guidance on curriculum design in endoscopy simulation training, see Simulation Curriculum Endoscopy, which outlines the progression from foundational skills to complex procedural competence.
Evidence and Professional Standards
Multiple professional societies have published guidelines on the indications and techniques for endoscopic biopsy. The British Society of Gastroenterology, the American Society for Gastrointestinal Endoscopy, and the European Society of Gastrointestinal Endoscopy all publish evidence-based guidance on biopsy protocols for common clinical scenarios.
Research available on PubMed documents the impact of training quality on biopsy adequacy rates in routine endoscopy practice. Studies have shown that training on simulators before clinical practice improves the consistency of biopsy samples, reducing the rate of inadequate specimens that require repeat procedures.
The World Health Organization's global patient safety initiatives specifically identify procedural competency, including biopsy accuracy, as a key target for quality improvement in gastrointestinal endoscopy services worldwide. For the broader policy framework, see WHO Patient Safety.
SuzhouFrank: Supporting Biopsy Training with High-Quality Simulation Equipment
SuzhouFrank manufactures medical simulation models specifically designed to support endoscopic procedure training, including biopsy technique practice. Our simulation equipment provides realistic tissue surfaces, compatible accessory channel dimensions, and durable construction for high-volume training use.
Explore our full range of endoscopy training equipment in our catalogue at https://www.suzhoufrank.com/all-products#endoscopic-intervention-training-model. For program-specific inquiries or product demonstrations, contact our team at https://www.suzhoufrank.com/contact-us.
Conclusion
Endoscopic biopsy technique is a foundational clinical skill that trainees in gastroenterology and surgical endoscopy must develop systematically. While the procedure appears straightforward, consistent, accurate, and protocol-compliant biopsy requires deliberate practice, feedback, and a thorough understanding of the instruments and anatomical considerations involved. Simulation, through physical models and increasingly sophisticated VR platforms, provides an ideal environment for this early skill development, ensuring that trainees enter their first supervised patient cases with the technical foundation needed to obtain high-quality specimens reliably and safely.
References:
© 2025. All rights reserved.
About Us
Introduction
Development
Cooperation
Service
Main Products
Medical Grade Monitor
No 15, Jinyang road KunshanSuzhou, Jiangsu, China
