📞Customer Service: +86 13248368268 📧servicecenter@suzhoufrank.com one year replacement and warranty!
Gastroscopy Simulators: Training Upper GI Endoscopy Safely
Upper GI endoscopy is a core clinical skill. Gastroscopy simulators give trainees the hands-on repetitions needed to build scope control and procedural confidence before real cases.
MEDICAL TRAINING
Dr Qi Rui
3/20/20268 min read
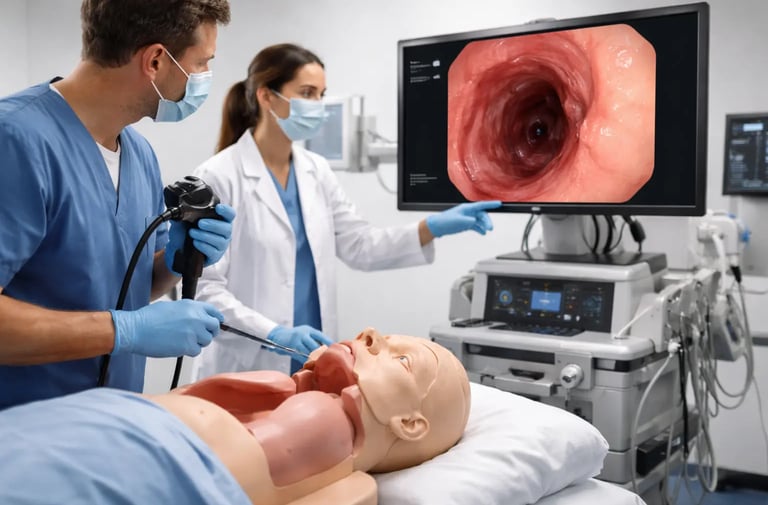
Upper gastrointestinal endoscopy, commonly called gastroscopy or esophagogastroduodenoscopy (EGD), is one of the most frequently performed procedures in gastrointestinal medicine. It provides direct visualization of the esophagus, stomach, and duodenum, and is essential for diagnosing and managing conditions ranging from peptic ulcer disease and Barrett's esophagus to upper GI bleeding and early gastric cancer.
Despite being technically less demanding than colonoscopy in some respects, gastroscopy requires its own set of learned skills. Scope intubation, esophageal navigation, antral and retroflexion views of the stomach, duodenal intubation, and a growing range of therapeutic interventions all take time and repetition to master. A gastroscopy simulator is a training tool purpose-built to accelerate that mastery, providing a safe, realistic environment where trainees can practice upper GI endoscopy without patient exposure.
This article covers what gastroscopy simulators are, how they support training across different stages of skill development, what to look for when selecting one, and how they integrate into a broader upper GI training program.
Why Gastroscopy Training Needs a Dedicated Approach
The assumption that gastroscopy is straightforward because it is shorter than colonoscopy is one of the most persistent misconceptions in GI training. While the procedure is indeed shorter in duration, the skills required are distinct and non-trivial.
Trainees new to upper endoscopy must learn:
Safe intubation: Passing the scope through the cricopharyngeus under direct vision without causing discomfort or injury
Esophageal navigation: Advancing the scope while managing air insufflation and maintaining orientation in a tubular structure
Gastric examination: Systematically examining all regions of the stomach including the fundus, body, incisura, antrum, and pylorus
Retroflexion: A technique that requires rotating the scope tip back on itself to view the fundus and cardia from below, a maneuver that many trainees find counterintuitive at first
Duodenal intubation: Advancing through the pylorus and navigating the acute angulation of the duodenal bulb and second part
Identification of pathology: Recognizing normal anatomical variants and distinguishing them from mucosal disease, vascular changes, or neoplastic lesions
Therapeutic skills: Biopsy, injection, hemostasis, polypectomy, band ligation, and increasingly advanced interventions
Each of these skills has its own learning curve, and each is best first practiced in a simulation environment where the trainee is not managing the concurrent demands of patient care, monitoring, and communication.
Research published through PubMed consistently shows that simulation-based practice before supervised clinical exposure improves early performance on real patients, reducing procedure time, improving technique, and decreasing the frequency of the errors most associated with trainee-level procedures.
What Is a Gastroscopy Simulator?
A gastroscopy simulator is a training device that replicates the anatomy and instrument dynamics of upper GI endoscopy for educational purposes. The key word is "replicates", the simulator does not need to be biologically identical to a human upper GI tract. It needs to be similar enough to develop the relevant skills.
Physical Gastroscopy Simulators
Physical gastroscopy simulators are tangible models of the upper GI anatomy, typically the esophagus, stomach, and duodenum, through which a real flexible endoscope is passed. The scope is connected to its standard video processor, and the trainee sees the same kind of image they would see in a clinical procedure.
The key advantages of physical simulators are:
Real instrument feel: Because a real scope is used, the trainee learns the actual weight, flexibility, and response of the instrument they will use clinically
No software required: No licensing, updates, or technical support needed
Cost-effectiveness: Physical models are substantially less expensive than high-fidelity VR platforms
Compatibility with any scope: Standard endoscopes from any manufacturer can be used
The primary limitation is the inability to dynamically change the case, the anatomy is fixed, and the model cannot simulate physiological responses or a wide range of pathology without modular inserts.
Virtual Reality Gastroscopy Simulators
VR gastroscopy simulators use computer-rendered environments and haptic feedback handles to simulate the procedure without a physical model. The learner holds a controller that replicates the endoscope handle, and the screen displays the virtual endoscopic view.
VR simulators offer:
A large library of cases, including rare pathology
Quantitative performance metrics (time, mucosal coverage, biopsy accuracy)
Dynamic scenarios including simulated complications
Unlimited repeatability without consumable costs
The limitations include higher upfront cost, potential haptic discrepancy from real scope feel, and the requirement for software maintenance.
Hybrid Models
Hybrid simulators combine a physical model for scope handling with a screen-based display for the endoscopic view. This approach gives trainees the benefit of realistic instrument handling while allowing a degree of case variety through the digital display. These platforms are particularly useful for programs that want realistic haptics without the full cost of a high-end VR system.
Key Skills Practiced on Gastroscopy Simulators
Scope Insertion and Esophageal Navigation
The first challenge in gastroscopy is safe, efficient scope insertion. The cricopharyngeus muscle at the top of the esophagus must be passed under direct vision with minimal force, and the esophagus must be navigated without over-insufflation or mucosal contact.
Gastroscopy simulators reproduce the tubular anatomy of the esophagus with realistic resistance at the cricopharyngeal level. Trainees practice insertion technique, air management, and advancement to the gastroesophageal junction before they attempt the maneuver on a patient. The repetition available on a simulator allows trainees to develop the fluid, confident insertion technique that experienced endoscopists make look easy.
Gastric Examination and Systematic Views
A complete gastric examination requires visiting all regions of the stomach in a logical sequence and ensuring adequate mucosal visualization of each area. This sounds simple but requires practice to execute efficiently, particularly for the fundus, which cannot be fully seen without retroflexion, and the lesser curvature and incisura, which require careful wheel adjustments to view completely.
Gastroscopy simulators with realistic stomach anatomy allow trainees to practice systematic examination protocols, developing the habit of checking each region in order so that no area is missed. Studies on adenoma detection rate in colonoscopy have demonstrated that systematic approach and adequate mucosal visualization are directly related to lesion detection. The same principle applies in the upper GI tract: systematic examination technique is learned through repetition, and simulation provides the repetitions.
Retroflexion
Retroflexion, rotating the scope to view the fundus and cardia from below, is one of the first distinctly non-intuitive maneuvers trainees encounter in gastroscopy. It requires up-angling the tip while simultaneously advancing the scope, producing a J-shaped turn that gives a view directly back at the gastroesophageal junction and fundal region.
Trainees who have never performed retroflexion often find it disorienting: the screen image rotates, the usual spatial orientation disappears, and the scope movement responses seem reversed. This disorientation resolves quickly with practice but is best resolved on a simulator rather than during a clinical procedure.
Gastroscopy simulators with a realistic fundal anatomy allow trainees to practice retroflexion, approach, tip deflection, advancement, and rotation, until the maneuver is comfortable and reliable before they attempt it in a patient encounter.
Pyloric Intubation and Duodenal Navigation
Passing the scope through the pylorus and navigating the duodenal bulb and second part requires a different skill set than esophageal or gastric navigation. The pylorus must be approached correctly, the scope tip must be positioned in the center of the pyloric opening, and the advancing movement must be timed appropriately with peristalsis.
The duodenal bulb is small and angular, advancing the scope into the second part requires a specific combination of tip deflection and torque that is not intuitive. Trainees frequently loop the scope or lose position the first many times they attempt duodenal intubation.
Simulators that reproduce the pyloric canal and duodenal anatomy allow trainees to develop the technique for duodenal intubation before their clinical cases. By the time they perform the maneuver on a patient, they have a mental model and a physical memory of the required movements.
Basic Therapeutic Skills
Beyond diagnostic navigation, many training programs introduce basic therapeutic gastroscopy skills through simulation:
Targeted biopsy: Positioning the scope to allow accurate biopsy forceps placement at a defined mucosal target
Injection: Submucosal or intravascular injection technique for hemostasis or EMR preparation
Hemostatic clipping: Deploying clips on a bleeding vessel model
Band ligation: Placing bands on variceal models
Polypectomy: Snare removal of gastric polyps
These skills are introduced progressively, typically after foundational navigation has been established, and they are best practiced on task trainers or modular inserts that specifically target each technique.
Selecting a Gastroscopy Simulator
For program directors choosing a gastroscopy simulator, the relevant selection criteria include:
Anatomical Realism
Does the model accurately reproduce the shape, size, and texture of the esophagus, stomach, and duodenum? Key checkpoints are the cricopharyngeal level, the gastric antrum and retroflexion environment, the pylorus, and the duodenal bulb angulation.
Scope Compatibility
Can the simulator be used with your institution's existing endoscopes? Most physical models are designed to work with standard GI endoscopes. Verify that the model's dimensions and access ports are compatible with your equipment.
Durability and Replaceability
Physical models undergo wear with use. Look for models where high-wear components, tissue inserts, anatomical sleeves, mucosal surfaces, are replaceable at reasonable cost. This determines the long-term economics of the platform.
Expandability for Therapeutic Skills
Does the simulator allow for modular pathology inserts, polyps, ulcers, bleeding sites, that can be added as trainees progress to therapeutic skills? A simulator that supports only navigation practice has a limited training lifespan.
Ease of Setup and Use
Simulators that are difficult to set up or clean will not be used consistently. Look for models with simple setup procedures that can be operated by trainees independently outside of instructor-supervised sessions.
The GI Endoscopy Simulator from SuzhouFrank is designed to address these requirements, providing a physical upper and lower GI training platform compatible with standard flexible endoscopes, with a focus on realistic anatomy and durable construction for regular training use.
Gastroscopy Simulators in a Training Curriculum
Gastroscopy simulation is most effective when it is integrated into a structured training curriculum rather than used ad hoc. The progression should follow the principle of building from foundational to complex:
Stage 1, Orientation: Trainees use the simulator to explore upper GI anatomy, develop scope orientation, and understand the control mechanisms of the endoscope. No procedure is expected, the goal is familiarization.
Stage 2, Navigation competency: Trainees practice complete esophageal navigation, systematic gastric examination, retroflexion, and duodenal intubation until they can complete these consistently and efficiently.
Stage 3, Pathology recognition: Using models with simulated pathology inserts or VR case libraries, trainees practice identifying and classifying mucosal abnormalities, distinguishing erosions from ulcers, polyps from submucosal bulges, and normal variants from disease.
Stage 4, Therapeutic skill introduction: On task trainers for biopsy, injection, clipping, and polypectomy, trainees develop the specific instrument-handling skills needed for therapeutic procedures.
Stage 5, Integration and assessment: Trainees complete full simulated gastroscopy procedures that combine navigation, pathology recognition, and therapeutic decision-making, assessed against defined competency criteria.
This staged approach mirrors the framework discussed in fellowship training advanced endoscopy, where simulation is used to prepare fellows for the increasing complexity of advanced procedures by systematically building on foundational skills.
For programs developing a broader simulation-based GI curriculum, the principles of structured progression and competency-based assessment are explored in medical simulation in endoscopy and GI training, which provides a comprehensive overview of the field.
SuzhouFrank: Gastroscopy and Upper GI Simulation Equipment
SuzhouFrank manufactures physical simulation equipment for upper and lower GI endoscopy training, designed for use in hospital training departments, medical schools, and endoscopy education centers. Their models are built to support the full range of gastroscopy training needs, from basic navigation to advanced therapeutic skill development.
Educators and program directors can explore the full range of available simulation models at https://www.suzhoufrank.com/all-products#endoscopic-intervention-training-model. For product inquiries, institutional pricing, or support with curriculum design, the team is available through the contact page.
Conclusion
Gastroscopy simulators are not a luxury add-on to upper GI training programs, they are a practical necessity for building the specific skills that upper endoscopy demands. Scope insertion, gastric examination, retroflexion, duodenal intubation, and therapeutic maneuvers all require repeated practice to develop, and simulation provides the repetitions needed without patient exposure.
The WHO's endorsement of simulation as a patient safety strategy reflects the broad consensus in the medical education community: simulation-based training, integrated thoughtfully into clinical curricula, produces better-prepared clinicians who are safer and more effective from their earliest patient encounters.
For GI training programs investing in their simulation infrastructure, gastroscopy simulators represent one of the most direct investments in training quality, and, by extension, in the safety and quality of care that trainees will deliver when they practice independently.
© 2025. All rights reserved.
About Us
Introduction
Development
Cooperation
Service
Main Products
Medical Grade Monitor
No 15, Jinyang road KunshanSuzhou, Jiangsu, China
