📞Customer Service: +86 13248368268 📧servicecenter@suzhoufrank.com one year replacement and warranty!
GI Endoscopy: Why Simulation Should Be Part of Training
GI endoscopy carries real risks for inexperienced trainees. Simulation-based practice builds the confidence, speed, and accuracy needed before supervised patient procedures begin.
MEDICAL TRAINING
Dr Qi Rui
3/19/20267 min read
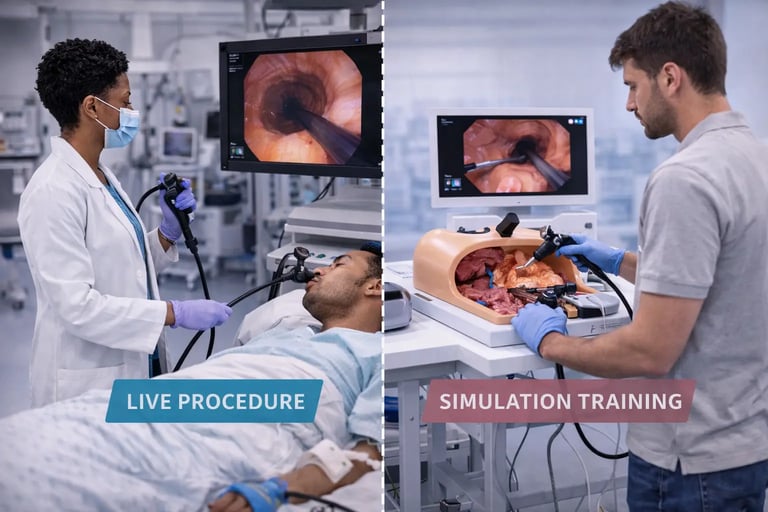
Gastrointestinal endoscopy saves lives. Colonoscopy detects and removes polyps before they become cancer. Upper endoscopy diagnoses ulcers, varices, and early malignancy. Therapeutic procedures like endoscopic submucosal dissection offer patients curative treatment for early GI cancers without open surgery. The clinical value of GI endoscopy is beyond dispute.
But GI endoscopy is also technically demanding, and the consequences of doing it poorly are real. A missed polyp, a perforation, an inadequate retroflexion view, a mismanaged bleed, these outcomes are not hypothetical. They happen, particularly when endoscopists are in the early phases of their training, and their frequency decreases as skill and experience accumulate.
The question for training program directors and clinical educators is: how do we get trainees to a level of competency that is safe for patients as efficiently as possible, and how do we verify that they have reached it? Simulation is a central part of the answer.
What Is GI Endoscopy?
Gastrointestinal endoscopy encompasses a broad family of procedures that use flexible endoscopes to visualize, diagnose, and treat conditions within the digestive tract. The core subdivisions are:
Upper GI endoscopy (esophagogastroduodenoscopy or EGD): A flexible scope is passed through the mouth and advanced through the esophagus, stomach, and duodenum. Used for diagnosis of dyspepsia, reflux disease, peptic ulcer, Barrett's esophagus, and upper GI bleeding, as well as a wide range of therapeutic interventions.
Lower GI endoscopy (colonoscopy): A longer, more flexible scope is passed through the rectum and advanced through the entire colon to the terminal ileum. Used for colorectal cancer screening, polyp detection and removal, investigation of bleeding, and diagnosis of inflammatory bowel disease.
Small bowel endoscopy: Including capsule endoscopy and device-assisted enteroscopy for examination of the small intestine, which is inaccessible by standard upper or lower scopes.
Endoscopic ultrasound (EUS): Combines endoscopy with ultrasound imaging for staging of GI and pancreatobiliary tumors and drainage of fluid collections.
ERCP (endoscopic retrograde cholangiopancreatography): Accesses the biliary and pancreatic ducts for diagnosis and treatment of biliary obstruction, stones, and strictures.
Advanced therapeutic endoscopy: Including EMR, ESD, submucosal tunnel procedures, and endoscopic closure techniques.
Each of these procedures has its own technical requirements, its own learning curve, and its own safety considerations. What they share is the need for training, and simulation has a role in that training across all of them.
The Learning Curve in GI Endoscopy
Medical education research consistently demonstrates that procedural skill in endoscopy follows a learning curve: performance improves with increasing procedural volume, but the rate of improvement varies between individuals and depends heavily on the quality of supervision and feedback provided.
The most studied procedure is colonoscopy. A landmark study published through PubMed found that colonoscopy competency, defined as independent cecal intubation in at least 90% of cases, typically requires between 200 and 300 supervised procedures. However, there is wide individual variation, and some trainees require significantly more exposure to reach this threshold.
Cecal intubation rate is only one metric of colonoscopy quality. Adenoma detection rate, withdrawal time, patient comfort scores, and complication rate all take longer to optimize and require sustained, structured training beyond the basic competency threshold.
For upper endoscopy, the learning curves are generally shorter for basic navigation but become steep again when therapeutic skills are added. ESD, which involves sustained electrosurgical dissection through the submucosal plane, has one of the longest learning curves in endoscopy, with many experts suggesting that true competency requires performing several hundred cases under supervision or in controlled training environments before independent practice begins.
The implication is clear: the number of supervised clinical cases required to reach competency is large, and the early part of the curve, when most errors and complications occur, is precisely the period when simulation can provide the greatest benefit by allowing skill development without patient exposure.
What Simulation Adds to GI Endoscopy Training
Safety During Skill Acquisition
The most direct argument for simulation in GI endoscopy is patient safety. When trainees perform their first scope insertion, their first loop reduction, their first polypectomy, they are going to make mistakes. The question is whether those mistakes happen on a simulator, where no harm results, or on a patient, where the consequences can be significant.
Simulation does not eliminate mistakes in clinical training. What it does is allow trainees to make many of their early mistakes in a safe environment, so that by the time they perform procedures on patients, they have a baseline of technical competency that reduces, though never eliminates, the risk of those early procedural errors.
The World Health Organization's patient safety curriculum explicitly identifies simulation-based training as one of the key strategies for reducing harm during training. For procedural specialties like GI endoscopy, this guidance is directly applicable.
Efficiency of Skill Development
Clinical training time is finite and valuable. Every minute a trainee spends struggling with basic scope navigation is a minute not spent on more advanced skills, and it represents a real cost in terms of patient throughput and faculty supervision time. Simulation allows trainees to build foundational skills before they arrive in the clinical environment, making their supervised clinical time more productive from the start.
A trainee who has completed 40 sessions on an endoscopy simulator and can navigate reliably to the cecum is not the same as a trainee starting their first supervised colonoscopy with no prior practice. The difference in supervision burden, procedure time, and patient comfort is measurable.
Standardized Exposure to Key Skills
In clinical training, the distribution of cases is outside the program's control. A trainee may complete 100 colonoscopies before encountering a difficult sigmoid anatomy, or they may encounter it in their first ten cases. Simulation allows programs to deliberately expose every trainee to defined scenarios, specific anatomical challenges, specific pathology types, specific complications, regardless of what the clinical case mix provides.
This standardization is particularly valuable for rare but important scenarios: a perforation recognized mid-procedure, a major bleeding event requiring emergent hemostasis, an advanced lesion requiring ESD. These are scenarios that a trainee may encounter very rarely in supervised clinical training but needs to be prepared for nonetheless.
Objective Competency Assessment
Simulation provides a platform for objective skill assessment in a way that clinical supervision does not always allow. In the endoscopy suite, assessment of a trainee's performance depends on the attending physician's attention, the complexity of the case, and the time pressure of a clinical environment. On a simulator, every session can be recorded, timed, and scored against defined criteria.
This objective data makes it possible to assess not just whether a trainee performed an adequate procedure, but how their skill is developing over time, and whether they are ready to progress to the next stage of training. This kind of measurement-based competency assessment is at the center of modern entrustable professional activity (EPA) frameworks used in GI training programs internationally.
For an overview of how competency assessment integrates with simulation, the framework described in competency training in endoscopy outlines a practical approach to connecting simulation performance to clinical progression decisions.
Simulation for Trainees at Different Stages
Medical Students and Early Residents
For learners at the very beginning of their clinical training, simulation provides an introduction to the endoscopic environment and instrument handling before any patient exposure. Basic anatomy orientation, scope navigation, and air/water management can all be practiced on a simulator so that the trainee's first supervised clinical case begins at a higher starting point.
GI Residents and Fellowship Trainees
This is where the core of simulation-based GI training occurs. Residents and fellows use simulation to build navigation skills, practice polypectomy and other basic therapeutic procedures, and work through structured case libraries that expose them to pathology types and scenarios they may not encounter frequently in clinical training.
The resources available to residents entering GI training are discussed in resident training GI endoscopy, which addresses how simulation fits into the early phases of a GI fellowship.
Advanced Fellows and Endoscopists in Training
For trainees moving into advanced endoscopy, ESD, EUS, ERCP, submucosal tunnel procedures, simulation provides the specific tissue models and practice environments needed before supervised clinical cases begin. This stage of training benefits particularly from ex-vivo tissue models and high-fidelity simulators that reproduce the procedural environment of advanced techniques.
Building Confidence Before Real Cases
Beyond the measurable technical benefits, simulation contributes something harder to quantify: confidence. A trainee who enters their first supervised procedure having practiced on a simulator is less anxious, more oriented, and more capable of absorbing supervision than a trainee arriving with no prior experience.
This confidence matters for learning. Anxiety increases cognitive load and reduces the processing capacity available for skill acquisition. A trainee who is worried about where they are in the colon has less mental bandwidth for noticing the retroflexion technique being demonstrated or internalizing the feedback on their withdrawal speed. Simulation-derived familiarity reduces that baseline anxiety and frees up cognitive resources for the higher-order learning that clinical training demands.
Simulation also builds the conceptual familiarity that allows trainees to set realistic expectations for their first clinical cases. They arrive knowing what scope navigation feels like, understanding what loop management involves, and having a mental model of the procedure flow. This cognitive preparation is itself a meaningful contribution to early clinical performance.
The Role of Physical Simulators in GI Training
While virtual reality platforms receive considerable attention, physical simulators remain highly effective and are in many ways more accessible for programs with limited budgets. A well-designed physical endoscopy simulator provides realistic scope handling, anatomical navigation practice, and, in more advanced models, tissue interaction for therapeutic skill development.
The GI Endoscopy Simulator from SuzhouFrank provides a physical platform that supports both upper and lower GI endoscopy training, including scope navigation and basic interventional skill practice. For programs developing trainees in advanced procedures, the GI ESD Surgical Simulator provides the tissue environment necessary for ESD technique development.
Physical simulators are compatible with standard endoscopic instruments, do not require software licensing, and can be used independently by trainees during self-directed practice sessions, all features that support accessible, high-volume repetition.
SuzhouFrank: Simulation Equipment for GI Endoscopy Training
SuzhouFrank is a manufacturer of medical simulation equipment focused on procedural training in GI endoscopy, bronchoscopy, and minimally invasive surgery. Their physical training models are designed to meet the specific technical demands of endoscopy education at every stage, from foundational navigation to advanced therapeutic skills.
The full catalogue of simulation products is available at https://www.suzhoufrank.com/all-products#endoscopic-intervention-training-model. Programs and institutions interested in discussing equipment options or building a simulation curriculum can reach the team through the contact page.
Conclusion
GI endoscopy is a specialty where technical skill directly affects patient outcomes, and where that skill takes time, volume, and structured training to develop. Simulation addresses the limitations of purely clinical training by providing a safe environment for early skill development, standardized exposure to key cases and scenarios, and objective measurement of competency.
The argument for including simulation in GI endoscopy training is not that it replaces clinical experience, it is that it makes clinical experience more effective, more efficient, and safer for patients. Programs that build simulation into their curriculum from the earliest stages of training produce trainees who arrive at their first patient procedures better prepared, more confident, and measurably more competent. That is what good training looks like.
© 2025. All rights reserved.
About Us
Introduction
Development
Cooperation
Service
Main Products
Medical Grade Monitor
No 15, Jinyang road KunshanSuzhou, Jiangsu, China
