📞Customer Service: +86 13248368268 📧servicecenter@suzhoufrank.com one year replacement and warranty!
Polypectomy Training in Colonoscopy Simulation
Simulation-based polypectomy training gives trainees the repetitions needed to develop safe, consistent snare technique before working with real patients in supervised colonoscopy cases.
MEDICAL TRAINING
Dr Qi Rui
3/27/20267 min read
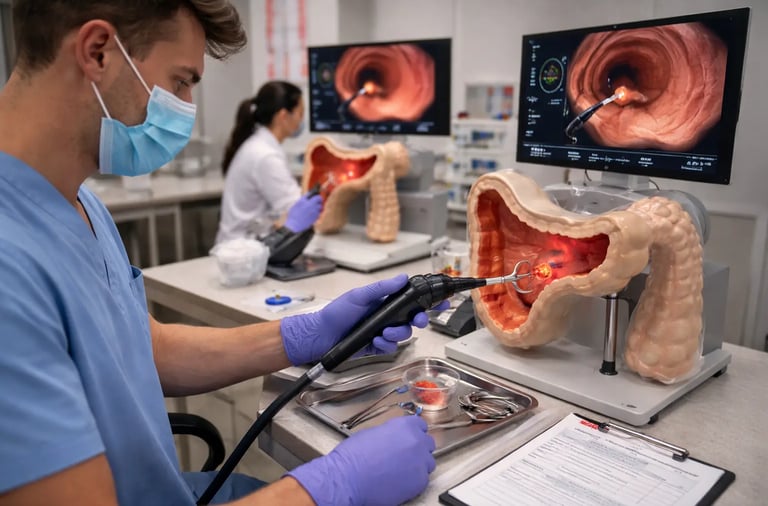
Polypectomy, the endoscopic removal of colorectal polyps, is among the most clinically important procedures performed during colonoscopy. When done correctly, it interrupts the adenoma-to-carcinoma sequence that underlies the majority of colorectal cancer cases. When done poorly, it can result in incomplete resection, perforation, or post-polypectomy bleeding, each of which carries significant patient morbidity. The stakes are high, and the technical demands are substantial.
For trainees in gastroenterology, learning polypectomy safely requires a structured approach that balances skill acquisition with patient protection. Simulation-based training has become an increasingly important part of this process, offering a platform for deliberate practice of snare technique, electrosurgical unit management, and complication avoidance before trainees perform their first unsupervised resections.
Why Polypectomy Requires Dedicated Training
Polypectomy is not simply an extension of basic colonoscopy skill. It introduces an entirely new set of technical and decision-making demands:
Polyp characterization: Correctly identifying polyp morphology (pedunculated, sessile, flat, depressed) and size influences technique selection, instrument choice, and resection strategy.
Snare selection and placement: Different polyp types require different snare sizes and shapes. Snare positioning, the degree of snare opening, the angle of approach, and the amount of stalk or tissue captured, directly determines resection adequacy.
Electrosurgical unit (ESU) settings: Polypectomy typically uses electrosurgical current to cut and coagulate simultaneously. Incorrect power settings risk incomplete resection or thermal injury.
Resection completion assessment: After snare closure, the endoscopist must confirm complete resection and assess the resection margin for residual tissue.
Complication recognition and response: Post-polypectomy bleeding and perforation must be recognized and managed promptly. These responses require a level of procedural confidence that can only come from structured training.
Each of these demands must be managed concurrently during a real procedure, making polypectomy a true multi-task challenge for trainees.
The Learning Curve for Polypectomy
Colonoscopy competence alone does not confer polypectomy competence. Studies have shown that polypectomy requires its own dedicated learning curve, separate from the skill development needed to achieve reliable cecal intubation. Specifically:
Trainees who are proficient at colonoscopy navigation may still struggle with snare placement, snare closure mechanics, and ESU management
The incidence of incomplete resection is higher in early training, even when trainees are supervised
Post-polypectomy bleeding rates in early training are elevated and can be reduced through structured technical preparation
The implication is clear: polypectomy skill must be developed deliberately, not assumed to follow automatically from general colonoscopy experience. Simulation provides the dedicated practice environment this deliberate development requires.
Polypectomy Technique: The Fundamentals
Understanding what must be practiced in simulation begins with understanding the polypectomy technique itself.
Polyp Morphology Classification
The Paris classification system categorizes colorectal polyps by their gross morphological appearance:
Type Ip (pedunculated): Polyps attached by a stalk. The snare is placed around the stalk, below the head.
Type Is (sessile): Broad-based polyps without a stalk. The snare must capture the full polyp base.
Type IIa (flat elevated): Slightly raised lesions requiring careful snare positioning or submucosal injection-assisted resection (EMR).
Type IIb (flat): Level with the surrounding mucosa, requires advanced technique.
Trainees must learn to classify polyps on sight and select the appropriate technique for each morphological type.
Snare Polypectomy Technique
For pedunculated polyps, the snare technique follows these steps:
Position the colonoscope to provide a stable, clear view of the polyp
Open the snare fully and position it above the polyp head
Lower the opened snare over the head and onto the stalk, landing it at mid-stalk position
Close the snare gradually while advancing the scope tip to center the snare
Apply electrosurgical current while slowly tightening the snare, blended cut/coagulation mode is standard for stalked polyps
Complete transection and inspect the resection site
For sessile polyps, the same general sequence applies but snare placement is more technically demanding: the snare must encompass the entire polyp base with minimal normal mucosa trapped, and ESU settings are often adjusted to favor coagulation over cutting to reduce perforation risk.
Submucosal Injection for Sessile Lesion Resection
Large sessile polyps typically require submucosal injection of saline or other lifting agents before snare resection. This technique (endoscopic mucosal resection, or EMR) raises the polyp away from the muscularis propria, creating a safety buffer that reduces perforation risk during electrosurgical resection. Trainees must learn to assess the lifting adequacy and to recognize the "non-lifting sign" that may indicate submucosal fibrosis or deep invasion.
How Simulation Supports Polypectomy Learning
Physical Polypectomy Training Models
Physical models designed for polypectomy practice include anatomically shaped colonic replicas with simulated polyps of different sizes and morphologies mounted on the mucosal surface. Trainees use real snares, real electrosurgical units (or function simulators), and real endoscopes to practice the complete resection sequence.
The primary advantages of physical models for polypectomy training include:
Real instrument interaction: Trainees learn how a real snare behaves during deployment, positioning, and closure, tactile knowledge that VR systems cannot fully replicate
Tissue resistance simulation: Physical models can replicate the resistance of polyp stalk and base tissue, calibrating the force applied during snare closure
Accessory channel mechanics: Passing and deploying a snare through a colonoscope accessory channel on a physical model is identical to clinical practice
The GI ESD Surgical Simulator from SuzhouFrank provides a sophisticated physical platform for practicing endoscopic resection techniques, including polypectomy and EMR. The simulator's tissue-mimicking surfaces and realistic anatomical geometry allow trainees to develop the scope positioning and snare manipulation skills needed for safe polyp resection.
VR Simulators with Polypectomy Modules
Several virtual reality colonoscopy simulators include polypectomy modules with computer-generated polyps of varying morphology. These systems allow trainees to practice polyp identification, technique selection, and snare placement in a controlled virtual environment. VR modules are particularly useful for:
Teaching polyp classification (Paris system recognition)
Practicing snare positioning strategy for different polyp types
Scenario training for challenging polyp locations (behind folds, at flexures, at the ileocecal valve)
Generating performance metrics (resection adequacy score, complication rate)
The combination of VR for polyp recognition and technique planning, and physical models for actual snare mechanics practice, creates a comprehensive polypectomy training program.
Staged Practice Before Live Cases
One of the most important principles of polypectomy simulation training is progression through stages. Trainees should not attempt full polypectomy on the simulator until they have mastered the prerequisite skills individually.
Stage 1: Snare Mechanics Familiarization
Before attempting simulated polypectomy, trainees should practice snare deployment, opening, and closure mechanics on a bench model outside the endoscope. This builds familiarity with the instrument before adding the complexity of endoscopic access.
Stage 2: Snare Placement on Static Models
With an endoscope in a physical colonic model, trainees practice snare positioning on simulated sessile and pedunculated polyps without applying electrosurgical current. The focus is entirely on achieving correct snare position and snare-closing mechanics.
Stage 3: Complete Resection with ESU
Once snare placement is consistently correct, trainees practice complete resection using electrosurgical current on tissue analog models. This stage develops familiarity with ESU settings, cutting technique, and resection endpoint recognition.
Stage 4: Challenging Morphology and Location
Advanced simulation sessions target difficult polypectomy scenarios: flat polyps in acute-angle segments, polyps behind folds requiring scope maneuver, and large sessile lesions requiring piecemeal resection. These scenarios prepare trainees for the variability they will encounter in clinical practice.
Stage 5: Supervised Clinical Transition
Trainees who complete staged simulation training are significantly better prepared for their first supervised patient polypectomies. Research published on PubMed has demonstrated that simulation-trained trainees show improved polyp resection adequacy and lower complication rates in early clinical cases.
For a comprehensive view of how simulation-based training integrates into the full endoscopy education continuum, see Endoscopy Training with Simulators, which covers curriculum design principles applicable across all endoscopic procedures including polypectomy.
Safety Considerations in Polypectomy Training
Polypectomy carries real procedural risks, primarily hemorrhage and perforation, that make patient safety a central training concern. Simulation training directly addresses safety through:
Complication Recognition Training
Trainees must learn to recognize post-polypectomy bleeding (immediate and delayed) and perforation, and to respond appropriately. VR simulators can present these complications in a controlled scenario, allowing trainees to practice hemostatic responses (clip application, injection therapy) and perforation management without real patient risk.
ESU Parameter Training
Incorrect electrosurgical settings are a common source of polypectomy complications. Training programs should include explicit instruction on ESU settings for different polyp types and sizes, with simulation practice using actual ESU units or realistic simulators.
Non-Lifting Sign Recognition
The non-lifting sign after submucosal injection indicates potential deep tissue involvement or fibrosis, which significantly changes the risk-benefit calculation for resection. Training trainees to recognize and respond to this sign on simulation models reduces the risk of inadvertent resection of lesions that should be referred for surgical management.
Assessment in Polypectomy Training
Objective assessment of polypectomy competence requires evaluation of multiple performance dimensions simultaneously. Key metrics include:
Resection adequacy rate: The proportion of polyps completely resected on first attempt
Complication rate: Incidence of perforation or significant bleeding
Resection technique appropriateness: Correct technique selection for polyp morphology
ESU parameter selection: Appropriate power settings for each case
For a detailed overview of how structured assessment supports endoscopy competency development, see Competency Training in Endoscopy, which covers the assessment frameworks and performance standards used in contemporary endoscopy training.
The World Health Organization's patient safety recommendations emphasize that procedural competency certification for high-risk procedures should be based on demonstrated performance rather than case volume alone, an approach that aligns directly with simulation-based assessment for polypectomy. See WHO: Patient Safety for the broader policy context.
SuzhouFrank: Simulation Equipment for Polypectomy Training
SuzhouFrank manufactures high-quality endoscopic simulation models for polypectomy and advanced therapeutic endoscopy training. Our products provide realistic tissue properties, compatible instrument channels, and anatomically accurate colonic geometry for effective snare technique development.
To explore the full range of our endoscopy training equipment, visit our catalogue at https://www.suzhoufrank.com/all-products#endoscopic-intervention-training-model. For inquiries about institutional programs, product specifications, or demonstrations, reach our team at https://www.suzhoufrank.com/contact-us.
Conclusion
Polypectomy is a high-stakes endoscopic procedure that directly reduces colorectal cancer mortality, but only when performed with consistent technical accuracy. The learning curve is real, the risks are meaningful, and the skills required go well beyond basic colonoscopy competence. Simulation-based training, using physical models for snare mechanics and tissue interaction, and VR platforms for polyp recognition and scenario practice, provides a safe, structured, and evidence-supported pathway to polypectomy competence. Programs that invest in dedicated polypectomy simulation training produce trainees who enter supervised clinical cases better prepared, safer, and more consistent in their technique. In a specialty defined by quality metrics like adenoma detection rate and complete resection rate, this preparation directly translates to better patient outcomes.
References:
© 2025. All rights reserved.
About Us
Introduction
Development
Cooperation
Service
Main Products
Medical Grade Monitor
No 15, Jinyang road KunshanSuzhou, Jiangsu, China
