📞Customer Service: +86 13248368268 📧servicecenter@suzhoufrank.com one year replacement and warranty!
Simulation Models in Healthcare Education
Simulation models in healthcare education include task trainers, mannequins, VR modules, and hybrid systems. Learn how each supports different learning objectives and skill levels.
MEDICAL TRAINING
Dr Qi Rui
3/16/20267 min read
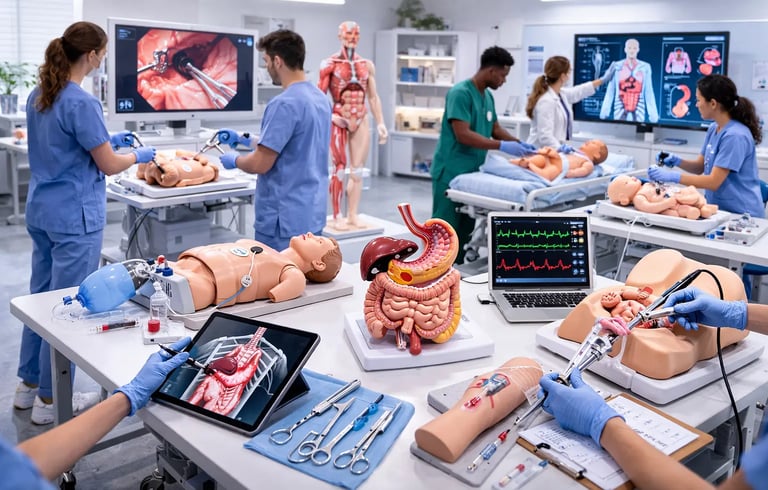
Healthcare education has undergone a fundamental shift over the past two decades. Where learners once relied almost entirely on seeing procedures done by senior clinicians and then attempting them under supervision on real patients, they now have access to a rich ecosystem of simulation tools designed to bridge the gap between classroom knowledge and clinical practice. At the heart of this ecosystem sits the simulation model, a broad term that encompasses everything from a plastic pelvis used for catheter insertion training to a full immersive virtual reality bronchoscopy system.
Understanding what a simulation model is, how different types are designed, and where each fits into healthcare education helps program directors, training coordinators, and clinical educators make better decisions about how to structure learning for their trainees.
Defining "Simulation Model" in Healthcare
A simulation model in healthcare education is any construct, physical, virtual, or hybrid, that replicates aspects of a patient, a clinical environment, or a medical procedure for the purpose of training or assessment. The term is deliberately broad because the field itself is broad.
A simulation model is not necessarily high-tech. A foam pad on which a trainee practices placing central lines is a simulation model. So is a sophisticated computerized mannequin that simulates anaphylaxis, complete with falling blood pressure, hives, and stridor. The common thread is that both provide a learning experience that stands in for, and prepares the learner for, a real clinical event.
The World Health Organization has long recognized simulation as a tool for improving patient safety outcomes, and the medical literature consistently supports its integration into formal training programs. A systematic review indexed on PubMed found that simulation-based medical education with deliberate practice leads to outcomes substantially superior to traditional clinical training alone.
The Role of Simulation Models in Healthcare Education
Simulation models serve multiple educational functions depending on where and how they are used:
Skill acquisition: Learners practice physical techniques, needle insertion, scope navigation, tissue dissection, in a controlled setting where errors carry no patient risk.
Scenario immersion: Full clinical scenarios are recreated so that trainees experience not just the technical demands of a procedure but also the monitoring, communication, and decision-making required in real settings.
Competency verification: Structured assessments conducted on simulation models provide objective evidence of skill that supports decisions about readiness for unsupervised practice.
Rare event preparation: Events that are uncommon in clinical practice, anaphylaxis, airway emergencies, rare pathology, can be simulated with reliable frequency so that trainees are prepared when they encounter them.
Deliberate practice: The ability to repeat a procedure on demand, without needing a patient to be available, allows for the kind of repetitive practice that research shows is essential to skill mastery.
These functions are described in detail in the context of gastrointestinal training through resources like clinical simulation in endoscopy, where the full arc from orientation to competency is laid out.
Core Categories of Simulation Models
Scenario-Based Mannequins
High-fidelity patient simulators, often called mannequins, are among the most widely recognized simulation models. These full-body systems allow program directors to build complete clinical scenarios around a synthetic patient who responds dynamically to interventions.
Modern mannequins can simulate:
Spontaneous breathing with adjustable rate and depth
Heart sounds, lung sounds, and bowel sounds
Peripheral and central pulses with programmable blood pressure
Pupil response
Bleeding from wounds
Drug administration responses
They are typically operated by an instructor from a control station who manages the mannequin's physiological responses in real time or runs pre-programmed scenarios. Debriefing after the scenario is a critical component, the simulation experience itself is the trigger for learning, but the debrief is where insight is generated.
Mannequins are most effective for scenarios that require managing a whole patient, anesthesia, emergency medicine, obstetric emergencies, and team-based resuscitation. They are less well-suited for detailed procedural training in specialties like endoscopy or laparoscopy, where the anatomy of a specific body region needs to be accurately reproduced at the tool-tissue interface.
Partial-Task Trainers
Partial-task trainers are simulation models designed to isolate and practice a specific subset of skills within a larger clinical procedure. Rather than recreating an entire patient encounter, they reproduce only the anatomy and mechanics relevant to the task being trained.
Examples include:
IV insertion arm models
Lumbar puncture trainers
Airway management trainers with intubatable heads
Pelvic models for speculum examination
GI tract models for scope navigation
Vessel puncture pads for arterial line training
Partial-task trainers are valued for their efficiency and repeatability. A trainee can perform the same procedure dozens of times in a session, building the muscle memory and coordination that full-scenario training does not always provide time for. Many modern partial-task trainers are instrumented, they measure insertion angle, force, or needle position and provide feedback on technique.
In endoscopy training, partial-task trainers are extensively used for skills like polypectomy, hemostatic clipping, and endoscopic submucosal dissection. The GI Endoscopy Simulator from SuzhouFrank is one example of a model that supports both navigation practice and basic interventional skills in a single platform.
Virtual Reality Modules
Virtual reality simulation uses computer-generated imagery and haptic feedback devices to replicate a clinical procedure entirely in a digital environment. The learner interacts with the simulated environment through controllers that track hand and instrument movements and, in higher-end systems, provide force feedback that approximates the resistance of real tissue.
VR modules are used across a wide range of specialties:
Upper and lower GI endoscopy
Bronchoscopy
Laparoscopy and robotic surgery
Colonoscopy with loop management
Urological endoscopy
Cardiac catheterization
The primary advantages of VR simulation are the unlimited case library, including rare pathologies that a trainee might not encounter in clinical training, and the absence of consumable costs once the platform is purchased. Every repetition costs nothing beyond the trainee's time.
The main limitations are cost (high-end VR simulators can be expensive), the learning curve of the platform itself, and the occasional gap between virtual haptics and the real tactile experience of tissue. Most programs use VR simulation alongside physical models rather than as a complete replacement.
Standardized Patients
While not models in the physical or digital sense, standardized patients, trained actors who simulate patient encounters, are a widely used form of simulation in healthcare education. They are particularly valuable for training communication skills, history-taking, physical examination, and breaking bad news.
Standardized patients are used in:
Medical school OSCE examinations
Communication skills workshops
Interprofessional education
Consent and counseling training
Because they cannot be used for invasive procedures, they are typically combined with other simulation models when full procedural scenarios are required.
Hybrid Simulation Models
Hybrid simulation combines two or more simulation types to create a more complete training experience. A common example is a physical pelvic model attached to a standardized patient actor, the learner conducts the examination conversation with a real person while using the physical model for the hands-on component.
In endoscopy and minimally invasive surgery, hybrid models often combine a physical model for instrument handling with a screen-based display for the endoscopic view. This approach gives trainees realistic hand-eye coordination practice while the visual environment is controlled and standardized.
Scenario Design in Simulation Education
The quality of a simulation model is only part of what makes simulation effective. How scenarios are designed around those models significantly affects educational outcomes.
Defining Clear Objectives
Every simulation session should begin with clearly defined learning objectives. What specific skill or knowledge should the learner acquire or demonstrate? Without this clarity, simulation time tends to drift, and learners may practice what they are already good at rather than what they need to improve.
Matching Fidelity to Purpose
Fidelity, the degree to which a model accurately reproduces reality, should match the learning objective, not be maximized for its own sake. A high-fidelity mannequin is not better than a simple task trainer for practicing scope insertion technique. Over-investing in fidelity where it is not educationally necessary wastes resources and can actually distract from the target skill.
Deliberate Practice Principles
Research by Ericsson and colleagues, widely cited in medical education literature, establishes that skill acquisition requires focused, effortful repetition with feedback and opportunities for correction. Simulation models support this by making repetition possible without patient exposure. Effective scenario design builds in the time and repetitions needed for mastery rather than assuming that a single exposure is sufficient.
Debriefing
The debrief is arguably more important than the simulation itself. Reviewing performance after a scenario, what went well, what could be improved, and why, drives the cognitive processing that turns experience into learning. Effective simulation programs build structured debrief time into every session regardless of the model type used.
For more on how these principles are applied in structured training programs, the approach to skills assessment in simulation offers a useful framework for connecting scenario design with competency measurement.
Simulation Models Across Medical Specialties
Different specialties have different simulation needs, and the range of models available reflects that diversity.
Emergency Medicine and Critical Care
Full-scenario mannequins dominate here because the learning objective is usually managing a deteriorating patient, a fundamentally whole-patient problem. Standardized patients are used for triage and communication, and partial-task trainers support procedural skills like chest decompression and IO access.
Surgery and Minimally Invasive Procedures
Laparoscopic and robotic surgery training relies heavily on box trainers (physical models with a camera and instrument ports) and VR simulators. The Laparoscopy Simulator provides an accessible platform for basic laparoscopic skill development without the overhead of operating theater time.
GI Endoscopy
Endoscopy has perhaps the richest ecosystem of simulation models of any procedure-based specialty, reflecting both the technical demands of scope navigation and the breadth of therapeutic interventions performed endoscopically. Physical task trainers, VR platforms, and ex-vivo tissue models are all used at different stages of training.
Pulmonology and Respiratory Medicine
Bronchoscopy training uses simulators that replicate the airway anatomy from the larynx through the segmental bronchi. The Endoscopy Bronchoscopy Simulator A supports foundational airway navigation practice for trainees entering pulmonology or critical care fellowships.
SuzhouFrank: Simulation Models for Procedural Healthcare Training
SuzhouFrank manufactures physical simulation models for a range of medical specialties, with particular depth in GI endoscopy, bronchoscopy, laparoscopy, and related minimally invasive procedures. Their models are designed for use in hospital training departments, medical universities, and dedicated simulation centers.
The full product catalogue, including models for endoscopic intervention training, is available at https://www.suzhoufrank.com/all-products#endoscopic-intervention-training-model. For institutional inquiries, custom configurations, or pricing information, the team can be reached through the contact page.
Conclusion
Simulation models in healthcare education encompass a wide and evolving landscape of tools, from simple task trainers and standardized patients to high-fidelity mannequins and virtual reality platforms. Each model type serves specific learning objectives, and the most effective training programs use them in combination, matching the right model to the right learner at the right stage of development.
The goal is always the same: prepare clinicians to perform at their best before they encounter the situations that matter most. Simulation models are the tools that make that preparation possible.
© 2025. All rights reserved.
About Us
Introduction
Development
Cooperation
Service
Main Products
Medical Grade Monitor
No 15, Jinyang road KunshanSuzhou, Jiangsu, China
