📞Customer Service: +86 13248368268 📧servicecenter@suzhoufrank.com one year replacement and warranty!
Surgical Simulation: Why It Matters Before the OR
Simulation is now standard preparation for minimally invasive surgery. Discover how endoscopy and laparoscopy simulators reduce the learning curve and improve first-case performance.
MEDICAL TRAINING
Dr Qi Rui
3/13/20267 min read
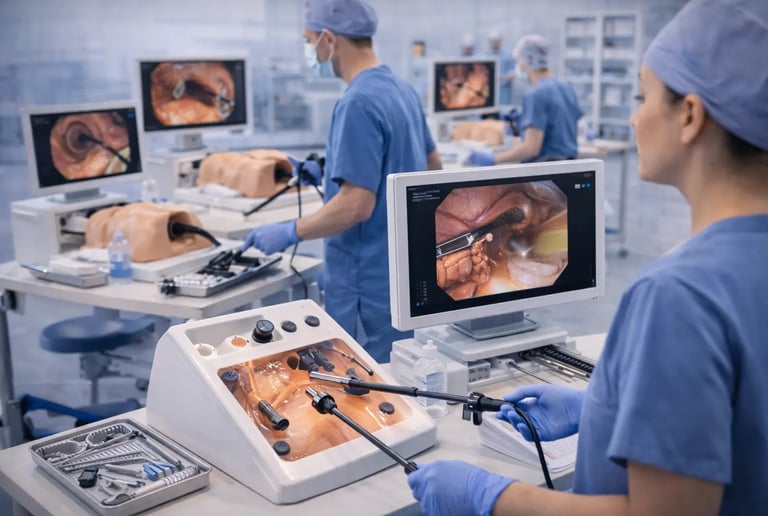
There is a moment every surgical trainee knows. You are in the operating room for the first time in a real procedural role, not as an observer, but as the person holding the instruments. The anatomy looks different than the textbook diagrams. The tissue moves. The instruments behave differently than you imagined. Your attending is watching. The patient is real.
That moment is inevitable, and experienced surgeons universally remember it. What varies, and what modern surgical education has worked hard to improve, is how prepared that trainee is when it arrives. The difference between a trainee who enters the OR with established instrument mechanics, spatial orientation, and procedural schema, versus one who is encountering these things for the first time, is not a matter of talent. It is a matter of preparation.
Surgical simulation is the infrastructure of that preparation. This article examines why simulation matters for minimally invasive surgery, with particular focus on endoscopy and laparoscopy, and how it helps trainees develop the anatomy familiarity, instrument competence, and workflow understanding they need before performing on real patients.
The Case for Pre-Operative Simulation
Patient Safety as the Foundational Argument
The most important argument for surgical simulation is patient safety. Every technical error a trainee makes while developing skill in a real operating room is an error made on a patient. Most of those errors are caught by supervisors and corrected without consequence, but not all, and not always in time. The goal of pre-operative simulation is to shift as much of the error-and-correction cycle as possible out of the operating room and into the simulation environment.
The World Health Organization's Safe Surgery initiative identifies surgical skill and training quality as directly linked to patient safety outcomes. Globally, surgical complications contribute an enormous burden of preventable harm. Pre-operative simulation is one of the most direct interventions available to reduce that burden.
The Learning Curve Problem in Surgery
Every surgical procedure has a learning curve, a period during which the trainee's performance is below the competency of an experienced practitioner. During this period, procedures take longer, complication rates are higher, and outcomes are less reliable. Learning curves are not inherently dangerous; they are unavoidable features of skill acquisition. But their shape, how long they last and how steep the initial performance deficit is, can be modified by preparation.
Research published through PubMed demonstrates that simulation-trained surgical trainees enter clinical practice with compressed learning curves across multiple procedure types. They begin at a higher baseline of technical skill, reach competency faster, and generate fewer procedure-related complications during the transition period.
Pre-operative simulation does not eliminate learning curves, it front-loads them. The errors and corrections that shape skill development happen in the simulation lab, not the operating room.
Endoscopy Simulation: Anatomy Without the Patient
What Trainees Need to Know Before Their First Case
Flexible endoscopy requires a set of skills that are genuinely non-intuitive. Moving a flexible scope through three-dimensional anatomy using a combination of tip deflection wheels, shaft torque, and push-pull mechanics is unlike anything in everyday experience. The scope bends, loops, and transmits force in ways that require spatial understanding that develops only through practice.
Specifically, trainees entering their first supervised endoscopy cases need:
Instrument mechanics, Understanding how the angle knobs translate to tip movement, how torque applied at the shaft propagates to the tip, and how the combination of these controls produces directional navigation in three-dimensional space.
Anatomical orientation, The ability to recognize landmarks on the endoscopic video image and correlate them with the scope's current position in the patient's anatomy. In colonoscopy, this means recognizing haustra, knowing what the hepatic and splenic flexures look like, and identifying the cecum. In upper endoscopy, it means orienting in the esophagus, stomach, and duodenum.
Loop recognition and management, Recognizing when the scope has looped in the sigmoid or transverse colon, and understanding the technique for loop reduction.
Basic interventional mechanics, For trainees who will perform polypectomy or biopsy, understanding how biopsy forceps and snares behave within the biopsy channel and against tissue.
Physical endoscopy simulators allow trainees to develop all of these competencies before their first patient encounter. The GI Endoscopy Simulator provides realistic anatomical geometry and tissue compliance that translates directly to clinical performance.
Advanced Endoscopic Procedures
Beyond basic upper and lower GI endoscopy, simulation is increasingly applied to advanced procedures:
Endoscopic submucosal dissection (ESD), One of the most technically demanding endoscopic procedures, ESD requires precise dissection in the submucosal layer using dedicated electrosurgical instruments. The consequences of incorrect technique, perforation, bleeding, incomplete resection, are significant. Pre-operative simulation on layered tissue models allows trainees to develop the tissue interaction skills required before their first case. The GI ESD Surgical Simulator is purpose-built for this application.
ERCP, Biliary and pancreatic endoscopy demands side-viewing scope mechanics, fluoroscopic guidance, and biliary cannulation technique that differ substantially from standard endoscopy. Simulator-based ERCP training allows trainees to develop the specific instrument mechanics of side-viewing scope navigation and biliary cannulation.
Bronchoscopy, The airway anatomy traversed in bronchoscopy, trachea, carina, lobar and segmental bronchi, is complex and three-dimensional in a way that is genuinely disorienting on first encounter. Bronchoscopy simulators provide the anatomical orientation training that reduces confusion in early supervised cases.
Laparoscopy Simulation: Operating in a Box
The Unique Challenges of Laparoscopic Surgery
Laparoscopic surgery presents a set of cognitive and motor challenges that differ fundamentally from open surgery:
Restricted field of view, The laparoscopic camera provides a two-dimensional image of a three-dimensional field. Depth perception must be reconstructed from visual cues rather than direct tactile and spatial experience.
Fulcrum effect, Laparoscopic instruments enter the abdomen through fixed port sites. Moving the instrument handle upward moves the instrument tip downward inside the patient, the opposite of intuitive direct manipulation. This fulcrum inversion takes significant practice to internalize.
Reduced tactile feedback, Laparoscopic instruments transmit reduced tactile information compared to open surgery. Force application requires calibration through visual feedback rather than hand sensation.
Two-dimensional to three-dimensional translation, Operating effectively in three-dimensional anatomy while viewing a two-dimensional image requires spatial reasoning that is genuinely trainable, but requires practice.
These challenges mean that laparoscopic trainees can cause harm through instrument misuse before they have any intuitive sense of what they are doing wrong. Pre-operative simulation specifically addresses each of these challenges in a safe environment.
Box Trainers and Simulator-Based Laparoscopy Training
Laparoscopy training typically begins with box trainers, simple enclosures with instrument ports that allow trainees to practice instrument handling, cutting, suturing, and tissue manipulation while viewing their work through a camera. Box trainers are low-cost, highly effective for developing instrument mechanics, and can be used with real instruments.
More sophisticated laparoscopy simulators add virtual reality environments, haptic feedback, and automated performance metrics. These are valuable for progressive training and competency assessment.
The Laparoscopy Simulator from SuzhouFrank provides a physical training environment for laparoscopic instrument mechanics that prepares trainees for supervised clinical cases.
OR Workflow Familiarity Through Simulation
Beyond instrument mechanics and anatomical orientation, surgical simulation can prepare trainees for the operational context of the operating room.
Team Communication and Role Clarity
The OR is a team environment. The surgeon, assistant, scrub nurse, circulating nurse, and anesthesiologist each have defined roles that must be coordinated smoothly for procedures to run safely and efficiently. Trainees who understand these roles before their first OR case integrate into the team more effectively and create fewer disruptions.
Simulation scenarios that incorporate OR team dynamics, requesting instruments, communicating findings, managing unexpected intraoperative events, build procedural and interpersonal competency simultaneously.
Equipment and Technology Familiarity
Modern minimally invasive surgery depends on a complex array of equipment: video processors, insufflation systems, electrosurgical units, stapling devices, ultrasonic energy devices. Trainees who are unfamiliar with this equipment in the OR create delays and distractions. Simulation environments equipped with representative technology allow trainees to develop equipment familiarity before clinical cases.
Complication Recognition and Management
One of the most valuable applications of high-fidelity surgical simulation is training for intraoperative complications. Perforation recognition in endoscopy, bleeding management, conversion decision-making in laparoscopy, these scenarios can be simulated in ways that build the pattern recognition needed to respond quickly and correctly when they occur in a real patient.
Evidence Supporting Pre-Operative Simulation
The evidence base for surgical simulation has grown substantially over the past two decades. Multiple systematic reviews and meta-analyses demonstrate that simulation-trained trainees:
Achieve competency in fewer supervised clinical cases
Generate lower complication rates during their training period
Perform better on objective technical assessment metrics
Report higher confidence entering their first supervised cases
These findings are consistent across endoscopy, laparoscopy, and other minimally invasive procedure domains. The argument for pre-operative simulation is not theoretical, it is supported by a robust empirical record.
For a deeper dive into how simulation integrates with clinical training in GI specifically, see Clinical Simulation in Endoscopy, which examines the evidence base and curriculum implications in detail.
From Simulation to the OR: The Transition
Simulation prepares trainees for the OR; it does not replace the OR experience. The transition from simulation to supervised clinical practice is an important phase that requires deliberate management.
Supervised Clinical Cases as Simulation Extension
The first supervised clinical cases following simulation training should be structured as an extension of the simulation curriculum, targeted at specific skills, with deliberate observation by the supervising faculty. Debriefing after supervised cases, as after simulation sessions, accelerates learning.
Progressive Independence
As trainees demonstrate competency in supervised settings, the level of supervisor intervention decreases. This progressive independence, the gradual transfer of decision-making and technical responsibility from supervisor to trainee, is the mechanism through which simulation-based preparation translates into clinical competence.
The Competency Training in Endoscopy framework provides guidance on structuring this transition and documenting the competency milestones that govern it.
SuzhouFrank: Simulation Equipment That Bridges Lab and OR
SuzhouFrank manufactures medical simulation training equipment designed to prepare trainees for real procedural performance. Their product range covers the full spectrum of minimally invasive procedures, endoscopy, laparoscopy, bronchoscopy, ESD, and more, with physical models engineered for anatomical realism and instrument compatibility.
For surgeons, program directors, and simulation educators looking to build or expand pre-operative simulation capability, explore the full range at the SuzhouFrank endoscopic intervention training model catalogue. Institutional inquiries, product evaluations, and program consultations are welcome through the contact page.
Conclusion
Surgical simulation matters before the OR because patients matter in the OR. The errors trainees make while learning to navigate anatomy, manage instruments, and coordinate with surgical teams should happen on simulators, not on patients. The evidence is clear, the tools are available, and the educational frameworks to support structured pre-operative simulation are well established.
Programs that invest in pre-operative simulation infrastructure are not adding a luxury feature to their training programs. They are fulfilling the fundamental obligation of surgical education: to send trainees into the operating room as prepared as possible to do the job safely and well.
References:
World Health Organization, Safe Surgery: https://www.who.int/teams/integrated-health-services/patient-safety/research/safe-surgery
PubMed, surgical simulation outcomes research: https://pubmed.ncbi.nlm.nih.gov/
© 2025. All rights reserved.
About Us
Introduction
Development
Cooperation
Service
Main Products
Medical Grade Monitor
No 15, Jinyang road KunshanSuzhou, Jiangsu, China
