📞Customer Service: +86 13248368268 📧servicecenter@suzhoufrank.com one year replacement and warranty!
Task Trainers in Endoscopy and GI: Focused Skill Practice
In endoscopy training, task trainers let learners drill a single technique until it becomes automatic. Discover how they fit into GI programs and which skills they target most effectively.
MEDICAL TRAINING
Dr Qi Rui
3/17/20267 min read
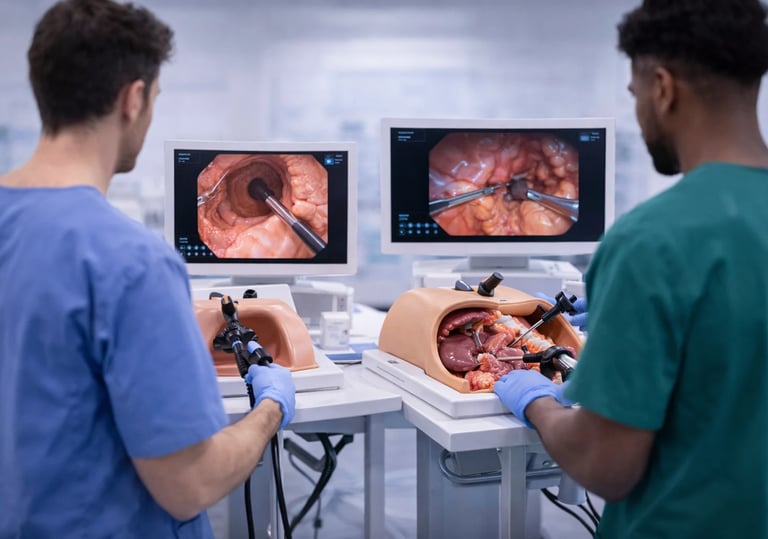
There is a paradox at the heart of procedural medical training: the skills that are hardest to learn safely on patients are often the ones most critical to patient safety. In gastrointestinal endoscopy, this paradox is particularly sharp. Polypectomy, endoscopic injection, hemostatic clipping, and mucosal dissection are all techniques that require precise, coordinated hand movements, and all carry real risks if performed imprecisely. Yet trainees must somehow develop those movements before they are trusted to perform them unsupervised.
The task trainer is one of the most important tools available for resolving this paradox. A focused, purpose-built practice platform, the task trainer isolates a single skill or a small cluster of related skills and allows the learner to practice that skill repeatedly, with feedback, before ever applying it to a patient. This article explains what task trainers are, how they work in GI and endoscopy training, and why they occupy such a central place in modern simulation-based education.
What Is a Task Trainer?
A task trainer is a simulation device designed to practice one specific task or a tightly defined subset of skills within a larger clinical procedure. Unlike a full-scenario simulator that recreates an entire patient encounter, a task trainer narrows the focus to exactly what needs to be practiced.
The distinction is important. A full GI endoscopy simulator might ask a trainee to navigate a scope through the esophagus, stomach, duodenum, and colon, detect polyps, and perform interventions, a complex, multi-skill challenge. A task trainer for polypectomy, by contrast, might present a single section of mucosa with a polyp and ask the trainee to snare and remove it cleanly. All cognitive load that is not directly relevant to polypectomy, navigation, orientation, communication, is removed so that the learner can focus entirely on the target skill.
This focused approach aligns with the principles of deliberate practice articulated in education research and widely applied in medical simulation. According to a foundational paper on simulation-based education available through PubMed, mastery of specific sub-skills through deliberate, repeated practice with feedback is the mechanism by which expertise develops. Task trainers are the physical tools that make deliberate practice possible in procedural medicine.
Why Task Trainers Matter Before Full Simulators
A common question in endoscopy education programs is whether task trainers are necessary when full simulators are already available. The answer is yes, and the reason comes down to cognitive load.
When a trainee is new to endoscopy, the full simulator asks them to manage too many things simultaneously: scope orientation, air and water management, wheel control, loop reduction, tissue identification, and instrument coordination. The mental demand of managing all of these together makes it difficult to focus on any single skill long enough to improve it meaningfully.
Task trainers decompose that complexity. By presenting just one skill at a time in a stable, low-distraction context, they allow the learner to:
Build the motor pattern for a specific movement
Develop the hand-eye coordination for a particular instrument
Understand the tissue response to a given technique
Make mistakes and correct them without consequences
Repeat until the movement becomes automatic
Once a skill is automated through task trainer practice, it can be integrated into the fuller simulation environment without overwhelming the trainee's attention. This staged approach, task trainer first, full simulator second, is standard in the most effective endoscopy training programs, as described in procedure training with simulators.
Types of Task Trainers in GI and Endoscopy
The range of task trainers available for GI and endoscopy training has expanded significantly as the specialty has adopted simulation more broadly. The following categories represent the most commonly used types.
Injection Trainers
Submucosal injection is a foundational technique used before polypectomy, endoscopic mucosal resection (EMR), and ESD. It requires precise needle placement at the correct depth, appropriate injection volume and speed, and visual monitoring of the bleb that forms under the mucosa.
Injection trainers provide a section of synthetic or ex-vivo mucosa with enough tissue depth to allow realistic injection practice. Trainees learn to identify the correct plane, control needle depth, and assess whether the injection has been placed correctly before they attempt the technique through a scope on a patient.
Polypectomy Trainers
Polypectomy, the removal of colorectal or gastric polyps using a snare, is one of the most commonly performed endoscopic interventions and one of the first therapeutic skills trainees are expected to develop. It requires accurate snare placement around the polyp stalk or base, controlled closure, and appropriate electrosurgical application.
Polypectomy task trainers incorporate synthetic polyps of varying size, morphology, and location. Trainees practice snare placement and closure on sessile, pedunculated, and flat polyps, each presenting different technical challenges. The trainer provides a consistent, repeatable environment for building snare technique without the time pressure and patient context of a real procedure.
Clipping Trainers
Hemostatic clipping is used to stop bleeding from a vessel or to close a mucosal defect after resection. Clip deployment through an endoscope requires precise targeting, correct opening angle, and controlled release, a sequence that takes coordination and practice to execute reliably.
Clipping task trainers reproduce the endoscopic environment of a bleeding site or post-resection defect. Trainees deploy clips repeatedly until the sequence is fluid and accurate. Some trainers are designed to test whether the clip has been placed over the target precisely, providing immediate feedback on deployment accuracy.
EMR and ESD Trainers
Endoscopic mucosal resection and endoscopic submucosal dissection are advanced techniques that require a combination of injection skill, incision control, and tissue manipulation. ESD in particular is one of the most technically demanding procedures in GI endoscopy, it requires sustained concentration, fine electrosurgical control, and the ability to manage complications like bleeding or perforation in real time.
Task trainers for EMR and ESD typically provide a section of layered tissue, mucosa, submucosa, and muscularis propria, that allows trainees to practice the full sequence: marking, injection, incision, and dissection. The GI ESD Surgical Simulator provides this kind of focused, multi-step tissue environment specifically for ESD training, enabling trainees to develop ESD technique before moving to animal lab models or supervised clinical cases.
Hemostasis Trainers
Beyond clipping, hemostasis in endoscopy involves thermocoagulation, epinephrine injection, and band ligation. Each technique has its own instrument-handling requirements and tissue interaction characteristics. Hemostasis trainers simulate active bleeding or vascular lesions to allow practice of these techniques in a context that resembles the urgency of a real bleeding event.
Navigation and Intubation Trainers
Although scope navigation is usually practiced on full simulators, dedicated navigation trainers isolate the specific challenge of advancing a scope through a region with challenging anatomy, the rectosigmoid junction, the hepatic and splenic flexures of the colon, or the pyloric canal. These trainers may be physical models with adjustable anatomy or compact bench-top platforms focused on loop formation and reduction.
How Task Trainers Fit Into a Simulation Curriculum
Task trainers are not a replacement for full simulators or supervised clinical experience, they are a complement that makes both more efficient. The most effective integration follows a clear progression.
Stage 1: Orientation and Basic Anatomy
Before task trainer practice begins, trainees benefit from orientation to the anatomy they will be working in. Basic anatomical models and didactic teaching establish the cognitive map that makes hands-on practice meaningful.
Stage 2: Isolated Skill Practice on Task Trainers
This is where task trainers do their primary work. Trainees practice individual techniques, injection, snare placement, clip deployment, repeatedly until they achieve a defined performance standard. Assessment checklists and direct observation by an instructor provide structured feedback.
Stage 3: Integration on Full Simulators
Once individual skills have been built to a baseline level of competency, trainees move to full simulators where they integrate multiple skills within a complete procedure. The full simulator challenges them to apply their task trainer skills in a more complex, dynamic context.
Stage 4: Supervised Clinical Practice
Having built both isolated skills and integrated procedural competency in simulation, trainees enter supervised clinical practice better prepared. The volume of supervision required is typically lower, and the quality of early clinical cases tends to be higher, because the learner arrives with genuine technical capability rather than starting from zero.
This progression is explored in detail in the context of structured programs in competency training in endoscopy, where the use of simulation tools across the training arc is directly addressed.
Evidence for Task Trainer Effectiveness
The evidence base for task trainers in procedural medical education is well-established. A meta-analysis published in the Annals of Surgery and widely indexed through PubMed found that simulation-based training with deliberate practice on task trainers significantly improved procedural skill compared to traditional apprenticeship approaches.
In endoscopy specifically, studies have shown that trainees who complete structured simulation-based curricula including task trainer practice reach clinical competency faster, require less correction during supervised procedures, and demonstrate lower error rates in early clinical cases than trainees who learn exclusively through supervised patient exposure.
The World Health Organization's framework for patient safety education explicitly includes simulation-based skill training as a recommended strategy for reducing procedural complications, a recommendation that task trainers directly support.
Practical Considerations for Using Task Trainers
For training program directors and simulation coordinators, several practical factors influence how task trainers are integrated into a curriculum.
Availability and accessibility: Task trainers should be available for self-directed practice outside of scheduled simulation sessions. This allows trainees to increase their repetition volume and practice at their own pace, a key advantage over relying on supervised clinical exposure alone.
Consumables management: Many task trainers use replaceable tissue inserts, synthetic or ex-vivo, that must be stocked and replaced regularly. Programs should budget for consumables when selecting task trainer platforms.
Assessment integration: Task trainers are most educationally valuable when performance on them is assessed against defined criteria. Structured checklists, video review, or instrument-based performance metrics should be integrated into task trainer sessions wherever possible.
Progressive difficulty: Where possible, task trainers should offer increasing levels of difficulty, for example, polyps of varying size and morphology, or injection targets at different tissue depths. This ensures that the trainer continues to challenge learners as their skill develops.
SuzhouFrank: Task Trainers for GI and Endoscopy Education
SuzhouFrank designs and manufactures physical simulation equipment specifically for procedural medical training, including a range of models suited for task trainer-based skill development in GI endoscopy, bronchoscopy, and related specialties. Their products are used in hospital training departments, endoscopy training centers, and medical universities worldwide.
To explore the full range of available models, including options for GI intervention, upper and lower endoscopy, and advanced procedural skills, visit the product catalogue at https://www.suzhoufrank.com/all-products#endoscopic-intervention-training-model. For direct inquiries about product specifications or institutional orders, the team is available through the contact page.
Conclusion
Task trainers occupy an essential position in GI and endoscopy education that full simulators and clinical supervision alone cannot fill. By isolating individual skills, injection, clipping, polypectomy, ESD, and allowing focused, repetitive practice in a controlled environment, they give trainees the opportunity to build technical capability before the pressure of a real procedure is present.
Used as part of a staged simulation curriculum, task trainers accelerate skill acquisition, reduce early errors in clinical practice, and give both trainees and supervisors greater confidence as learners transition to patient care. In a specialty where precision matters and complications are serious, the focused practice that task trainers enable is not just educationally valuable, it is a patient safety imperative.
© 2025. All rights reserved.
About Us
Introduction
Development
Cooperation
Service
Main Products
Medical Grade Monitor
No 15, Jinyang road KunshanSuzhou, Jiangsu, China
