📞Customer Service: +86 13248368268 📧servicecenter@suzhoufrank.com one year replacement and warranty!
Building a Simulation Lab for Endoscopy and GI Training
Building a simulation lab requires more than equipment. Discover how leading GI programs plan their simulation spaces, staff them, and integrate them with residency curricula.
MEDICAL TRAINING
Dr Qi Rui
3/12/20267 min read
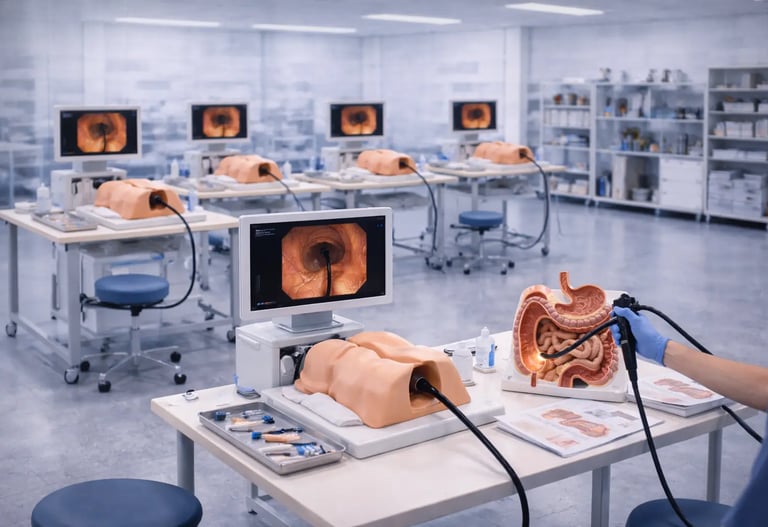
The case for simulation-based GI training is well established. The research is clear, the educational benefits are documented, and the shift toward competency-based assessment in residency and fellowship programs is already underway. What many program directors and training coordinators struggle with is not the "why" of simulation, it is the "how." How do you actually build a simulation lab? What space do you need, what equipment do you buy, how do you staff it, and how do you integrate it meaningfully into an existing training program?
This guide addresses those practical questions directly. It is intended for gastroenterology fellowship directors, GI division chiefs, nursing educators, hospital administrators, and anyone else responsible for planning a simulation training facility, whether starting from scratch or formalizing an existing informal setup.
Step 1: Define Your Training Objectives Before Buying Anything
The most common mistake in simulation lab planning is starting with equipment rather than objectives. A well-intentioned department purchases a high-fidelity simulator, installs it in a converted storage room, and discovers that no one knows how to integrate it into the training program. The equipment sits underused, and the investment is difficult to justify.
Before specifying a single piece of equipment, define what your simulation lab needs to accomplish:
Which procedures will trainees practice? (Upper endoscopy, colonoscopy, ERCP, EUS, ESD, bronchoscopy, or a combination?)
At what training levels? (Medical students, residents, fellows, attending upskilling, nursing staff?)
What are the competency objectives for each learner group?
How will simulation performance feed into credentialing or progression decisions?
How many trainees need access simultaneously, and how many hours per week of simulation time are required?
Answering these questions first shapes every subsequent decision, space requirements, equipment selection, staffing model, and scheduling structure.
Step 2: Planning the Physical Space
Minimum Viable Space
A functional endoscopy simulation lab does not require a large facility. A single room of approximately 20–30 square meters can accommodate:
Two procedure simulation stations (one for upper GI/bronchoscopy, one for lower GI/colonoscopy)
Instructor workstation and observation area
Storage for physical models, instruments, and consumables
A small debriefing area or table
For programs with broader ambitions, including laparoscopy, ultrasound, or multi-specialty simulation, additional space is needed, but the core GI simulation function can be achieved in a relatively modest footprint.
Key Space Design Considerations
Electrical and data infrastructure, Simulation equipment requires reliable power. If you are running video-integrated simulators, plan for sufficient electrical outlets, a stable data network connection, and screen mounting points for video display.
Lighting, Simulation stations should have adequate lighting for instructor observation and video recording. Overhead fluorescent lighting is functional; adjustable task lighting is better.
Ventilation and infection control, Physical models made from silicone or composite materials may require periodic cleaning with specific disinfectants. Ensure adequate ventilation and a sink with hand hygiene supplies in or immediately adjacent to the simulation space.
Storage, Physical models, spare components, accessory instruments, consumables (simulated tissue inserts, lubricants, specimen containers), and documentation materials all require organized, accessible storage. Plan for more storage than you think you need.
Observation and debriefing, Effective simulation includes structured debriefing after practice sessions. Designate a space, even a corner with chairs and a whiteboard, where trainees and instructors can review performance, watch recorded video, and discuss technique.
Step 3: Equipment Selection
Core GI Simulation Equipment
Physical endoscopy models, These are the workhorses of any GI simulation lab. At minimum, a well-equipped lab needs:
A colonoscopy model (full colon with variable loop characteristics)
An upper GI model (esophagus, stomach with retroflexion capability, duodenum)
At least one interventional model for polypectomy, injection, or hemostasis practice
For programs training in advanced procedures, add:
An ESD model with layered tissue
An ERCP model with side-viewing scope compatibility
A bronchoscopy model if pulmonary or thoracic training is included
Instrument inventory, Physical models require instruments to train with. At minimum, a simulation lab should stock training-grade endoscopes (or access to clinical endoscopes during off-hours), biopsy forceps, snares, injection needles, and hemostatic clips.
Video integration, Many training programs benefit from recording trainee sessions for debriefing review. A simple camera mounted to capture the model and the trainee's hand position provides significant educational value at modest cost.
Optional Advanced Equipment
Haptic feedback simulators, Software-based simulators with haptic interfaces add objective performance metrics and enable unsupervised practice with automated feedback. These represent a higher investment but significantly expand training capacity.
Laparoscopy trainers, If your program includes surgical training, a laparoscopy box trainer or laparoscopy simulator expands the lab's scope. The Laparoscopy Simulator from SuzhouFrank is a practical option for programs looking to integrate laparoscopic skills training alongside endoscopy.
Bronchoscopy simulators, Programs with respiratory or critical care components benefit from bronchoscopy simulation. The Ultrasound Bronchoscopy Simulator supports training for EBUS procedures and advanced bronchoscopy techniques.
Equipment Selection Criteria
When evaluating physical simulation models, assess:
Anatomical fidelity, does the model reproduce the geometry and tissue properties trainees will encounter clinically?
Durability, how many training cycles can the model withstand before components require replacement?
Instrument compatibility, does the model accept the instruments trainees will use in practice?
Maintenance requirements, what cleaning protocols are required, and are replacement parts available?
Supplier support, can the manufacturer provide technical support, spare components, and educational guidance?
Step 4: Staffing the Simulation Lab
Simulation Lab Director
Every effective simulation program has a designated clinical director, typically a senior faculty member with both clinical expertise and interest in medical education. This person is responsible for curriculum design, faculty training, and quality oversight of the program.
Simulation Technician or Coordinator
A dedicated simulation coordinator manages day-to-day lab operations: scheduling, equipment maintenance, supply inventory, session documentation, and technical support. This role is often underinvested in; programs that try to run simulation labs without dedicated administrative support consistently struggle with utilization and sustainability.
Faculty Instructors
Faculty members who lead simulation sessions need their own orientation to the simulation equipment and to effective simulation teaching methods. Observing a trainee on a physical model and providing useful, specific feedback is a skill, it is not automatic, even for experienced endoscopists. Invest in faculty development alongside trainee training.
Step 5: Scheduling and Access
Protected Simulation Time
The most common failure mode in simulation lab utilization is the absence of protected training time. Simulation sessions that are optional, unscheduled, or dependent on clinical downtime will simply not happen at the frequency needed to drive skill development.
Build simulation sessions into the formal training schedule:
Mandatory simulation orientation for new residents and fellows at the start of each rotation
Weekly or biweekly protected simulation sessions during the first half of training
Pre-procedure simulation rehearsal for trainees approaching their first advanced procedure cases
Open Access Hours
Beyond mandatory sessions, consider designating open-access hours during which trainees can use simulation resources independently or with a peer. Autonomous practice, particularly after initial instructor-led orientation, is a valuable supplement to supervised sessions.
Documentation and Tracking
Maintain a log of simulation session attendance, objectives addressed, and performance assessments for each trainee. This documentation serves multiple purposes: it supports competency-based credentialing decisions, demonstrates program quality to accreditors, and provides data for ongoing curriculum improvement.
Step 6: Curriculum Integration
A simulation lab that operates in isolation from the clinical training program adds limited value. The greatest impact comes when simulation is integrated into the training curriculum as a structured preparatory and assessment tool.
Baseline Assessment
Use simulation sessions at the start of training to establish individual trainee baselines. Where are skill gaps? What foundational competencies need priority attention? Individualized training plans based on baseline assessment are more efficient than uniform curricula that do not account for learner variation.
Progressive Skill Building
Structure simulation use to advance in parallel with clinical training exposure. As trainees begin supervised clinical cases, simulation sessions should reinforce and extend what they are encountering in the endoscopy suite, not repeat the same introductory content.
Pre-Clinical Procedure Rehearsal
Before trainees perform their first supervised case of a new procedure type, schedule a mandatory simulation rehearsal session. This pre-clinical rehearsal is one of the highest-value uses of simulation time, and the evidence for its impact on clinical performance is substantial.
For a detailed framework on structuring simulation curricula, see Simulation Curriculum Endoscopy.
Integration with Residency and Fellowship Programs
For programs aligned with formal residency or fellowship training, simulation lab activities should be documented in the format required by the relevant accreditation body. In the United States, ACGME milestone documentation increasingly expects evidence of simulation-based training. In other jurisdictions, similar requirements are emerging.
The Resident Training GI Endoscopy and Fellowship Training Advanced Endoscopy resources provide guidance on integrating simulation into formal training program structures.
Budget Considerations
Initial Setup Costs
A basic GI simulation lab can be established for a relatively modest investment. A functional setup with two or three physical models and basic instrument inventory is achievable in the range of several thousand to low tens of thousands of dollars, depending on model selection and whether clinical-grade instruments are already available.
High-fidelity software-based simulators represent a higher investment, typically $30,000–$100,000 or more for a single station, but provide capabilities (automated metrics, unsupervised practice, advanced procedure simulation) that justify the cost for high-volume programs.
Ongoing Costs
Budget for consumable replacement (model components, simulated tissue inserts), equipment maintenance, instrument repair, and staff time. Labs that fail to budget for ongoing costs find their initial investment depreciating rapidly.
Return on Investment
The ROI of simulation infrastructure is not primarily financial, it is measured in training quality, competency outcomes, and patient safety. Programs that can demonstrate faster trainee progression, lower complication rates, and documented competency achievement have a compelling case for continued investment.
According to the World Health Organization, investment in healthcare professional training, including simulation-based programs, is among the most cost-effective interventions for improving patient safety outcomes.
SuzhouFrank: Equipment and Support for Simulation Lab Development
SuzhouFrank works with simulation lab developers, training program directors, and hospital educators to supply physical endoscopy training equipment for new and expanding simulation facilities. Their product range covers the full spectrum of GI endoscopy, bronchoscopy, laparoscopy, and interventional procedures.
Browse the complete catalogue at SuzhouFrank's endoscopic intervention training model page to review the available options. For program planning assistance, bulk pricing inquiries, or customization discussions, visit the SuzhouFrank contact page.
Conclusion
Building a simulation lab is a meaningful institutional investment, but it does not require a large space, an enormous budget, or a complex infrastructure to start. A clearly defined set of training objectives, a modest but well-chosen set of physical simulation models, a structured curriculum, protected training time, and a designated coordinator are the core ingredients of a functional and effective simulation program.
Start with those fundamentals, document what you do, measure outcomes, and build from there. The programs that have had the greatest impact on training quality did not start with the best equipment, they started with the clearest vision of what they were trying to accomplish.
© 2025. All rights reserved.
About Us
Introduction
Development
Cooperation
Service
Main Products
Medical Grade Monitor
No 15, Jinyang road KunshanSuzhou, Jiangsu, China
