📞Customer Service: +86 13248368268 📧servicecenter@suzhoufrank.com one year replacement and warranty!
Endoscopy Models for GI Training: How They're Used
Discover how endoscopy models support GI training through realistic anatomy, scope handling practice, and basic intervention techniques. Complete guide inside.
MEDICAL TRAINING
Dr Qi Rui
3/9/20265 min read
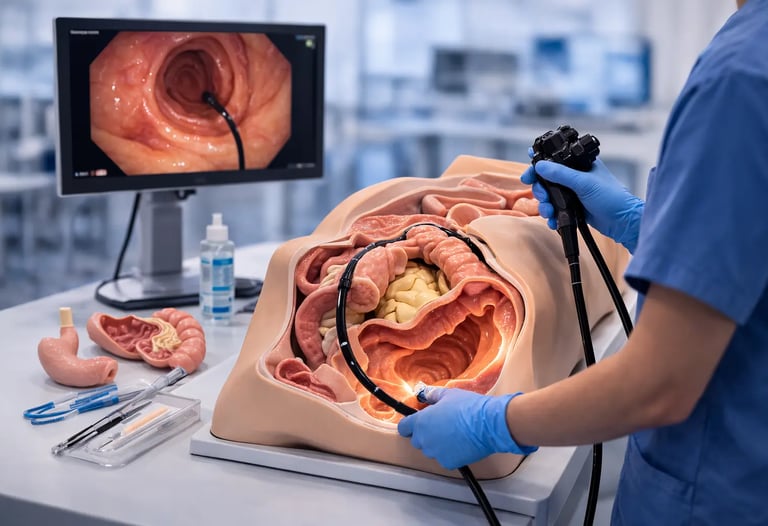
Physical endoscopy models form the backbone of hands-on procedural training across gastroenterology programs worldwide. These anatomical replicas allow trainees to develop fundamental skills in scope handling, navigation, and basic interventions before encountering real patients. Understanding how endoscopy models are constructed and deployed within training curricula helps program directors make informed equipment decisions and optimize educational outcomes.
What Are Endoscopy Models?
Endoscopy models are physical training devices that replicate human anatomical structures, enabling clinicians to practice endoscopic procedures in controlled environments. Unlike virtual reality simulators that generate computer-generated imagery, physical models provide tangible surfaces that trainees can see and feel while manipulating actual or simulated endoscopes.
The fundamental design of most endoscopy models follows a consistent pattern. An external rigid case, typically constructed from durable plastic, provides structural support and defines the training workspace. Inside this framework sits a phantom made from soft materials such as silicone that replicates the visual appearance and mechanical properties of gastrointestinal tissues. Cavities within the phantom allow endoscope insertion, creating pathways that approximate the anatomical routes encountered during clinical procedures.
Research published in Cancers journal describes how physical simulators aim to reproduce mechanical and visual properties of the GI tract with high fidelity, focusing on accurate selection of appropriate materials, molds, and surface textures. This attention to realistic construction directly impacts training quality by providing authentic tactile feedback during scope manipulation.
Construction Materials and Manufacturing Approaches
The materials used in endoscopy model construction significantly influence their training effectiveness and durability. Medical-grade silicone remains the most common choice for internal anatomical structures due to its tissue-like compliance and resilience under repeated use. Different silicone formulations can be tuned to approximate specific tissue characteristics, with softer compounds representing mucosal surfaces and firmer materials simulating muscular layers.
Modern manufacturing increasingly incorporates three-dimensional printing technology. Organs can be digitally reconstructed from computed tomography imaging data, then converted to physical models using specialized printers and materials. This approach enables creation of anatomically accurate replicas based on actual patient scans, potentially including pathological variations that trainees should learn to recognize.
Some cost-effective training solutions utilize readily available materials including PVC tubing, latex balloons, and foam components. While lacking the sophisticated realism of commercial products, these DIY approaches can provide basic skill development opportunities for programs with limited budgets. Studies have documented effective training programs built around such economical models, particularly for early-stage learners focused on fundamental scope handling.
Applications in Scope Handling Training
The primary application of endoscopy models centers on teaching basic scope manipulation skills. Novice trainees must master several coordinated movements before safely performing procedures on patients: dial control for tip deflection, torque application through shaft rotation, and balanced advancement without excessive force. Physical models provide safe environments for developing these foundational competencies.
A comprehensive review in Clinical Endoscopy notes that mechanical models excel during initial training phases and offer superior haptic realism compared to virtual alternatives. This tactile authenticity proves particularly valuable for teaching trainees to recognize appropriate resistance levels and pressure applications. The medical simulation guide provides detailed frameworks for integrating physical models into structured training programs.
Upper GI models support training in esophageal intubation, gastric navigation, and duodenal examination techniques. Trainees practice advancing scopes through anatomical landmarks while maintaining clear visualization and appropriate insufflation. The Gastrointestinal Endoscopy Simulator offers realistic upper tract anatomy enabling systematic practice of diagnostic EGD maneuvers from oral insertion through pyloric passage.
Lower GI models present different challenges reflecting colonic anatomy. Loop formation and reduction techniques require dedicated practice, as successful colonoscopy depends heavily on minimizing looping while maintaining forward progress. Models featuring configurable colon tubes allow instructors to create varying difficulty levels, progressively challenging trainees as their skills develop.
Supporting Navigation and Orientation Skills
Beyond basic handling, endoscopy models support development of spatial orientation skills critical for procedural success. Trainees must learn to interpret two-dimensional monitor images while mentally constructing three-dimensional anatomical maps. This translation between visual input and spatial understanding develops gradually through repeated practice.
Transparent model designs allow visual observation of scope behavior within anatomical structures, providing immediate feedback about loop formation, tip position, and overall scope configuration. This external visualization supplements the endoscopic view, helping trainees connect scope movements with resulting changes in position and orientation.
For bronchoscopy training, models replicating branching airway anatomy challenge trainees to navigate systematically through progressively smaller passages. The Bronchoscopy Simulator Type B features four-level bronchial branch configurations with both visual and closed training modes, accommodating learners at different skill levels.
Enabling Basic Intervention Practice
While primarily valuable for diagnostic procedure training, many endoscopy models also support practice of fundamental therapeutic interventions. Modular designs allow attachment of simulated polyps, lesions, or other pathological features that trainees can target with appropriate instruments.
Biopsy technique development benefits significantly from model-based practice. Trainees learn to position scopes appropriately, advance forceps through working channels, and execute tissue sampling maneuvers with proper targeting and force application. These coordinated actions require repetitive practice that models safely accommodate.
Polypectomy training presents opportunities for snare placement and tissue capture practice. Some models incorporate tissue elements that respond realistically to electrosurgical energy, though most focus on mechanical aspects of snare technique. The Gastrointestinal ESD Surgical Simulator provides advanced capabilities for practicing therapeutic techniques including submucosal dissection approaches.
Research in Gastroenterology & Hepatology documented that simulation training provides novice endoscopists with early advantages in developing procedural skills. Fellows who trained with simulators performed better during subsequent patient procedures, and their patients reported less discomfort compared to traditionally trained counterparts.
Cross-Specialty Training Applications
The principles underlying GI endoscopy models extend to other endoscopic specialties, each requiring discipline-specific anatomical replicas. Training programs across multiple departments can share fundamental equipment philosophies while utilizing specialty-appropriate models.
Pulmonary medicine programs utilize airway models for bronchoscopy training, with configurations ranging from basic navigation practice through interventional procedures. The Ultrasound Bronchoscopy Simulator addresses growing training needs in endobronchial ultrasound techniques increasingly used for lung cancer staging.
Urological endoscopy requires distinct anatomical models reflecting lower urinary tract structures. The Urological Endoscopy Simulator supports cystoscopy and related procedure training with appropriate bladder and urethral anatomy.
Gynecologic training utilizes hysteroscopy models enabling uterine cavity navigation and intervention practice. The Hysteroscopy Simulator provides realistic training environments for diagnostic and operative hysteroscopic procedures.
Integrating Models into Training Curricula
Effective utilization of endoscopy models requires thoughtful integration into broader educational frameworks. Models serve best as components within comprehensive curricula that also include didactic instruction, mentored patient procedures, and assessment tools. The simulation curriculum guide outlines strategies for incorporating simulation resources into cohesive training programs.
Progressive training sequences typically begin with basic handling exercises on mechanical models, advance through increasingly complex scenarios, and culminate in supervised patient procedures. This staged approach allows trainees to build foundational competencies before facing clinical complexity, potentially accelerating overall skill acquisition.
Assessment applications represent growing uses for endoscopy models. Standardized scenarios enable objective comparison of trainee performance, supporting competency documentation and identifying areas requiring additional focus. Programs implementing skills assessment protocols benefit from reproducible testing conditions that models provide.
About Suzhou Frank Medical
Suzhou Frank Intelligent Technology Co., Ltd., headquartered in Suzhou, Jiangsu Province, China, manufactures medical endoscopic imaging systems and clinical simulation training equipment. The company produces HD and fluorescence imaging platforms alongside comprehensive training models spanning gastrointestinal, respiratory, urological, and gynecologic specialties.
Training programs seeking to establish or expand simulation capabilities can review the complete product catalog featuring endoscopy models designed for various training applications. For equipment specifications, pricing information, and institutional consultation, contact the Suzhou Frank team directly.
Conclusion
Endoscopy models provide essential training infrastructure for developing procedural competency across endoscopic specialties. Constructed from materials designed to approximate tissue properties, these physical devices support scope handling practice, navigation skill development, and basic intervention training in controlled environments. Strategic integration into comprehensive curricula maximizes their educational value, helping trainees build foundational skills before progressing to supervised patient care.
© 2025. All rights reserved.
About Us
Introduction
Development
Cooperation
Service
Main Products
Medical Grade Monitor
No 15, Jinyang road KunshanSuzhou, Jiangsu, China
