📞Customer Service: +86 13248368268 📧servicecenter@suzhoufrank.com one year replacement and warranty!
Gastroscopy Training: How Simulators Support Early Learning
How do training programs use simulation to teach gastroscopy? This guide explains the curriculum structure, simulator types, and assessment methods used to build upper GI competence.
MEDICAL TRAINING
Dr Qi Rui
3/21/20266 min read
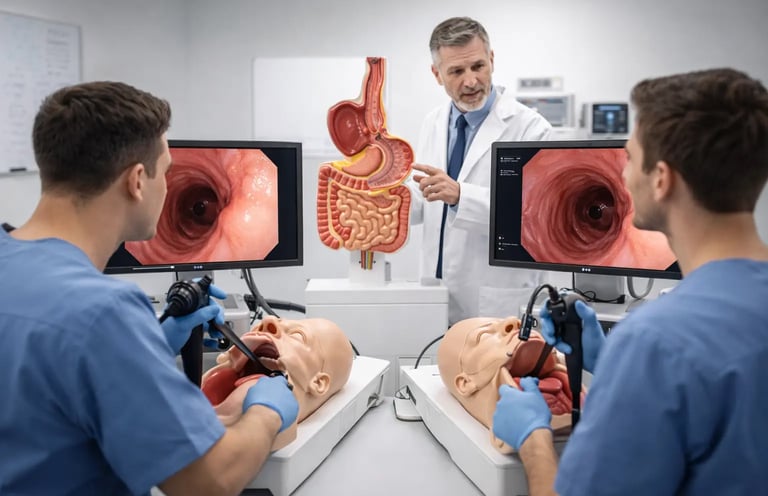
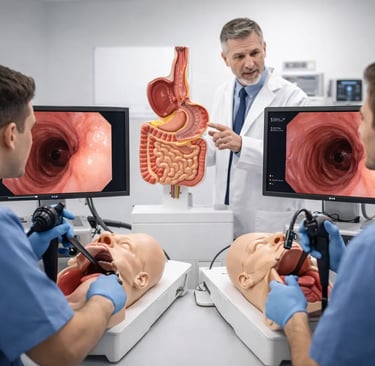
Gastroscopy is one of the most commonly performed endoscopic procedures worldwide, used to examine the esophagus, stomach, and duodenum for conditions ranging from acid reflux disease to early gastric cancer. Despite its frequency, learning gastroscopy is not trivial. A trainee must develop simultaneous competence in scope insertion, image interpretation, patient communication, and procedural decision-making, often under time pressure and in the presence of conscious, anxious patients. The early learning curve is steep, and the traditional approach of "see one, do one, teach one" has long been recognized as insufficient for building reliable, safe technique.
Simulation-based training has emerged as a critical bridge between theoretical knowledge and supervised clinical practice. By allowing trainees to practice gastroscopy in a risk-free environment, simulators reduce the burden placed on patients during early skill acquisition and help programs deliver more consistent, measurable training outcomes.
Why Gastroscopy Is Challenging to Learn
Gastroscopy requires a coordinated skill set that takes time to develop. Unlike many clinical tasks, the endoscopist must navigate a flexible instrument through a dynamic, curved anatomy while maintaining orientation in a two-dimensional video feed that does not always correspond intuitively to the physical space being explored.
Cognitive and Psychomotor Demands
New trainees frequently struggle with three distinct challenges simultaneously:
Spatial disorientation: Understanding which direction the scope tip is moving relative to the image on screen requires a mental model that must be built through repetition.
Torque and tip control: Gastroscopy demands fine-tuned coordination between the left hand (holding the control section) and the right hand (advancing, withdrawing, and torquing the shaft).
Mucosal recognition: Identifying normal from abnormal mucosa requires both experience and attentiveness that is difficult to develop during brief supervised sessions.
When trainees must focus cognitive bandwidth on basic scope mechanics, they have less capacity for image interpretation and patient safety. This is exactly where simulation adds the most value.
The Structure of Gastroscopy Training
Most gastroscopy training programs follow a progression from foundational skills to complete supervised procedures. Simulation fits naturally into the early and intermediate stages of this progression.
Stage 1: Pre-Clinical Orientation
Before touching a live endoscope, trainees benefit from understanding the mechanics of the instrument. This includes learning how the control dials affect tip deflection, how to hold and support the scope correctly, and how to advance and withdraw without causing patient discomfort. Physical models and box trainers provide this orientation without requiring clinical time.
Stage 2: Simulator-Based Skill Acquisition
Simulation-based training allows for deliberate practice of core gastroscopy skills including:
Transoral insertion and navigation through the pharynx
Esophageal intubation and recognition of the gastroesophageal junction
Gastric inflation and systematic inspection of all mucosal folds
Pyloric identification and duodenal intubation
Retroflexion in the gastric fundus
Controlled withdrawal and scope removal
These maneuvers can be repeated many times without patient exposure, allowing trainees to build muscle memory and spatial confidence before their first supervised case. For a broader overview of how simulation supports endoscopy education across multiple specialties, see Medical Simulation in Endoscopy and GI Training.
Stage 3: Supervised Clinical Cases with Performance Tracking
After simulation-based foundations are established, trainees begin supervised patient cases. At this stage, the transition is smoother because fundamental scope control has already been internalized. Trainers can focus feedback on image interpretation, communication, and procedural decision-making rather than basic mechanics.
Evidence for Simulation in Gastroscopy Training
The evidence base for simulation in upper GI endoscopy training has grown substantially over the past decade. Multiple studies have demonstrated that trainees who complete structured simulator-based training before clinical cases achieve competence faster and with fewer patient discomfort events.
A landmark study published in Gastrointestinal Endoscopy found that simulator-trained residents demonstrated significantly better technical performance during their first 20 clinical gastroscopy cases compared to controls who received only standard apprenticeship training. The effect was most pronounced in scope insertion success and time to reach the duodenum.
The American Society for Gastrointestinal Endoscopy (ASGE) and the European Society of Gastrointestinal Endoscopy (ESGE) both recommend simulation as a component of endoscopy training programs. The ESGE curriculum specifically identifies simulation as appropriate for pre-clinical orientation and early skill development in gastroscopy, esophageal intubation, and systematic mucosal survey.
Research published on PubMed has documented the effectiveness of simulator-based curricula in accelerating gastroscopy competence among gastroenterology fellows, reinforcing what many program directors have observed clinically.
Types of Simulators Used in Gastroscopy Training
Two major categories of simulators are used in gastroscopy training: virtual reality (VR) simulators and physical/mechanical models. Each has distinct advantages depending on the learning objective.
Virtual Reality Simulators
VR simulators generate computer-rendered anatomy that responds to scope manipulation in real time. They typically include:
Haptic feedback to simulate tissue resistance
Automated performance metrics (insertion time, mucosal visualization score, patient discomfort index)
Libraries of pathology cases including ulcers, tumors, Barrett's esophagus, and varices
VR simulators are well-suited to systematic mucosal survey training and image interpretation, because the same anatomical scenario can be run repeatedly under controlled conditions. They are less effective for practicing accessory channel skills like biopsy, which require physical instrument handling.
Physical Endoscopy Models
Physical models use anatomically shaped silicone or latex structures to replicate the esophagus, stomach, and duodenum. Trainees use real endoscopes and accessories on these models, which makes them ideal for practicing accessory tasks, learning force application, and familiarizing with instrument handling before clinical use.
The GI Endoscopy Simulator from SuzhouFrank is a high-quality physical training model designed for gastroscopy and upper GI procedure practice. It provides realistic tactile feedback and allows repeated, low-cost training sessions for individual trainees or groups.
Designing an Effective Gastroscopy Simulation Curriculum
A well-structured gastroscopy simulation curriculum should include clear learning objectives, defined milestones, and objective performance assessment at each stage.
Key Curriculum Components
1. Pre-training Assessment Baseline psychomotor testing helps instructors understand where individual trainees start and tailor instruction accordingly.
2. Structured Simulator Sessions Each session should target a specific skill (e.g., duodenal intubation only, or retroflexion only) rather than asking trainees to practice the entire procedure each time. Targeted deliberate practice accelerates skill acquisition more effectively than unstructured repetition.
3. Debriefing and Feedback After each simulation session, a brief structured debrief with an experienced endoscopist reinforces correct technique and addresses errors before they become ingrained habits.
4. Transition Criteria Programs should define objective criteria that must be met on the simulator before a trainee advances to supervised patient cases. This protects patients and ensures training consistency across the cohort.
For a broader view of how simulation fits into the overall endoscopy training progression, see Endoscopy Training with Simulators, which covers curriculum design principles applicable across upper and lower GI procedures.
Common Mistakes in Early Gastroscopy Training
Understanding the most frequent errors made by novice gastroscopists helps instructors design simulator training that specifically targets these failure points.
Over-Reliance on Tip Deflection
Beginners often over-use the control dials to steer the scope tip, resulting in looping, patient discomfort, and loss of visualization. Simulation allows trainees to develop the habit of using torque and shaft advancement as primary navigational tools, with tip deflection reserved for fine adjustment.
Inadequate Mucosal Survey
Systematic inspection of all gastric regions is a learned skill. Trainees frequently miss areas, particularly the posterior gastric body and the fundus on retroflexion. Structured simulation sessions dedicated to systematic survey technique help establish the habit of complete inspection early.
Rushed Pyloric Intubation
Impatience during pyloric intubation leads to trauma and failed duodenal entry. Simulation allows trainees to practice patience, positioning, and the waiting technique that allows the scope to pass naturally through the pylorus with minimal force.
The Role of Assessment in Gastroscopy Training
Objective assessment is as important as practice itself. Simulation platforms that generate performance data allow trainers to track progress, identify plateau points, and adjust training accordingly.
The ASGE TESI (Training in Endoscopy Simulation Initiative) and the GAGES (Global Assessment of Gastrointestinal Endoscopic Skills) tool are both used to assess gastroscopy competence in structured training environments. Integrating these tools into a simulation curriculum creates a coherent pathway from novice to competent practitioner.
For a detailed look at how structured assessment works across endoscopy training programs, see Skills Assessment in Simulation, which reviews assessment tools and their application across multiple GI procedures.
SuzhouFrank: Supporting Gastroscopy Training Programs Globally
SuzhouFrank is a dedicated manufacturer of medical simulation equipment, providing physical training models and procedure simulators to medical schools, hospitals, and endoscopy training centers around the world. Our gastroscopy training products are designed to deliver realistic tactile feedback, anatomical accuracy, and durable performance across thousands of training sessions.
To explore our full range of GI simulation products, visit our catalogue at https://www.suzhoufrank.com/all-products#endoscopic-intervention-training-model. For program-specific inquiries, bulk pricing, or to request product demonstrations, reach out through our contact page at https://www.suzhoufrank.com/contact-us.
Conclusion
Gastroscopy training has evolved considerably over the past two decades. The move away from purely apprenticeship-based learning toward structured, simulation-supported curricula reflects both ethical imperatives around patient safety and practical recognition that simulators accelerate competence without consuming clinical resources. For trainees, the availability of realistic simulation models means entering their first supervised patient cases with a foundation of practiced technique rather than blank-slate nervousness. For programs, simulation provides a consistent, assessable, and scalable training infrastructure that traditional methods cannot replicate. As simulation technology continues to improve and evidence continues to accumulate, the integration of simulators into gastroscopy training will only deepen, making high-quality simulation resources an essential investment for any serious endoscopy training program.
References:
© 2025. All rights reserved.
About Us
Introduction
Development
Cooperation
Service
Main Products
Medical Grade Monitor
No 15, Jinyang road KunshanSuzhou, Jiangsu, China
