📞Customer Service: +86 13248368268 📧servicecenter@suzhoufrank.com one year replacement and warranty!
Hemostasis Training in GI Endoscopy Simulation
GI bleeding management requires fast, accurate hemostasis technique. Simulation-based training lets trainees practice injection, clipping, and thermal methods before high-pressure real cases.
MEDICAL TRAINING
Dr Qi Rui
3/31/20267 min read
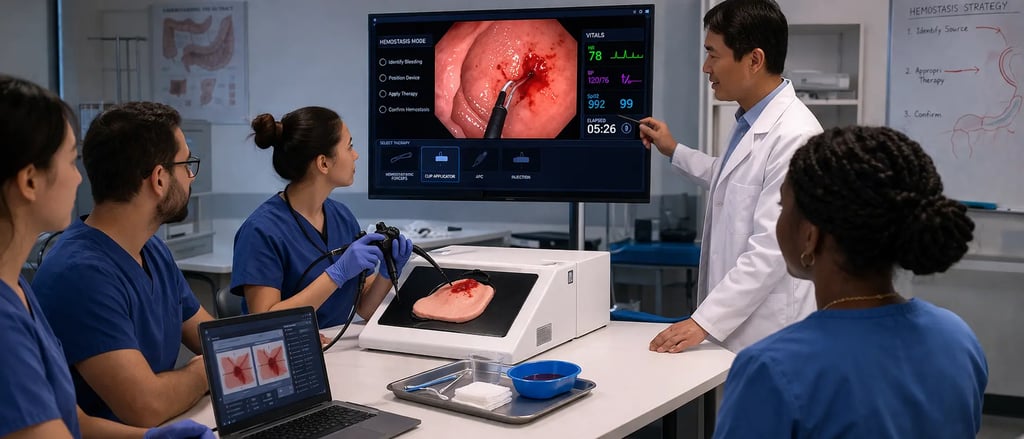
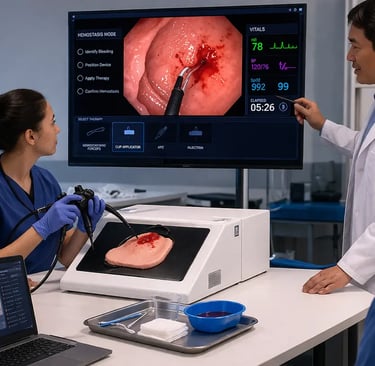
Gastrointestinal bleeding is one of the most common and potentially life-threatening emergencies encountered in gastroenterology. Whether from peptic ulcer hemorrhage, post-polypectomy bleeding, variceal rupture, or Dieulafoy lesions, GI bleeding events demand rapid, decisive endoscopic intervention. The endoscopist's ability to identify the bleeding source, select the appropriate hemostatic technique, and execute it under pressure directly determines patient outcomes.
Yet hemostasis is among the most technically and cognitively demanding skills in therapeutic endoscopy. It must be performed in a dynamic, often blood-obscured field, under time pressure, in a patient who may be physiologically unstable. These conditions make real-time learning on patients both ethically challenging and practically difficult. Simulation-based hemostasis training has emerged as an essential component of GI endoscopy education, providing a controlled environment where trainees can develop, practice, and refine life-saving skills before their first emergency case.
The Clinical Stakes of Hemostasis in GI Endoscopy
Acute upper GI bleeding has a reported mortality rate of 2–10% in hospitalized patients, with rates rising sharply in patients with cirrhosis, coagulopathy, or multi-organ failure. The success of endoscopic hemostasis in reducing this mortality depends critically on the endoscopist's technical proficiency.
Major clinical scenarios requiring endoscopic hemostasis include:
Peptic ulcer bleeding (PUB): The most common cause of acute upper GI hemorrhage, requiring injection therapy, thermal coagulation, or mechanical clipping depending on the Forrest classification of the lesion
Post-polypectomy hemorrhage (PPH): Occurring immediately or up to two weeks after colonoscopic polypectomy, requiring clip or thermal hemostasis
Variceal bleeding: Esophageal and gastric varices require band ligation or injection sclerotherapy under urgent conditions
Dieulafoy lesions: Arterial lesions that bleed massively and are often difficult to identify, requiring precise hemostatic targeting
Angiodysplasia and GAVE: Vascular lesions that may require thermal coagulation over multiple sessions
Each scenario involves different instruments, different techniques, and different decision-making pathways. Trainees cannot be expected to perform competently across this spectrum without structured practice.
Core Hemostatic Techniques in Endoscopy
Before designing simulation training for hemostasis, it is important to understand the principal techniques that trainees must learn.
Injection Therapy
Injection therapy involves delivering a hemostatic agent, typically dilute epinephrine (1:10,000 or 1:20,000 in saline), directly into or around a bleeding lesion via a sclerotherapy needle passed through the accessory channel. The epinephrine causes vasoconstriction and tamponade effect, reducing bleeding acutely.
Injection technique requires:
Accurate needle placement at the bleeding point and in multiple quadrants around it
Controlled injection volume to achieve tamponade without excessive submucosal dissection
Recognition of appropriate tissue response (pallor, elevation)
Injection alone is generally not sufficient for major bleeding from visible vessels and is typically combined with thermal or mechanical methods (dual therapy).
Thermal Coagulation
Thermal methods use electrical energy (contact probes, argon plasma coagulation) or heat (heater probe) to coagulate bleeding vessels. Contact thermal probes, including bipolar (BICAP) probes and heater probes, are applied directly to the bleeding point with controlled pressure and pulsed activation.
Thermal hemostasis requires:
Precise probe positioning on the bleeding vessel
Correct probe pressure application (firm contact to compress the vessel before coagulation)
Appropriate ESU settings and pulse duration to achieve coagulation without perforation
Recognition of adequate coagulation endpoint (vessel obliteration, surface changes)
Argon plasma coagulation (APC) is a non-contact thermal method that delivers argon gas ionized by electrical current to the tissue surface. APC is particularly useful for diffuse vascular lesions such as GAVE and radiation proctopathy, where contact-by-contact hemostasis would be impractical.
Mechanical Hemostasis: Endoclip Application
Endoscopic clips (hemoclips) are metallic clips deployed through the accessory channel that mechanically compress bleeding vessels or close mucosal defects. They are used for:
Peptic ulcer bleeding with visible vessel
Post-polypectomy bleeding
Dieulafoy lesion hemostasis
Pre-emptive closure of polypectomy sites at high hemorrhage risk
Clip application is technically demanding. The clip must be:
Oriented correctly relative to the bleeding vessel or wound edge
Opened to the appropriate diameter for the target
Advanced to precise contact with the tissue before deployment
Deployed with controlled pressure to achieve complete tissue apposition
Clip malpositioning, too lateral, too shallow, or at the wrong angle, results in ineffective hemostasis and may require multiple additional clip applications, increasing procedure time and patient risk.
Band Ligation for Variceal Bleeding
Variceal band ligation is the primary endoscopic treatment for acute esophageal variceal hemorrhage. A multiband ligator is loaded onto the endoscope tip; each band is deployed by aspiration of the varix into the ligator cap followed by band release. Precision in band placement and complete variceal capture are essential for effective hemostasis.
Why Simulation Is Critical for Hemostasis Training
The conditions under which hemostasis is performed clinically, urgency, blood in the field, physiologically unstable patient, time pressure, are precisely the conditions that make learning most difficult and error most consequential. Simulation removes these pressures from the initial learning phase, allowing trainees to develop technique in a controlled, unhurried environment.
Deliberate Practice of High-Stakes Skills
Simulation enables deliberate practice of hemostasis skills that would otherwise only be available in emergency conditions. Trainees can practice:
Identifying the bleeding point in a blood-filled field
Selecting the appropriate hemostatic technique for the lesion type
Executing injection, thermal, and clip techniques with real instruments on tissue analog surfaces
Practicing under time pressure once basic skills are established
This practice cannot be adequately obtained through observation alone. Reading about clip application and watching a supervisor clip a bleeding ulcer builds knowledge but not procedural skill. Physical practice on a simulation model builds both.
Multiple Repetitions Without Patient Exposure
Each repetition of hemostatic technique on a simulation model is one iteration of deliberate practice that does not require a bleeding patient. Over dozens of sessions, trainees develop the automatic instrument handling and decision patterns that allow them to act quickly and correctly when a real bleeding event occurs.
Simulation Models for Hemostasis Training
Physical Tissue Analog Models for Injection and Thermal Techniques
Physical models for injection therapy training use gel or silicone blocks that mimic the compressibility and flow dynamics of mucosal tissue. Trainees inject into the model and observe visual and tactile feedback indicating correct placement. For thermal training, models use materials that visibly change on exposure to heat, providing immediate confirmation of correct contact and activation.
The GI ESD Surgical Simulator from SuzhouFrank provides a physical training environment for advanced endoscopic interventions, including hemostatic techniques. Its tissue-realistic surfaces support injection, thermal, and clip training with real instruments, making it a versatile platform for upper and lower GI hemostasis skill development.
Anatomical Models for Bleeding Scenario Training
More advanced simulation platforms integrate simulated bleeding scenarios into anatomical models of the stomach, duodenum, or colon. These models present trainees with a simulated bleeding lesion in a realistic anatomical context, requiring them to:
Navigate to the bleeding source
Characterize the lesion and select technique
Execute hemostasis with the selected instrument
Assess adequacy of hemostasis
This scenario-based format is closer to clinical reality than isolated technique practice and better prepares trainees for the integrative demands of a real bleeding emergency.
VR Simulators with Hemostasis Modules
Advanced VR GI endoscopy simulators increasingly include upper GI bleeding modules with computer-generated ulcers, visible vessels, and variceal scenarios. These modules allow trainees to practice decision-making under time pressure, to experience the visual challenge of blood-obscured fields, and to receive automated feedback on technique and outcomes.
VR hemostasis training complements physical model practice: VR provides scenario variety and automated metrics; physical models provide the tactile skill development that VR currently cannot replicate.
For an overview of the endoscopy simulator landscape including platforms with hemostasis training capabilities, see GI Simulators for Training, which reviews key simulator categories and their applications in GI training programs.
Designing a Hemostasis Training Curriculum
A structured hemostasis training curriculum should progress from isolated technique practice to integrated scenario management.
Phase 1: Instrument Familiarization
Trainees learn to deploy, advance, and retrieve each hemostatic instrument, sclerotherapy needle, thermal probe, hemoclip, through an endoscope accessory channel on a bench or box trainer. No tissue interaction at this stage; focus is entirely on instrument mechanics.
Phase 2: Isolated Technique Practice
Each hemostatic technique is practiced in isolation on tissue analog models:
Injection: Needle placement, injection volume control, tissue response assessment
Thermal: Probe positioning, contact pressure, ESU activation, coagulation endpoint recognition
Clipping: Clip orientation, tissue capture, deployment mechanics, completeness verification
Phase 3: Lesion-Specific Scenarios
Trainees practice technique selection and execution for specific lesion types: Forrest Ia peptic ulcer (active spurter), Forrest IIa ulcer (visible vessel), post-polypectomy bleeding, Dieulafoy lesion. Each scenario presents a defined clinical context requiring appropriate technique selection followed by execution.
Phase 4: Integrated Bleeding Scenarios
The most advanced training phase combines navigation, lesion identification in a blood-obscured field, technique selection, and hemostasis execution in a realistic anatomical context under time pressure. This phase is most realistically delivered by VR simulator platforms with GI bleeding modules.
For guidance on structuring a simulation curriculum that integrates hemostasis training within the broader endoscopy education program, see Simulation Curriculum Endoscopy, which provides a framework for organizing training from foundational skills through advanced therapeutic competencies.
Assessment of Hemostasis Competence
Assessing hemostasis competence requires evaluation across technical and decision-making dimensions. Key performance indicators include:
Time to hemostasis: Measured from lesion identification to successful hemostasis, a proxy for both technical speed and decision efficiency
Number of techniques required: Ideally, experienced endoscopists achieve hemostasis with minimal technique switching; excessive attempts signal technical difficulty
Technique appropriateness: Correct technique selected for the lesion type and Forrest classification
Complication rate: Perforation, worsening of bleeding, or procedure abandonment
Post-procedure re-bleeding rate: In clinical cases, reflects completeness of initial hemostasis
Research published on PubMed demonstrates that simulation-based training for endoscopic hemostasis produces measurable improvements in technique execution, time efficiency, and decision accuracy when trainees are assessed during early clinical cases. The evidence base supports simulation as a standard component of hemostasis training for gastroenterology fellows and surgical endoscopy trainees.
For a comprehensive review of assessment methodologies in endoscopy simulation training, see Skills Assessment in Simulation, which covers the tools and frameworks used to measure competence across the procedural endoscopy skill spectrum.
The Global Significance of Hemostasis Training
GI bleeding is a global health problem. Acute upper GI hemorrhage accounts for approximately 400,000 hospitalizations annually in the United States alone, with comparable burdens in Europe and Asia. In lower-resource settings, mortality from untreated GI bleeding is substantially higher due to limited access to trained endoscopists and emergency hemostasis capability.
The World Health Organization's focus on safe surgical and procedural care includes endoscopic hemostasis as a key component of essential hospital service capacity. Expanding the number of endoscopists trained in effective hemostasis techniques, enabled in part by scalable simulation training programs, is an important step toward reducing GI bleeding mortality globally. For the WHO framework on safe procedural care, see WHO: Patient Safety.
SuzhouFrank: Supporting Hemostasis Training with High-Quality Simulation Equipment
SuzhouFrank manufactures medical simulation equipment designed for the full spectrum of GI endoscopy training, including therapeutic procedures like hemostasis. Our physical simulation models provide realistic tissue analogs compatible with real endoscopic instruments including injection needles, thermal probes, and hemoclips.
Explore our complete product catalogue at https://www.suzhoufrank.com/all-products#endoscopic-intervention-training-model to find simulation solutions for your hemostasis training program. For program consultation, product demonstrations, or institutional purchasing inquiries, our team is available at https://www.suzhoufrank.com/contact-us.
Conclusion
Hemostasis training in GI endoscopy simulation addresses one of the most demanding and consequential procedural competencies in gastroenterology. The complexity of GI bleeding scenarios, urgency, obscured visualization, multiple technique options, high complication risk, makes adequate training on real patients alone both ethically problematic and educationally inefficient. Simulation provides the structured environment in which injection, thermal, and mechanical hemostatic techniques can be practiced deliberately, assessed objectively, and integrated into realistic bleeding scenarios before trainees face their first unsupervised emergency. Programs that invest in hemostasis simulation infrastructure produce endoscopists who are not merely familiar with hemostatic techniques but genuinely competent in them, and that competence saves lives.
References:
© 2025. All rights reserved.
About Us
Introduction
Development
Cooperation
Service
Main Products
Medical Grade Monitor
No 15, Jinyang road KunshanSuzhou, Jiangsu, China
