📞Customer Service: +86 13248368268 📧servicecenter@suzhoufrank.com one year replacement and warranty!
Training Models in Medical Simulation: Types and Use Cases
Medical training models range from anatomical replicas to pathology-specific task trainers. Learn the main types, how they differ, and where each fits in a simulation curriculum.
MEDICAL TRAINING
Dr Qi Rui
3/16/20267 min read
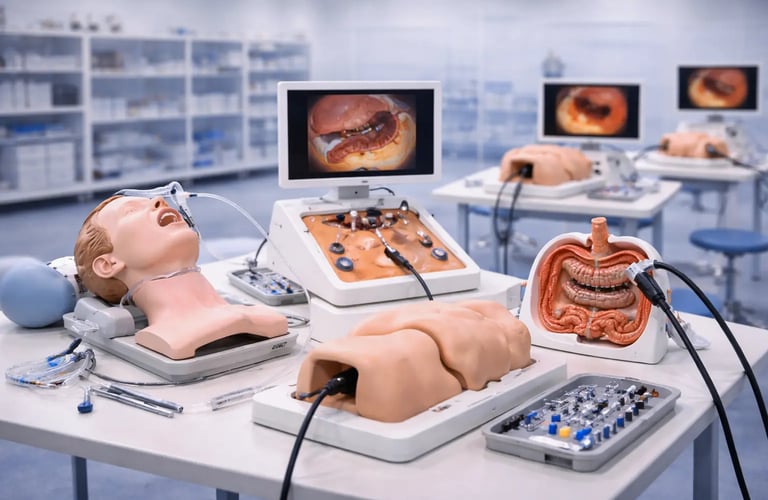
Medical simulation has transformed the way healthcare professionals are trained. At the center of this transformation sits the training model, a physical or virtual representation of human anatomy or a clinical procedure that allows learners to practice without risk to real patients. Whether it is a silicone organ replica, a full-body mannequin, or a virtual environment rendered in software, training models provide a safe, repeatable space where mistakes become learning moments rather than patient harm events.
This article defines what a training model is in the context of medical simulation, explores the major categories of models in use today, and explains where each type is most valuable in clinical education.
What Is a Training Model in Medical Simulation?
A training model is any physical or virtual construct used to simulate human anatomy, physiology, or a clinical procedure for educational purposes. The model does not need to replicate every detail of a living body, its job is to reproduce the relevant features of a specific task or scenario with enough fidelity to support learning.
Training models exist on a wide spectrum. On one end, you have simple bench-top boxes with synthetic tissue used to practice suturing. On the other, you have sophisticated high-fidelity mannequins that breathe, bleed, and respond to medications with programmed physiological changes. Most clinical training programs use a combination of models matched to the learning objectives at each stage of a curriculum.
The term is sometimes used interchangeably with "simulator," though strictly speaking a simulator can refer to a complete training system, software, hardware, and feedback mechanisms together, while a training model typically refers to the physical or representational component. In practice, the distinction matters less than understanding what a model is designed to train and how well it achieves that goal.
According to the World Health Organization's patient safety guidelines, simulation-based education is recognized as a key strategy for reducing medical errors and improving procedural competency. Models are the foundation upon which those simulation experiences are built.
Why Training Models Matter
The case for simulation-based training is well-established in the medical literature. A meta-analysis published through PubMed found that simulation training significantly improves procedural skill acquisition compared to traditional didactic instruction alone. Training models are what make that simulation possible.
Beyond skill acquisition, training models serve several practical functions:
Risk elimination: Errors made on a model carry no consequence for patients.
Deliberate practice: Learners can repeat a procedure as many times as needed.
Standardized exposure: Every trainee encounters the same anatomy or scenario.
Objective assessment: Instructors can observe and measure performance against defined criteria.
Feedback loops: Many modern models are instrumented to provide real-time data on force, technique, and accuracy.
For programs interested in structured skill development, the principles described in endoscopy training with simulators demonstrate how training models fit into broader curricula across GI and procedural medicine.
Types of Training Models
Training models can be classified in several ways: by the material they are made from, by the organ or system they represent, by the procedures they support, or by their level of fidelity. The most practical classification for educators is by use case, what is this model for, and at what stage of training is it most appropriate?
1. Anatomical Models
Anatomical training models reproduce the structure of human organs, body regions, or systems. They are used primarily for orientation and exploration, helping learners understand where things are, how structures relate to each other, and what normal anatomy looks and feels like.
Examples:
Cross-sectional torso models showing organ position
Transparent models of the GI tract
Segmented brain or spinal cord models
Vascular tree replicas for catheter navigation training
Anatomical models are widely used in early medical education and in pre-procedure orientation for trainees entering a new specialty. They do not typically simulate procedural steps, but they provide the cognitive map that makes procedural training more effective.
2. Procedural Task Trainers
Procedural task trainers are designed to simulate a specific clinical procedure or a subset of skills within a larger procedure. Unlike full anatomical models, they isolate the relevant anatomy and mechanics of a task so that learners can focus their practice.
Task trainers are among the most widely used model types in procedural medicine because they are cost-effective, highly repeatable, and targeted. A trainer designed for endoscopic submucosal dissection, for example, does not need to replicate the entire GI tract, it needs to replicate the tissue layer, the visual field, and the instrument dynamics relevant to that one technique.
In the context of gastrointestinal endoscopy, task trainers for injection, clipping, polypectomy, and hemostasis allow trainees to build specific technical skills before they encounter those situations in a live patient. You can explore how these tools are applied in detail through a discussion of simulation models in healthcare.
Common features:
Silicone or ex-vivo tissue inserts
Replaceable tissue components for repeated use
Visual access through a scope or camera
Compatible with standard clinical instruments
3. Pathology-Focused Models
Pathology-focused training models incorporate simulated disease states, polyps, ulcers, bleeding lesions, strictures, tumors, to train recognition, decision-making, and intervention. These models bridge the gap between normal anatomy practice and real clinical encounters where pathology is the reason the procedure is being performed.
Where they are most useful:
Pathology-focused models are especially valuable in:
Endoscopy training: Teaching trainees to recognize adenomas, early carcinomas, submucosal lesions, and vascular abnormalities
Radiology and ultrasound: Simulating abnormal findings on imaging
Surgical training: Practicing resection or repair of diseased tissue
When trainees first encounter pathology in a simulated environment rather than on a patient, they arrive at real cases with a baseline of recognition experience. This improves the efficiency of supervised clinical training considerably.
4. Full-Body Patient Simulators (Mannequins)
High-fidelity mannequins simulate a complete patient with programmable physiological responses. They are used in scenarios that require managing not just a procedure but a patient, including communication, monitoring, anesthesia, and team coordination.
These simulators are most commonly used in:
Anesthesia training
Emergency medicine
Intensive care
Obstetrics (for labor and delivery scenarios)
Team-based crisis resource management training
The mannequin's value is in its ability to simulate deterioration, respond to interventions, and create the full context of a clinical event, not just the technical procedure. For specialized procedural training, however, full-body simulators are often less efficient than targeted task trainers because the anatomy relevant to the procedure is not always well-reproduced in a general-purpose mannequin.
5. Virtual Reality and Hybrid Models
Virtual reality (VR) simulation uses computer-rendered environments and haptic feedback devices to simulate procedures without any physical model. Hybrid simulators combine a physical model (often for hand position and instrument handling) with a VR screen display to simulate the endoscopic or laparoscopic view.
VR and hybrid models are used across:
GI endoscopy (upper and lower)
Bronchoscopy
Laparoscopy
Urological procedures
Cardiac catheterization
The main advantages are unlimited repeatability without consumable costs and the ability to incorporate a wide library of cases, including rare pathologies that a trainee might not encounter in sufficient numbers during clinical training. The main limitations are the upfront cost and the ongoing software maintenance.
6. Ex-Vivo Tissue Models
Some of the most realistic training models use actual animal or human tissue to simulate procedures. Porcine (pig) stomach, colon, or trachea models, for example, are commonly used in endoscopy and surgical training because the tissue properties closely resemble those of human tissue.
Ex-vivo models are particularly useful for:
Advanced endoscopic procedures such as ESD (endoscopic submucosal dissection)
Practicing electrosurgical instrument control
Suturing and anastomosis training
Hemostasis techniques
The main challenges are tissue availability, biohazard management, and the inability to reuse tissue after a session. Many training programs use ex-vivo models selectively, typically for advanced learners who have already built foundational skills on synthetic models.
Matching Model Type to Learning Stage
The most effective simulation programs do not rely on a single type of model. Instead, they use a progression:
During early orientation, anatomical models and basic mannequins give learners their first encounter with spatial anatomy and instrument handling without overwhelming them. As trainees move into foundational skill building, synthetic task trainers let them drill specific procedural steps repeatedly until the motor patterns become automatic. At the intermediate competency level, hybrid simulators and VR modules add objective feedback and scenario variety. For advanced and rare procedures, ex-vivo tissue models and pathology-specific trainers provide the tissue fidelity needed to practice techniques that simply cannot be replicated in software. And for team-based and crisis training, full-body high-fidelity mannequins create the realistic clinical environment that scenario-based simulation requires.
This kind of structured progression mirrors the approach described in medical simulation in endoscopy and GI training, where skill-building is layered deliberately from fundamental technique to complex, patient-centered scenarios.
Training Models in GI Endoscopy
Gastrointestinal endoscopy is one of the specialties that has most systematically adopted training models into its education pathway. The technical demands of endoscopy, scope navigation, torque control, loop management, tissue manipulation, are well-suited to model-based practice because they involve hand skills that require repetition to develop.
Physical training models for GI endoscopy range from simple bench-top loop trainers to sophisticated anatomical replicas of the stomach, duodenum, and colon. More advanced models incorporate pathological findings such as polyps or bleeding sites and allow trainees to practice therapeutic maneuvers including polypectomy, injection, clipping, and ESD.
The GI ESD Surgical Simulator is one example of a model purpose-built for advanced GI training. It provides a realistic tissue environment for practicing the multi-step ESD technique, including marking, injection, circumferential incision, and submucosal dissection, skills that require significant repetition before they can be safely performed on patients.
SuzhouFrank: Physical Training Models for Medical Education
SuzhouFrank is a manufacturer of medical simulation equipment with a focus on procedural training across GI endoscopy, bronchoscopy, laparoscopy, and other minimally invasive specialties. Their product range includes anatomical models and task trainers designed to meet the practical training needs of hospitals, medical schools, and endoscopy training centers.
For educators building or expanding a simulation curriculum, SuzhouFrank's full catalogue is available at https://www.suzhoufrank.com/all-products#endoscopic-intervention-training-model. Direct inquiries about specific models, custom configurations, or institutional orders can be made through the contact page.
Conclusion
Training models are not a luxury in medical education, they are a necessity for building procedural competency safely. From simple anatomical replicas to sophisticated pathology-focused task trainers and hybrid VR platforms, the range of available models gives educators the tools to design progression-based curricula that prepare trainees thoroughly before they encounter real patients.
The key is deliberate selection: matching the model type to the learning objective, the learner's stage of development, and the resources available. When training models are integrated thoughtfully into a simulation curriculum, they accelerate skill acquisition, reduce early errors, and produce more confident, competent clinicians.
© 2025. All rights reserved.
About Us
Introduction
Development
Cooperation
Service
Main Products
Medical Grade Monitor
No 15, Jinyang road KunshanSuzhou, Jiangsu, China
