📞Customer Service: +86 13248368268 📧servicecenter@suzhoufrank.com one year replacement and warranty!
Endoscopy Nurse Skills: What Should Be Trained on Simulators?
Learn which endoscopy nurse skills benefit most from simulator training, from room setup and procedural assistance to emergency response protocols.
MEDICAL TRAINING
Dr Qi Rui
3/10/20266 min read
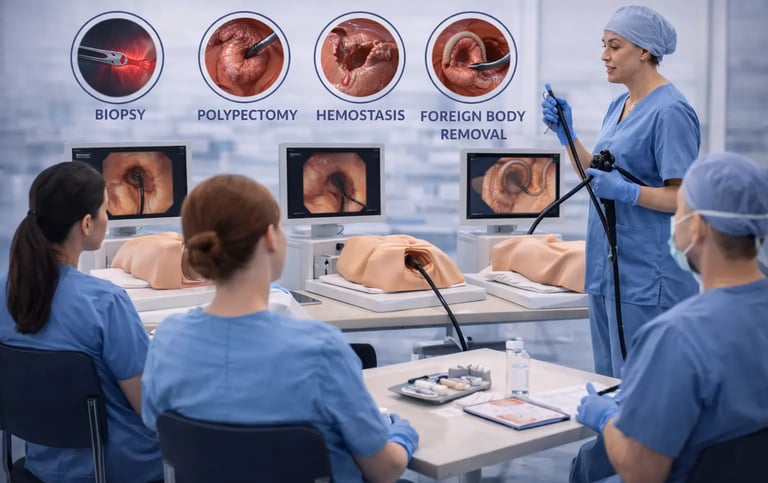
Endoscopy nurses serve as essential team members throughout every gastrointestinal procedure, from patient intake through recovery. Their responsibilities extend well beyond basic assistance, encompassing patient monitoring, equipment management, emergency response, and infection control. As endoscopy departments face increasing procedural volumes and greater procedural complexity, simulation-based training has emerged as a valuable approach for developing comprehensive endoscopy nurse skills alongside physician training. Understanding which nursing competencies benefit most from simulation helps program directors design effective interdisciplinary training curricula.
Core Endoscopy Nurse Competencies
The scope of endoscopy nursing practice encompasses multiple interconnected skill domains that collectively ensure patient safety and procedural success. Research has identified eight core competency areas for endoscopy nurses: emergency care, patient monitoring, evidence-based practice, documentation and referral, patient safety, nursing process, patient assessment, and infection control. These competencies require both cognitive understanding and practical application skills that develop through structured training and clinical experience.
Emergency care consistently emerges as the highest priority training need among endoscopy nurses. A needs assessment study of Korean GI endoscopy nurses found the largest gap between perceived importance and actual performance in emergency care competencies, ranking this domain as the top priority for continuing education. This finding reflects the reality that endoscopy emergencies, while relatively rare, demand immediate coordinated responses that nurses cannot adequately practice during routine procedures.
Patient monitoring during procedural sedation represents another critical competency area. Nurses administering sedation must continuously evaluate consciousness levels, respiratory function, and cardiovascular parameters while remaining prepared to intervene if patient status deteriorates. The dynamic nature of sedation, which can progress or regress between levels unpredictably, requires constant vigilance and rapid assessment capabilities that benefit significantly from simulation practice.
Room Setup and Equipment Preparation Skills
Effective endoscopy requires meticulous preparation before any procedure begins. Nurses must ensure all necessary equipment is available, functional, and appropriately configured for the specific procedure planned. This includes verifying endoscope functionality, preparing accessory devices, confirming medication availability, and organizing the workspace for efficient workflow.
The complexity of modern endoscopy equipment creates substantial learning requirements for nursing staff. Different procedures demand different scope configurations, accessory selections, and room arrangements. Training nurses to anticipate procedural needs and prepare accordingly reduces delays, minimizes complications, and supports overall unit efficiency.
Simulation environments allow nurses to practice equipment setup procedures without the time pressures of actual patient schedules. Training on physical simulators like the Gastrointestinal Endoscopy Simulator familiarizes nurses with scope handling, accessory insertion, and equipment troubleshooting in contexts that closely approximate clinical conditions. This foundational knowledge transfers directly to real procedural settings.
The endoscopy training guide outlines comprehensive approaches for incorporating equipment familiarity into structured nursing education programs.
Procedural Assistance and Team Communication
During active procedures, endoscopy nurses function as integral team members whose actions directly influence procedural outcomes. Effective assistance requires anticipating endoscopist needs, positioning patients appropriately, managing accessory devices, and maintaining clear communication throughout the procedure.
Team communication emerges as a fundamental skill that simulation training addresses particularly well. Research published in Frontline Gastroenterology describes Endoscopic Non-Technical Skills (ENTS) as comprising four key domains: communication and teamwork, situation awareness, leadership, and judgment and decision making. While physicians typically lead procedural teams, nurses contribute substantially to all four domains through their ongoing interactions with patients, physicians, and other team members.
Simulation training that incorporates hybrid models, where physical simulators combine with standardized patients and full team participation, creates particularly valuable learning opportunities. A review in World Journal of Gastrointestinal Endoscopy notes that learners can engage in team-based simulations within naturalistic endoscopy suite settings, building skills in communication, decision making, leadership, coordination, and crisis management. This integrated approach develops non-technical competencies alongside procedural skills.
Training programs can implement team scenarios using equipment like the Gastrointestinal ESD Surgical Simulator, which supports therapeutic procedure practice requiring close nurse-physician coordination. Nurses learn to anticipate equipment needs, respond to procedural developments, and maintain effective communication throughout complex interventions.
Patient Safety and Monitoring Competencies
Patient safety represents the overarching framework within which all endoscopy nursing activities occur. Nurses monitor vital signs, assess consciousness levels, recognize adverse events, and initiate emergency responses when necessary. These responsibilities demand both technical monitoring skills and clinical judgment capabilities.
Simulation provides unique advantages for developing emergency response competencies. Real endoscopy emergencies occur infrequently, limiting opportunities for nurses to gain experience managing critical situations through clinical practice alone. Simulated scenarios allow repeated practice of emergency protocols, helping automate appropriate responses so nurses can perform effectively under pressure.
In situ simulation, where training occurs within actual endoscopy units using portable equipment and standardized scenarios, has shown particular promise for team-based emergency training. Studies from UK endoscopy units report that nurses and healthcare assistants participating in such programs demonstrate improved confidence in managing emergency scenarios and develop shared learning with physician colleagues. Additionally, these training sessions identify latent errors in the working environment, such as missing emergency equipment or malfunctioning alert systems, that might otherwise go undetected until actual emergencies occur.
Cross-specialty simulation experience further broadens nursing competencies. Familiarity with bronchoscopy procedures through training on the Bronchoscopy Simulator Type A or Ultrasound Bronchoscopy Simulator prepares nurses to support pulmonary endoscopy services, expanding their clinical value and career opportunities.
Reprocessing Fundamentals and Infection Control
Endoscope reprocessing represents a critical infection control responsibility that requires systematic training. Proper cleaning, disinfection, and storage procedures prevent transmission of pathogens between patients, protecting both patient safety and institutional liability. Reprocessing failures have been implicated in numerous infection outbreaks, making this competency area essential for all endoscopy nurses.
While physical reprocessing skills typically require hands-on training with actual equipment, simulation can reinforce conceptual understanding of contamination risks, cleaning principles, and disinfection requirements. Training scenarios that incorporate infection control decision making help nurses understand the reasoning behind established protocols rather than simply memorizing procedural steps.
The clinical simulation guide addresses integration of procedural knowledge with broader clinical competencies including infection prevention practices.
Training Nurses Alongside Physicians
The interdependent nature of endoscopy teamwork suggests substantial value in training nurses alongside physicians rather than in isolation. Joint training sessions build mutual understanding of respective roles, establish shared mental models for procedural conduct, and develop team communication patterns that transfer to clinical practice.
European guidelines from ESGE and ESGENA explicitly recommend that GI endoscopy nurses participate actively in developing trainee skillsets by contributing to instruction in basic equipment handling, reprocessing protocols, and patient monitoring. This recommendation recognizes nurses as valuable educators whose practical expertise complements physician knowledge.
Hybrid simulation scenarios that incorporate full team participation create authentic learning environments where nurses and physicians practice together. The review in Frontline Gastroenterology describes courses involving doctors, nurses, and healthcare assistants that produced significant improvements in participant confidence across multiple ENTS domains. Participants identified strategies for improving future practice and enhanced patient centeredness as positive outcomes from this integrated training approach.
Simulation also offers opportunities to train nurses in supporting residents and fellows during supervised procedures. Understanding how to assist learners appropriately while maintaining patient safety requires practice that simulation environments safely provide. The competency training framework outlines progression models applicable to both nursing and physician education.
Implementing Nurse Simulation Training Programs
Successful implementation of simulation-based nurse training requires attention to practical considerations including equipment access, protected training time, faculty development, and curriculum design. Even modest investments in simulation resources can yield meaningful training benefits when programs are thoughtfully structured.
Low-fidelity approaches using basic manikins and portable monitoring equipment can deliver effective emergency response training within existing endoscopy units. In situ simulation requires minimal preparation compared to dedicated simulation center programs while maintaining direct relevance to actual clinical environments. Programs can begin with brief, regularly scheduled sessions that build progressively toward more complex scenarios.
Specialty-specific training expands nursing capabilities across endoscopy disciplines. Practice with the Urological Endoscopy Simulator or Hysteroscopy Simulator prepares nurses to support procedures outside traditional GI endoscopy, increasing workforce flexibility and career development opportunities.
Assessment tools support competency documentation and identify areas requiring additional training focus. The skills assessment framework provides structures for evaluating nursing performance during simulated scenarios.
About Suzhou Frank Medical
Suzhou Frank Intelligent Technology Co., Ltd., established in 2009 in Suzhou, Jiangsu Province, China, manufactures medical endoscopic imaging systems and clinical simulation training equipment. The company supplies HD, 4K, and fluorescence imaging platforms alongside comprehensive training simulators spanning gastrointestinal, respiratory, urological, and gynecologic specialties.
Training programs developing nurse simulation curricula can explore the complete product catalog featuring simulation equipment suitable for interdisciplinary team training. For equipment specifications, curriculum consultation, and institutional pricing, contact the Suzhou Frank team directly.
Future Directions in Nurse Simulation Training
As simulation technology continues advancing, new opportunities emerge for endoscopy nurse education. Virtual reality platforms increasingly incorporate team-based scenarios, while artificial intelligence systems provide automated feedback on procedural performance. These developments promise more accessible, scalable training options that complement traditional simulation approaches.
The growing recognition of nursing contributions to endoscopy safety will likely drive continued investment in nurse-specific simulation curricula. Programs that establish systematic training pathways for nursing staff position themselves for improved patient outcomes and enhanced team performance.
Conclusion
Endoscopy nurse skills encompass a broad range of competencies from equipment preparation through emergency response, all of which contribute to patient safety and procedural success. Simulation training offers unique advantages for developing these capabilities, particularly for emergency care skills and team communication competencies that cannot be adequately practiced during routine clinical procedures. Programs that train nurses alongside physicians create authentic learning environments that build effective team dynamics while developing individual competencies. Strategic implementation of simulation resources, even at modest scales, can meaningfully enhance endoscopy nursing education and ultimately improve patient care.
© 2025. All rights reserved.
About Us
Introduction
Development
Cooperation
Service
Main Products
Medical Grade Monitor
No 15, Jinyang road KunshanSuzhou, Jiangsu, China
