📞Customer Service: +86 13248368268 📧servicecenter@suzhoufrank.com one year replacement and warranty!
Medical Training: From Classroom to Simulation-Based Practice
From lecture halls to simulation labs, modern medical education relies on progressive, practice-based learning. See how simulators fit into each phase of a trainee's journey.
MEDICAL TRAINING
Dr Qi Rui
3/11/20266 min read
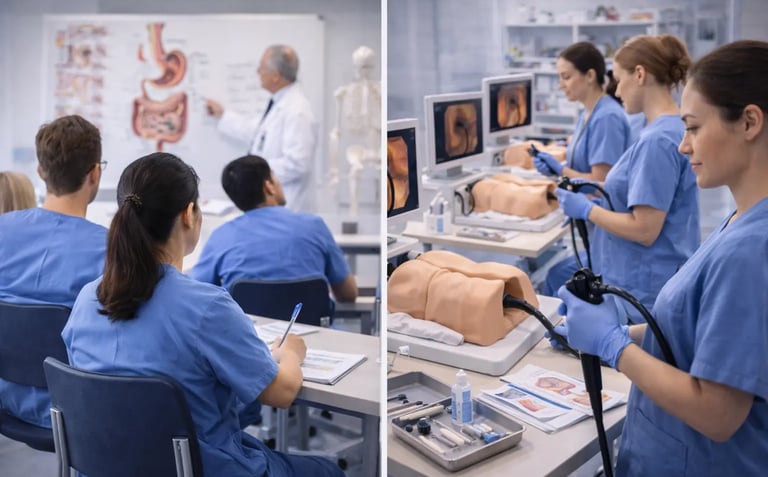
Medical education has always been built on a paradox. You cannot become competent at clinical procedures without practicing them on patients. But practicing on patients before you are competent creates risk for those very patients. For most of modern medical history, this paradox was resolved through apprenticeship, supervised practice under the watch of experienced practitioners who guided, corrected, and ultimately vouched for the trainee's readiness.
That apprenticeship model still exists, and it remains valuable. But it has significant limitations: uneven exposure to cases, variation in supervisor teaching quality, pressure to perform in high-stakes environments before foundational skills are solid, and increasingly, reduced training hours that compress the window available for skill development. These limitations have pushed medical education toward a more structured, simulation-augmented model, one that preserves the value of supervised clinical experience while filling in the gaps that traditional apprenticeship cannot address.
This article traces the stages of medical training from foundational theory through to clinical practice, and examines where simulation adds the most value in bridging the gap between knowledge and genuine procedural competence.
Stage 1: Foundational Knowledge, The Classroom Years
Medical training begins with knowledge: anatomy, physiology, pathology, pharmacology, clinical reasoning. These foundations are taught through lectures, textbooks, case studies, and increasingly, digital learning platforms. Students develop a cognitive framework for understanding disease, treatment, and the mechanics of clinical procedures.
This stage is essential, but it has a well-known limitation: knowing what to do and being able to do it are entirely different competencies. A student who can correctly describe the anatomy of the colon, the indications for colonoscopy, and the mechanics of snare polypectomy has precisely zero procedural skill until they actually handle a scope.
The gap between cognitive understanding and procedural ability is sometimes called the "knowledge-to-skill gap." Bridging it has historically required direct patient contact, which is where the risk is introduced. Simulation offers an alternative path across that gap.
Stage 2: Pre-Clinical Simulation, Building Skills Before Patients
The most important contribution of simulation to medical training is the creation of a pre-clinical skills development space. Before a trainee touches a patient, they can develop and refine motor skills, procedural sequences, and clinical decision-making in a controlled environment.
Task Training on Physical Models
Physical models, anatomical replicas designed to accept real medical instruments, allow trainees to practice procedures repeatedly and without consequence. The trainee can make errors, correct them, and repeat the sequence until the technique is reliable. This kind of deliberate practice, documented extensively in educational psychology research, is among the most efficient paths to durable skill acquisition.
For procedural medicine specifically, task training on physical models addresses skills that cannot be taught through observation or video alone:
Instrument mechanics, how to hold, advance, torque, and deflect a flexible endoscope
Tissue interaction, how instruments engage with tissue, how force is communicated through a flexible shaft
Spatial orientation, how to maintain awareness of anatomy relative to the instrument tip in three-dimensional space
Low-Fidelity to High-Fidelity Progression
Effective simulation curricula are built on a deliberate progression from low to high fidelity. A trainee beginning colonoscopy training does not start on a high-fidelity simulator with haptic feedback and automated scoring. They start with a basic physical model that lets them focus on the fundamentals, scope insertion, tip control, basic navigation.
As core competencies are established, training advances to higher-fidelity environments with more anatomical complexity, more realistic tissue properties, and more demanding procedural requirements. This progression mirrors the pedagogical principle of scaffolded learning: each stage builds on and extends the previous one.
The Medical Simulation in Endoscopy and GI Training guide provides a detailed overview of how simulation fits within the GI training ecosystem specifically, with frameworks applicable to training program design across specialty areas.
Stage 3: Supervised Clinical Practice, From Simulation to Real Patients
Simulation does not replace clinical training, it prepares trainees to make better use of clinical training. A resident who has practiced colonoscopy on a physical model fifty times before their first supervised case will navigate that first case very differently from one who has never held a scope.
Faster Skill Acquisition in Clinical Cases
Studies published in peer-reviewed journals and accessible through PubMed consistently show that simulation-trained trainees reach defined competency milestones, cecal intubation rate, procedure time, complication rate, in fewer supervised clinical cases than traditionally trained peers. This is not a marginal difference. It represents meaningful reduction in the number of patient procedures during which the trainee is operating below competency.
Reduced Patient Risk in Early Training
One of the clearest benefits of pre-clinical simulation is the reduction of trainee-related risk in early supervised cases. Trainees who arrive at their first patient cases with established instrument mechanics and basic procedural sequences make different kinds of mistakes, more nuanced, higher-level errors that their supervisors can catch and correct, than trainees who are simultaneously learning how to hold an instrument, advance it, and make clinical decisions in a complex environment.
Competency-Based Progression
Modern residency and fellowship training programs are increasingly moving away from case-count-based credentialing (a trainee needs to perform X colonoscopies before certification) toward competency-based models in which progression is determined by demonstrated skill rather than procedure volume. This shift requires objective assessment tools, and simulation provides the data infrastructure to support it.
Simulation-based assessment is covered in depth in Skills Assessment in Simulation, which outlines how structured simulation programs generate the performance data needed for competency-based credentialing decisions.
Stage 4: Advanced and Fellowship Training
Once foundational procedures are mastered, training advances to more complex subspecialty interventions. At this stage, simulation continues to play an important role, providing a safe environment to rehearse advanced procedures before performing them on real patients.
Advanced Procedural Simulation
Procedures such as ERCP, EUS, ESD, and advanced laparoscopic surgery involve skill sets that build significantly on foundational endoscopy or surgery training. The consequences of technical errors in these procedures can be severe, pancreatitis, perforation, bleeding, bile duct injury. Simulation allows fellows to develop the specific mechanics of these procedures before clinical exposure.
The Fellowship Training Advanced Endoscopy resource provides a detailed examination of how simulation is integrated into advanced endoscopy fellowship programs.
Rare and Emergency Scenario Training
Advanced simulation also covers scenarios that trainees are unlikely to encounter frequently in routine practice but must be prepared to manage: acute GI hemorrhage, perforation recognition and management, difficult anatomy variants, failed cannulation in ERCP. Repeated simulation of rare scenarios builds readiness that case-volume-based training cannot guarantee.
Stage 5: Continuing Education and Maintenance of Competency
Medical training does not end at the completion of residency or fellowship. Experienced clinicians face the same learning curves when adopting new techniques, new technologies, or new procedures. Simulation provides the same benefits for continuing medical education that it provides for initial training.
New endoscopic technologies, new imaging modalities, new ablation techniques, new hemostatic devices, require technical skill that must be acquired before clinical implementation. Simulation-based onboarding for new technologies reduces the learning curve on patients and accelerates safe adoption.
The World Health Organization has consistently highlighted skills maintenance and continuing competency assessment as pillars of patient safety in surgical and procedural care.
Where Simulation Adds the Most Value: A Summary
The stages above suggest a clear framework for where simulation contributes most effectively to medical training:
At the pre-clinical stage, simulation builds motor competence before any patient exposure, giving learners a foundation that makes their first supervised cases far more productive. During early clinical training, simulators prepare trainees for supervised cases in ways that accelerate competency and reduce the risk to patients during that initial learning curve. At the intermediate stage, simulation shifts toward competency validation, providing objective performance data that supports fair and evidence-based progression decisions. For advanced and fellowship-level trainees, simulators serve as a rehearsal space for complex interventions, allowing learners to work through difficult procedures many times before performing them under real clinical conditions. And in continuing education, simulation accelerates the safe adoption of new technologies, letting experienced clinicians build familiarity with unfamiliar instruments or techniques before using them on patients.
Building Simulation Into Your Training Program
For program directors and clinical educators, the question is not whether simulation adds value, the evidence for that is well established. The question is how to integrate simulation effectively into an existing training structure.
Key decisions include:
Which simulation tools to invest in (physical models, software-based simulators, or both)
How to structure the curriculum around defined competency objectives
How to assess and document trainee performance
How to allocate protected simulation time within a busy clinical schedule
The Simulation Curriculum Endoscopy framework offers practical guidance on these decisions specifically for GI and endoscopy programs.
Physical simulation tools, including the range of procedural training models available from SuzhouFrank, provide the hands-on training infrastructure that every well-designed curriculum requires. The GI Endoscopy Simulator and related products are designed to support training programs from first-year residents through to advanced fellowship trainees.
SuzhouFrank: Simulation Equipment for Every Stage of Medical Training
SuzhouFrank designs and manufactures medical simulation training equipment used across the full spectrum of medical education, from foundational endoscopy training through to advanced interventional procedures. Their products are used in medical schools, residency programs, fellowship training centers, and hospital-based simulation labs.
Explore the full product range at the SuzhouFrank endoscopic intervention training model catalogue, covering GI endoscopy, bronchoscopy, laparoscopy, ultrasound, and more. For program enquiries, product evaluations, or institutional partnerships, visit the contact page.
Conclusion
The trajectory of medical training, from classroom theory to simulation-based practice to supervised clinical work and beyond, is not a linear march through disconnected stages. It is an iterative, scaffolded process in which each phase prepares the learner for the next. Simulation occupies a critical position in that process: it is the mechanism by which the knowledge-to-skill gap is bridged safely, efficiently, and at scale.
Programs that invest in structured simulation infrastructure at every stage of training produce clinicians who arrive at patient care better prepared, progress more quickly, and ultimately deliver safer, more effective care. That is not an aspiration, it is what the evidence consistently shows.
© 2025. All rights reserved.
About Us
Introduction
Development
Cooperation
Service
Main Products
Medical Grade Monitor
No 15, Jinyang road KunshanSuzhou, Jiangsu, China
